
Do you often experience digestive stress after eating certain foods?
Can the discomfort be so severe that it affects your day-to-day activities?
The link between foods and digestive disorders is well recognised, and there is a good chance that FODMAPs – small carbohydrates in certain foods – may be the culprit.
As a food intolerance dietitian, I’ve seen how remarkable a low-FODMAP diet can be for people with chronic gastrointestinal symptoms… things like recurrent bloating, gas, cramps, diarrhea or constipation. This diet is one of the natural ways known to alleviate such chronic symptoms.
There’s also many new case studies suggesting it can help manage symptoms of other health issues too.
If you’re keen to learn more, and maybe even try a low FODMAP diet for yourself, this 3,000 word beginner’s guide is a great place to start.
Note that each section in this article has a ‘summary’ box (like this one) to save time. Below this box is a contents menu to help you navigate directly to a particular section.
What Are FODMAPs?

A low FODMAP diet is also known as a FODMAP elimination diet.
This is a temporary eating pattern that has a very low amount of food compounds called FODMAPs.
The acronym stands for:
- Fermentable – meaning they are broken down (fermented) by bacteria in the large bowel
- Oligosaccharides – “oligo” means “few” and “saccharide” means sugar. These molecules are made up of individual sugars joined together in a chain
- Disaccharides – “di” means two. This is a double sugar molecule
- Monosaccharides – “mono” means single. This is a single sugar molecule
- And Polyols – these are sugar alcohols (however, they don’t lead to intoxication!)
As you can see, there are four main saccharide groups that make up FODMAPs – oligosaccharides, disaccharides, monosaccharides and polyols.
These FODMAP groups have specific names and may also have more than one group within them, known as a FODMAP subgroup:
- Oligosaccharides have two subgroups, known as fructans and galactans (or galacto-oligosaccharides or GOS for short)
- Disaccharides are known as lactose and only contain one group
- Monosaccharides are known as fructose (or excess fructose) and also only contain one group
- Polyols have two subgroups, known as sorbitol and mannitol
Let’s stick with the term FODMAPs shall we?
Those saccharides and polyols are short-chain carbohydrates that, if poorly digested, ferment in the lower part of your large intestine (bowel).
This fermentation process draws in water and produces carbon dioxide, hydrogen, and/or methane gas that causes the intestine to stretch and expand.
The result is strong pain, bloating, visible abdominal distension and other related symptoms (1).
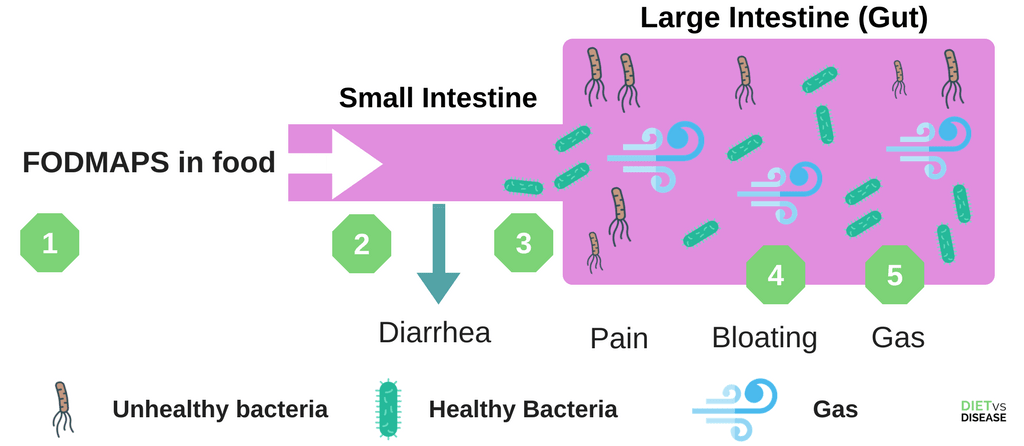
- Food is eaten that contains FODMAPs.
- Some FODMAPs may pull water into the small intestine, causing diarrhea
- In those with IBS, FODMAPs can travel to the large intestine (gut) largely undigested.
- When “unhealthy” bacteria interact with FODMAPs in the gut, it causes a range of symptoms such as bloating, gas and pain.
- Different people are sensitive to different FODMAPs, so it’s important to identify which ones are the culprit.
This is a video training I made that explains FODMAPs and the low FODMAP diet if you prefer to watch instead of read:
What is a low FODMAP diet?
The primary use of this diet is to relieve digestion-related symptoms, but is emerging as a useful tool for several other conditions too.
It can be useful for those with:
- Irritable Bowel Syndrome (IBS)- more on that below
- Other forms of Functional Gastrointestinal Disorder (FGID)
- Small intestinal bacterial overgrowth (SIBO)
- Certain auto-immune conditions/diseases like (potentially) rheumatoid arthritis, multiple sclerosis or eczema
- Fibromyalgia or other health issues you’ve noticed are triggered by certain foods
- Frequent migraines that appear to be triggered after certain meals
- Inflammatory bowel disease (IBD) such as Crohn’s disease, ulcerative and microscopic colitis.
The best candidates for trialling this diet also tend to answer yes to these questions.
And note that it’s not to be confused with a food chemical intolerance such as a low Histamine Diet or a low Salicylate diet.
Summary: FODMAPS are short-chain carbohydrates that, if poorly digested, ferment in the bowel to cause severe digestive stress. This diet is designed to temporarily restrict the amount of FODMAPs consumed and is useful for treating conditions like IBS.
The “What Can I Eat on a FODMAP Diet?” food list
This is a giant list of what foods to eat, and what foods to avoid when following a low FODMAP diet.
It’s based on the latest published FODMAPs data (7, 8, 9, 10, 11).
It looks like this:
You can download a large and printable 4-page PDF version now by tapping the blue button below:
Many legumes not included on this list (such as chickpeas and lentils) can be made far more digestible and low FODMAP by pre-soaking for 7-24 hours.
Also note that like with anything food related, portion size is fundamental. A serving of 10 almonds are considered low FODMAP, but if you eat 20 almonds then you will end up eating a high amount of FODMAPs.
As with anything we eat, the dose makes the poison.
Summary: Above is a list of high and low FODMAP foods that you can take with you when grocery shopping. Remember that many of these foods still contain trace amounts, so portion size is fundamental.
Common FODMAPS and what to look for on the label

Common FODMAPs in your food include:
- Fructose: A sugar found in most fruits and vegetables.
- Lactose: A sugar found in dairy foods like milk.
- Fructans: A chain of sugars found in many vegetables and grains.
- Galactans: Found primarily in legumes.
- Polyols: Sugar alcohols like sorbitol and mannitol. You find them mainly in artificial sweeteners and chewing gum but they are also naturally occurring in various fruits and vegetables.
The Monash University low FODMAP diet phone app is a great place to start when reading food labels.
You can check the app for foods that have been tested as high FODMAP.
It’s also useful to know other common high FODMAP ingredients such as inulin (chicory root), natural flavors, high fructose corn syrup, agave, honey, etc so you can avoid them also.
Is Gluten a FODMAP?
While gluten can also trigger food sensitivities in a handful of people, it is a protein, not a carbohydrate.
Therefore gluten cannot be classified as a FODMAP.
However, gluten-free products do still appear beneficial for those with FODMAP sensitivities. Testing from Australia’s Monash University shows that gluten-free products almost always have reduced amounts of fructans and oligosaccharides.
This is because gluten and FODMAPs often co-exist in the same product e.g. wheat bread and pasta.
So by choosing gluten-free products means that they are also more likely to be lower in FODMAPs, and free of gluten of course.
Summary: FODMAPs exist mainly in dairy, legumes, and many fruits and vegetables. While gluten is not technically a FODMAP, gluten-free products are typically lower in FODMAPs anyway.
A low FODMAP diet is very restrictive and designed to be temporary

Before we go any further, it’s important to clarify that following a low FODMAP diet is very restrictive and cuts out numerous common foods and food groups.
That means you need to reintroduce foods at some stage, so it cannot be a permanent solution.
The idea is that restricting all FODMAPs at once should have a far greater and more consistent effect than simply restricting one FODMAP in isolation. By reducing all high FODMAP foods, your intake of FODMAPs will reduce to a level where you no longer get symptoms.
How it works
There are three phases of the low FODMAP diet.
- Phase 1 – Elimination/Strict low FODMAP Diet: For 3-8 weeks (depends on how you respond) you strictly exclude all high FODMAP foods from your diet.
- Phase 2 – Reintroduction/Rechallenge: You will reintroduce each FODMAP group one at a time to see what triggers symptoms. For example, you may first reintroduce fructose for three days. If you have no symptoms, you may then reintroduce lactose too, and so on.
- Phase 3 – Modified/Adapted FODMAP Diet: Once the trigger FODMAPs have been identified, you will know what you can and cannot eat. You can then use this information to formulate your own personalised diet that keeps your symptoms to a minimum.
Summary: This diet is not designed to be permanent. It is highly restrictive for several weeks, before foods are slowly reintroduced to determine what causes symptoms.
IBS and studies that support a low FODMAP diet

Much of the research has been on patients with Irritable Bowel Syndrome (IBS).
IBS is a chronic gastrointestinal disorder characterised by abdominal pain and altered bowel habits, and around two thirds of IBS patients report their symptoms are related to food.
It’s now estimated to affect 11% of the population globally, up to 13% in Australia and up to a whopping 20% in the US and UK (2, 3).
One landmark clinical trial compared the responses of 39 IBS patients who received standard healthy eating advice against 43 IBS patients who received low FODMAP training from a dietitian (13).
Can you guess what diet is best for IBS?
I’ve illustrated some of the results here below in this chart. The black bar represents those in the standard diet advice group, the pink bars are those in the low FODMAP group.
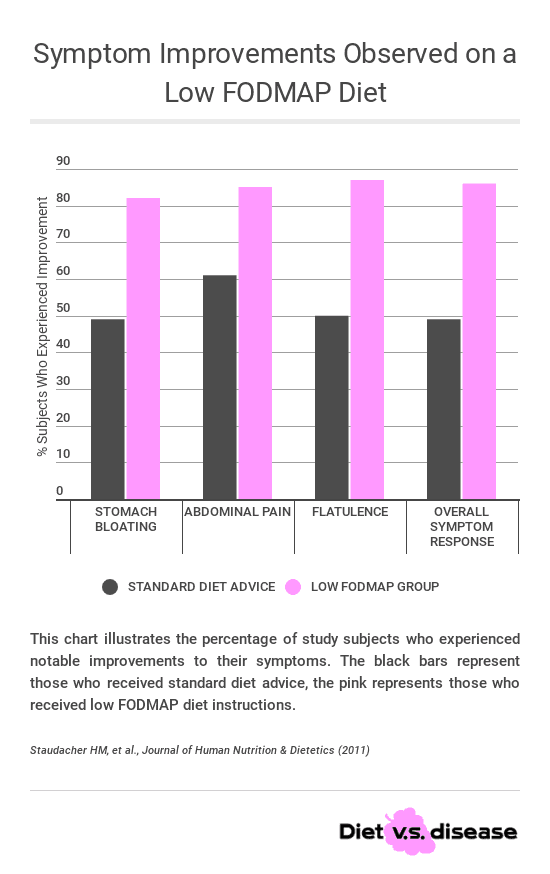
While diet changes helped for both groups (as expected), the number of subjects who experienced an improvement in IBS symptoms was far greater in the low FODMAP group compared to the standard group.
Basically almost 9 out of every 10 people on the FODMAP diet had huge improvements in bloating, stomach pain, flatulence and their overall symptoms.
Another high quality study was an Australian clinical trial that compared the effects of a low FODMAP diet between 30 IBS patients and 8 similar individuals without IBS (to act as a control group for comparison) (4).
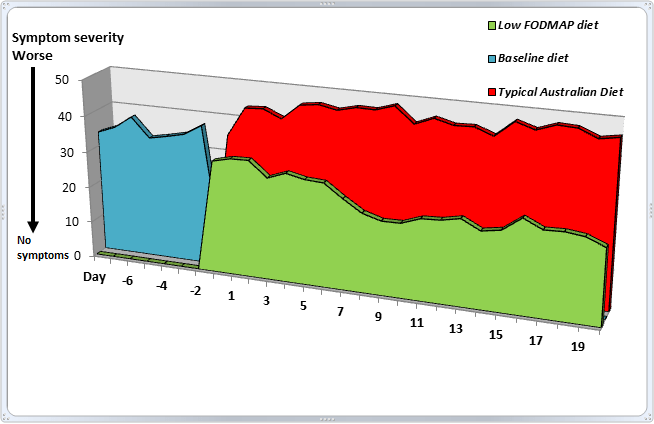
Participants were randomly assigned to receive either a diet low in FODMAPs (less than 3 grams per day) or a typical Australian diet for 21 days. This was followed by a long “washout period”, before crossing over to the alternate diet for another 21 days. Almost all food was provided to the participants, and breath hydrogen and stool samples were collected frequently.
This is what happened:
Click to enlarge.
IBS symptoms were reduced by 50% overall on the low FODMAP diet, with the greatest improvements observed one week after implementing the diet. More specifically, improvements were seen for bloating, abdominal pain, wind and dissatisfaction with stool consistency.
Numerous similar studies (albeit not as well designed) have found very similar benefits, and the overall average success rate is about 68-76% of patients (5, 6).
Research in this area still has a way to go, but many doctors now recommend it as the first dietary approach for treatment of recurrent gastrointestinal issues.
Summary: Controlled trials continue to find that a well-designed and supervised low FODMAP diet improves symptoms by about 50% in as little as one week. The average success rate is 68-75% of patients that try it, based on the studies mentioned above.
Low FODMAP recipe ideas
Appropriate recipes are those low in total FODMAPs, yet still nutritious and simple to make (and delicious of course).
To save you time searching around all day, I’ve compiled a roundup of low FODMAP recipes for mains and snacks that are not only family-friendly, but easy to bring to work too:
- 25 Scrumptious Low FODMAP Breakfast Recipes To Start Your Day
- 25 Tasty Low FODMAP Lunch Recipes For IBS
- 30 Delicious Low FODMAP Dinner Recipes: Don’t Get Stuck Eating The Same Thing!
- 77 Easy and Tasty Low FODMAP Snacks: You Don’t Have To Miss Out
- 30 Delicious Low FODMAP Vegetarian And Vegan Recipes Plus Some FAQ
Probiotics may help ease symptoms but it’s unclear

Recent data suggests there is a strong link between the balance of our gut bacteria (called the gut microbiota) and health.
An imbalance of this bacterial “community” – known medically as gut dysbiosis – can cause many problems… especially gut issues.
Probiotics is the term used to describe the bacteria we eat specifically for to restore this balance and improve health.
So how does this relate to FODMAPs?
Growing evidence shows that many subgroups of IBS patients have a highly irregular gut bacterial environment (7).
The question posed now is will the addition of “good” bacteria – from probiotics – help to manage FODMAP sensitivities? The research is promising, and I’ve written a detailed review and guide here.
Essentially from that review it appears that the probiotic supplements VSL#3, Symprove and Align/Alflorex are the most useful. If you are predominantly dealing with occasional irregularity then look for a probiotic with a mixture of Lactobacilli species.
Whole food sources of probiotics include fermented foods like quark, kefir yoghurt and pickled vegetables such as sauerkraut. Apart from the fact that many of these probiotic containing foods are high FODMAP and so are not well tolerated by many, there are several potential problems relying on whole foods for probiotics.
For example, each batch of food will vary in their active probiotic strains and concentration. Additionally, fermented foods are rich in food chemicals like salicylates and histamine, which some people may also be sensitive to (9).
This fact should be considered on an individual basis.
Summary: Poorly absorbed FODMAPs are thought to directly upset the bacterial balance in our gut. In line with this theory, regular probiotic supplementation has been shown to effectively reduce symptom severity in IBS patients. I suspect that the addition of probiotics to a low FODMAP diet will be very beneficial.
A low FODMAP diet plan and dining out ideas

Diet plans are generally tailored to individual patients as we all have different eating habits and preferences.
However I have put together a sample 7-day diet plan that you can see here in more detail.
There are also pre-packaged foods formulated to be low in FODMAPs if you prefer the convenience.
For example, Fodmapped products is the world’s first dedicated FODMAP brand and is available for sale in Australia, the UK and more recently, the US.
Here is a low FODMAP food list of common products found worldwide.
Low FODMAP dining out ideas

Set meal plans aren’t particularly useful when you’re eating out at a restaurant or takeaway shop. Here are some food choice tips to help you make appropriate choices:
- Café: choose tea or coffee with lactose-free or almond milk, poached eggs on sourdough or gluten free bread with grilled low FODMAP vegetables, lactose-free yoghurt with low FODMAP fruit (Greek yogurt or quark is okay too but still has some lactose), smoothies made with lactose-free or almond milk and low FODMAP fruits and vegetables
- Pub food: choose plain meat, chicken and fish with low FODMAP salad or vegetables, olive oil and lemon juice as a dressing, fries with plain salt
- Asian: choose stir fries with no onion or garlic, sushi, sashimi or rice paper rolls
- Mexican: ask for no onion, garlic, beans and sour cream on corn nachos or tacos
- Italian: choose gluten free pasta and ask for an accompanying sauce that does not contain onion or garlic, or ask for a salad with plain meat or chicken with olive oil and lemon juice as a dressing
- Fast food: choose fries with plain salt
- Cinemas: choose popcorn and water
Summary: At the beginning of a low FODMAP diet it’s much easier if you prepare your own meals at home, just to get familiar. And while it can seem overwhelming at first, trends start to emerge between what you can eat at home and dining out.
DIY or do I need help from a Dietitian?
As you can see the low FODMAP diet is complex.
This is generalised advice and may be difficult to do yourself without professional guidance.
Group education sessions have recently been used with success, but it’s traditionally done in a one-on-one setting so that any diet modifications are individualized. In fact, the diet has only ever been evaluated formally as a dietitian-delivered diet (12).
For this reason it’s recommended to do this under the guidance of a dietitian where possible.
That said, with the quality of resources now available online it certainly can be done on your own, but you must be highly motivated and disciplined.
I recommend you to buy the Monash University Low FODMAPs app (we have no affiliation). Monash is the world’s leading source of FODMAP research and information (from Melbourne, Australia), and their app is worth every penny.
Consider probiotics as well either before you start the FODMAP diet or after you have finished. Also speak with your doctor or dietitian first just in case you require medication.
Safely removing and reintroducing the appropriate foods takes a lot of learning upfront, but countless patients can tell you it’s worth it.
Would you like personalized support with this?
We offer a concierge-level service where we walk clients through the entire gut healing process, from the nutrition to the behavior and psychology and more.
This is a premium service we’ve been running since 2019 and I’m confident it’s the absolute quickest way to resolve symptoms and heal your gut in a sustainable way.
To apply with us please fill in this form and schedule a nutrition assessment call with one of our specialists, where we can determine if we can help you and explain what options are available.
The “What Can I Eat on a FODMAP Diet?” food list
This is a giant list of what foods to eat, and what foods to avoid when following a low FODMAP diet.
This is how it looks:
You can download a large and printable 4-page PDF version now by tapping the blue button below:
Frequently Asked Questions About The Low FODMAP Diet
What protein powders are low FODMAP?
Whey protein isolate (WPI) is low FODMAP at 40 grams. Whey protein concentrate (WPC) may not always be low FODMAP depending of the lactose content.
Rice and pea protein are vegan protein powders that are low FODMAP at 40 grams (2 tablespoons).
Just also check that the protein powder doesn’t contain any other high FODMAP ingredients.
For more detailed information on picking a low FODMAP protein powder see this article.
Can I still do The Low FODMAP Diet if I’m a Vegetarian or Vegan?
Yes of course, but it can be more tricky because many staple vegetarian and vegan protein options are high FODMAP.
This includes legumes, some nuts and soy products.
Low FODMAP vegetarian and vegan protein options include:
- Firm tofu (2/3 cup cubed, 160g)
- Tempeh (100g)
- Quorn mince, no onion (75g)
- Eggs (2 eggs, 117g)
- Some nuts and seeds (refer to this low FODMAP food list for specifics)
- Canned and rinsed chickpeas/garbanzo beans and butter beans (1/4 cup, 42g)
- Canned and rinsed lentils (1/2 cup, 46g)
- Quinoa (1 cup cooked, 155g)
- Soy protein milk (1 cup, 250ml)
- Lactose free cow’s milk (1 cup, 250ml)
- Lactose free yogurt (1 tub, 170g)
- Greek yogurt (4/5 cup, 200g)
- Hard yellow cheese e.g. cheddar, Colby, Swiss (2 slices, 40g)
- Cottage cheese (4 tablespoons, 36g)
- Soy cheese (2 slices, 40g)
Can I Cook With High FODMAP Foods and Then Just Remove Them?
Yes and no. Let’s start with the no.
Unfortunately, most FODMAPs mix with water (known as water soluble). This means mixing high FODMAP foods with other ingredients when cooking could see the FODMAPs leach into the low FODMAP food (virtually every other ingredient or food contains water). Cooking with garlic and onion is the main example when this occurs.
It’s thought that high temperature cooking can breakdown FODMAPs (potentially favorable), but to what extent is not yet known. Therefore, currently the best way to keep your meal low FODMAP is to cook with only safe ingredients.
There is an exception, which is why I said “yes” in the beginning.
Cooking with garlic and/or onion in oil is safe as long as you remove all pieces before you add any other ingredients. While FODMAPs mix with water, they do not mix with oil (much like water does not mix with oil, if you ever drop oil into water you will see).
So for example, you can cook whole garlic cloves in oil, which allows the flavor compounds to mix with the oil but not the FODMAPS. Then remove the garlic from the oil before adding any other ingredients (so keep the garlic pieces large so they are easy to remove). This leaves you with what is essentially garlic-infused oil, which is low FODMAP.
More on IBS, FODMAPs and related topics
- Best Remedies, Medicine, & Low FODMAP Products For Stomach Pain and IBS
- 7-Day Low FODMAP Diet Plan For IBS
- FODMAP Reintroduction Plan and Challenge Phase: Your Guide and FAQ
- The “Eat This, Not That” FODMAP Foods List
- Best Probiotics For Irritable Bowel Syndrome (IBS): Explained in Plain English
- How To Stop Diarrhea: Diet Changes and Natural Remedies
- 11 Warning Signs You Have A Sneaky Food Intolerance


Hi Your comment that a low fodmap diet should be only temporary is entirely unfounded.
I have had such remarkable health results from it that I intend staying on low fodmap for good.
For thirty five years I had an almost permanent mild headache which weekly would morph into a migraine.
At the same time I had a bad back which at times hospitalised me or put me into bed for a week at a time.
After years of fruitless visits to doctors and many kilos of pain pills I decided to try the fodmap diet, my reasoning being that my problems could perhaps be inflammation related.
Within three weeks I was cured of both problems with no recurrence six months later.
I eat fish, meat, eggs, masses of green vegies and the allowed varieties of fruit. In what way is this restrictive?
There is always exceptions to any blanket statements.
Keep in mind this article is for the general public, the individual who does not know anything about FODMAPs yet. Low FODMAPs in this article means all FODMAPs excluded during the first phase.
For the vast majority of users, a low FODMAP diet (limiting *all* FODMAPS) is temporary. And most certainly restrictive of how the general population eats.
Once the problem foods are discovered, you reintroduce the food groups you tolerate. From that point on it does not get labelled a low FODMAP diet (even though it is in some aspects). It’s just your diet.
I’m very happy you found out what works for you.
I love your attitude Vaughan! I am about to help my 19 year old start on this and was looking for positive words like this! I would love to hear any secrets you have.
Thanks so much for sharing, Joe. This is one of the most thorough and helpful explanations of the low-FODMAP diet I’ve seen!
Thanks Joyce!
Hi, I have a question regarding the artificial sweetener Swerve. Can someone on this diet use this substitute for table sugar? It’s an erityrol and olgliosccharides product derived from fruit and vegetables.
Unfortunately no, oligosaccharides. But if you already have tested yourself and you know you are not intolerant to them, then you could use it. But if you are just starting the low FODMAP, go with stevia
Thanks…it’s for my husband. Recently diagnosed with colitis. I am diabetic and have swerve and stevia in my house…we will go with stevia for him. This is so new to us, the information on your page helped spell out some of the guidelines for us
Hi,
Is there any “increasing order” suggested list of low FODMAP foods?
Suppose I want to eat a 3-4 Oz dish, what is the lowest FODMAP dish among the list: rice, oats, potatoes, tapioca, grits(corn),quinoa?
I’m looking for some sort of answer like:
rice<potatoes<oats<quinoa<tapioca… etc.
I would appreciate any help in finding a source/answer to this.
Thank you very much!
Dan
Hi Dan the best thing for that is to download the Monash FODMAPs app. It’s about $10 in the appstore, totally worth it
Thank you for all of this information, I am beginning this diet. I cook Italian and the thoughts of no garlic is a bit disturbing…………I’m ok without pasta……….I have found some info that says “garlic powder” is ok, but I’m not certain I want to take this risk. Appreciate your thoughts. Thank you, Sandi
Use garlic infused olive oil. FODMAP free
How about xantham gum, gellen gum, and other “gum” preservatives found in processed foods? I have noticed that most almond milks have these in them as well as gluten free products. Is it okay to eat these? Or are they also bad for people following the low FODMAP diet? Thank you for your helpful article!
I was curious about this too, I’ve been sticking to gluten free snacks but recently a gluten free snack really flared up my ibs. The almond milk that I have tried made me feel a bit sick too. I am not lactose intolerant and have no problems drinking that even though I do have ibs. Although I’m not sure if it effecting me adversely.
What about coconut sugar? Is it acceptable on low FODMAP?
I have a question about the diet. I keep reading that it’s a temporary elimination diet. I know already that there are a lot of foods that give me symptoms, so couldn’t I just try to avoid all high fodmap foods permanently?
Someone already asked this question at the start and joe mentioned this in his video too. Check it out.
Hi – you’ve recommended carrot and cucumber sticks **with hummus** in your list of dining out ideas, but isn’t hummus usually made with garlic?
True. I’m confused with hummus but plain hummus getting bored n I go for red pepper hummus so yummy. I love it. I don’t know it ok to use??
Hi,I’m wondering if you can help me. I’ve been diagnosed with acid reflux and it has been suggested that I should try a low FODMAP diet. Having looked at the list of foods available to me, I noticed many of them are a common trigger for reflux. Is there anything you could suggest to help me.
Take 1/2 lemon juice in warm water first thing in the morning! Do this as many days as you possibly can. I got read of years of acid reflux! Never needed another pill again. Good luck!
I am surprised and dismayed at the sentence “Ask for gluten-free bread (preferably spelt or sourdough)”. It is bad advice. Spelt is not gluten-free. Like kamut, people think it is but it isn’t.
Yeah, there are other conflicting pieces advice in the “Low FODMAP Dining Out Ideas” section as well. For instance…”Sushi and sashimi with soy sauce and wasabi”. Soy sauce’s (Kikkoman brand) second ingredient is wheat…ahead of even soy beans.
Soy sauce is not gluten free (unless it is labeled as such, and it’s not easy to find), and it is not low in FOMAPs.
Hello! I was recently diagnosed with (EPI – Exocrine Pancreatic Insufficiency) I was just put on Creon and it seems to help but sometimes i get the same symptoms. So I have been looking into the low FODMAP diet. I also have polycystic kidney disease so I shouldnt use alot of salt. I have many other health issues (Reflex Sympathetic Dystrophy, Fibromyalgia, Chronic pain just to name a few) my dr isnt really helping me so Im teying to come up with something. Just alot to try to figure out.
Hi, I have just found your post and found it very helpful, but I have a couple of questions. Do you have a link that I can go to that tells what foods are in each group? For example, i know that pears have polyols and fructans, so if testing polyols, it’s not a good one to try. Also, do you have to test EVERY food in each group, or if you have a reaction to one fod in that group, then they are all out? Hope this makes sense!
The Monash App does the job. Join the dietvsdisease support group on FB and you will get answers from other members who are also going to lhrough same or similar conditions and have tried the app. Also Joe monitors the group as it’s his.
Hi,
How much meat example: ground turkey or chicken can you eat a day. I did not see any measurements next to that part. Thanks so much for any assistance you can provide.
Hi Amber meat does not contain FODMAPs. Only plant-based foods and ingredients
I have had stomach problems since I was about 9 yrs. old. I just turned 60. Every time I got tested the Dr. would say tests came out negative. I have battled deep terrible thoughts with depression since I was a young girl too. I recently started getting awful anxiety attacks. Also diagnosed with Fibromyalgia a few years ago. Stomach problems have affected me holding down jobs & even going out. I found your website today. Did I find a connection?! It is extremely difficult to wake happy every day when you are tired & know your stomach may be sick 3 or 4 times that day. Sometimes more. I have seen diets that have 1/2 the selection of food! I am going on this diet & feel hopeful. Thank you!
Good luck Cari. If you join the diet vs disease support group on FB, you will have great support from others who suffer similar condition. It’s Joe’s support group so he does monitor and reply in there too.
You may want to rethink the advice about probiotics in light of the recent British Dietetic Association systematic review of systematic review and evidence-based practice guidelines for the use of probiotics in the management of irritable bowel syndrome in adults (2016 update)
Practical considerations
Individuals with IBS can be advised that, despite numerous probiotic RCTs, there is insufficient good evidence to recommend any specific probiotic product and, independent of IBS-subtype, improvement in all symptoms is unlikely.
There are many probiotics available with different preparations, bacterial strains and doses. Individuals with IBS who choose to try probiotics should be aware that some products contain ingredients that may increase IBS symptoms [dietary fibre, fermentable oligosaccharides, disaccharides, monosaccharides and polyols (FODMAPs)]. If an individual finds a probiotic beneficial after 4 weeks, he/she can be advised that the long-term effects of continued use are unknown.
http://onlinelibrary.wiley.com/doi/10.1111/jhn.12386/abstract;jsessionid=66EF23D210BA8C611D6B0AF128209D21.f02t01?userIsAuthenticated=false&deniedAccessCustomisedMessage= The
And it might be useful to put a comment indicating that the most reliable source of information on the FODMAP content of foods is the Monash University GI department phone app. The Monash GI group developed the diet. The app cost about $9. Updates are free. And all of the money goes to support IBS research and improvement of the FODMAP diet
http://www.med.monash.edu.au/cecs/gastro/fodmap/iphone-app.html
I have a question: Is it okay to flavor things with onion and garlic as long as you don’t actually eat the onion and garlic? For example, putting a whole clove of garlic in vinaigrette to flavor it then removing it after letting it set awhile or putting half a slice of onion in a pot of green beans while cooking them, then removing the onion.
@Tom Andersen. The fructans are water soluble. As such, they will leech out in your vinaigrette. They are not fat soluble however. So you can add big pieces of garlic and onions to a stir-fry (before adding the veggies ect) and then remove these pieces before adding other ingredients. Keep in mind that veggies etc contain water which can make the fructans leech out.
Just FYI: I am a registered dietitian at NutriHeal (Mauritius) specializing in naturopathic treatments for GI and hormonal issues. One of my patients asked me my opinion about this website.
Hi,
Thank you so much for this post! I started GAPS about 20 days ago, and although it has made me feel better, I still have stomachaches, feel bloated and struggle with gas etc. At this point I realized that I probably have problems with fodmaps. I put garlic and onions in all my soups which is probably the reason why they make me feel bad afterwards. It makes so much sense now! I will try to stay on GAPS while only eating low fodmaps and see how it goes. Combining those two diets will be hard and restrictive, but I have such a strong will to finally heal my body.
My question is: Do the amounts for the low fodmaps food on your shopping list count for one day, or a week? How does it work?
Thank your so much!
Tina
Per serving actually. But when you starting in the first week, per day would be a good safe way to start
TESTIMONY OF HOW I GOT CURED FROM FIBROMYALGIA
This is real take it serious, who will believe that herbs can cure fibromyalgia, i never believe it will work, i have spend a lot, getting drugs from the hospital to keep me healthy and release me pain, but it got to a time when there was nothing left in me again because i was so broke,one day a friend introduce this great herbal medicine home called perfecthealthherbalmedicinehome,own by DR SITTHU who is well known for curing different deadly diseases, i decided to email him (perfecthealthherbalmedicine @ gmail. com), but I never thought herbals can cure fibromyalgia, though I just wanted to give him a try, he replied my mail and Needed some Information about me, then I sent them to him, then i purchased herbal medicine cure for fibromyalgia and he sent it through Courier Service, the Courier Office told me that 2-3 days I will receive the package and when i received the herbal medicine, i took the medicine as prescribed by him.i used it for 6 weeks,all my symptoms disappeared,then went for medical check up,for confirmation,surprisingly after medical check up the doctor confirm fibromyalgia free, i thought it was a joke, i will never stop thanking you for saving my life, I will always testify your good works. if you are fibromyalgia patient, contact him and you will be cured permanently…for more information about him check his website (www. . weebly. com)
Do you know if colostrum-LS contains FODMAPS?
I want to share my experience since starting the fodmap diet.
My life has totally changed for the good!
I’m lucky that my body responds quickly to changes and within the first week I was feeling more energized and noticing a difference in my bowel movements. They were so normal. (I had forgotten what normal was) And I started to fart again. What a great sign of a healthy gut.
I also discovered a few new things: I can’t eat peanuts or almond milk. They both give me severe abdominal pain. I’m not bothered as I am not a fan of nuts and don’t like almond milk.
I was feeling a bit constipated last week but realized it was just a lack of fibre…..how great I now know when I’m not eating properly. This is amazing!!!
It’s been 5 weeks now and I’m ready to start the re-introduction phase. I’m not looking forward to the pain and adverse effects, but understand the importance.
I believe I know which fodmap groups are the bad ones, but I also expect to be surprised.
Thank you for all your emails and wealth of information…I’m a new woman!!!
I’m a personal trainer and my clients doctor recommended she try a fodmap diet.This was an incredibly helpful and well organized page to really break down the entire diet for those of us who may know what it is but aren’t that familiar.I’m really excited for her to hopefully get great results. Thank you for such an awesome page.The recipes are great as well.
For the items that are low fodmap at a given portion size, in that meal would I need to avoid adding in another food that is portion-specific low formap? Or could I for example have aubergine and courgette each at their specified portion sizes in the same meal? Or that meal and then strawberries for desert? I’m about to start the diet but want to be sure I’m doing it right.
Please do join the dietvsdisease support group on FB as all the members are very responsive and are mostly on FODMAP program or starting.
i have had such an issue with lectin proteins, they have caused a leaky gut. so much has been repaired but i still struggle with gaining weight and will have loose stools for a few days and then be fine. i am hopeful this will help me. there are still so many foods on this list that will be unable to eat, no matter what, but if it can help me absorb and gain weight i am willing to give it a shot. i have already been on mostly meat and veggies, with very little fruit. i love blueberries and can get so carried away with them for a treat. i can see where some of these foods could be the next issue to remove. wish i had a question to ask, but right now i am worn out with what i have been doing, for the past 6 years that i will try to muttle through. the naturopath i see says he is familiar with this diet and will give me as much assistance as i need. thank you for posting this site. kandi
i do have a question. when juicing, how do you determine the serving? kandi
Hi Kandi, why don’t you join the dietvsdisease support group on FB and ask your question there. Many people are having same issue and all the members are very responsive is almost immediate and encouraging.
Eugene’s Low Fodmap Diet
1. Cream of Rice
Can be eaten anytime everyday. If you sign up for Vons Club card then log in at Vons, then buy some boxes of cream of wheat, then online personalized special coupons should become available for this product. Normal price $3.99, but I get personalized special for $2.53 often.
2. Rice, Baked Chicken, Eckrich Virginia Ham, baked Fish with boiled Cabbage or Broccoli plate.
Eckrich Virginia Ham from Vons, Safeway, or Albertson. I ask for setting 3 which is a thick cut so it is easier for me to cut the rind off. I use only McCormick Sea Salt Grinder and Crystal Geyser water. I eat this plate up to four times a day. I have not tried this with brown rice.
3. In and out Burger
Double Meat lettuce tomato only protein style. This is two meat patties with tomato wrapped with lettuce. Extra tomato is free. In and out fries are the only fries I eat.
4. Black Angus
Black Angus will make a steak cooked with only salt if asked. Side salad no dressing, croutons, cheese, with extra tomato. Baked potato with only green onions.
5. Wood Ranch BBQ
BBQ Half chicken with no BBQ sauce and I don’t eat the skin to avoid any spices. Boiled broccoli and baked potato with only green onions
6. Marshmallow Peeps and Orange Tic Tacs
Both use sugar and no High Fructose Corn Syrup
7. Bigalow Green Tea
Best price is Walmart because they sell the larger boxes of 40 tea bags. I use Grystal Geyser water as much as possible. Currently about two gallons a day. Best price for the water is Walmart for 94 cents but Vons gives me personalized specials for 79 cents sometimes.
8. Sometimes I’ll eat Banana, Strawberry, or Kiwi but rarely lately
Re the Low-High FODMAP terminology: Websites I’ve previously read about low FODMAP diets indicate the Elimination Phase is where you eat “No High FODMAPS” during this short period to see if symptoms improve (though some might eat no FODMAPS). You then go into the “Re-Introduction Phase” as you re-introduce high FODMAPS back into your diet to see which ones you might be able to eat and in what serving sizes while still enjoying the low FODMAP foods you can tolerate. After that, you’ll be eating a “Low FODMAP” diet that’s customized for you which allows you to eat foods you can tolerate when in in appropriate serving sizes.
Spelt is gluten. It should not be on the gluten free list.
Eugene’s Low Fodmap Diet
1. Cream of Rice
2. White Rice, baked chicken, , Eckrich Virginia Ham from Vons deli cut on thick setting three with rind removed, and baked Fish with boiled Cabbage or Broccoli.. All spiced with McCormick Sea Salt Grinder. Rice cooked with Crystal Geyser water.
3. In and out Burger
Double Meat lettuce tomato only protein style. This is two meat patties with tomato wrapped with lettuce. Order of fries and Crystal Geyser water.
4. Black Angus
Steak cooked with only salt. Side salad no dressing, croutons, cheese, with extra tomato. Baked potato with only green onions.
5. Wood Ranch BBQ
BBQ Half chicken with no BBQ sauce and remove the skin to avoid spices. Boiled broccoli and baked potato with green onions
6. Marshmallow Peeps and Orange Tic Tacs
Both use sugar and no High Fructose Corn Syrup
7. Bigalow Green Tea
Made with Crystal Geyser water.
8. Rarely Banana, Strawberry, or Kiwi.
thank you.Is the rice plain ?
Hi
I did the elimination diet followed by reintroduction phase 1 year ago and would like to see if I can reintroduce further food groups. Can I just add them in the usual 6 day periods to my current diet or do I need to go back to the full low FODMAP diet first?
If you are living with mild symptoms now (little to no symptoms) then you can just rechallenge/reintroduce on top of your normal diet
Hi with the serving sizes you suggest is that per day?
Per meal 🙂
Hi. My doctor just put me on this FODMAP diet. My protein powder is gluten and lactose free, but there are so many ingredients in the protein powder and some other things that I was taking like guar gum, xanthin gum, husk, psyllium seed, hemp, chia seed, saviseed and stevia leaf extract. Was wondering how to know if these things are restricted in the FODMAP diet or how to find information on if these types of ingredients are allowed. Was also wondering what kind of fiber supplements work with the diet because by doctor suggested I take one.
Hi Carol, I’d recommend ‘Whey Protein Isolate’ powder. Most of the brands do not contain all those other ingredients, but check the ingredients before you buy, just to make sure. Not sure what country you’re in, but there should be a number of reputable brands around.
If you use the search bar on the website, you can find an article that lists high FODMAP ingredients.
Fiber supplements are high FODMAP but can work, depends what your symptoms are. Usually we don’t recommend you start a new FODMAP supplement until after the low FODMAP diet. If your doctor advises you do take one, rather than just suggesting it, then probably psyllium husk is the way to go, but again, it depends on your symptoms.
Spelt is a form of wheat and contains gluten. So to “ask for gluten-free bread, preferably spelt,” would be very bad advice for someone who needs to be gluten-free.
Hi Sherrie, gluten free spelt is still gluten free 🙂
But Spelt contains gluten…… so gluten-free spelt doesn’t exist.
Re: Lactose free milk
I’m just curious as to why lactose-free products are promoted. As far as I know, products labelled as “lactose free” usually just contain additionally added lactase enzyme.
Why the difference?
Thanks!
Hi Rita, good question! It’s a bit confusing, the answer is yes to both. Yes it’s lactose free, and yes they add lactase. When the enzyme is added, it essentially ‘removes’ the lactose, hence “lactose-free”. I guess it’s a bit like the lactase deletes the lactose 🙂
What are your thoughts on eggs?
Eggs are low FODMAP (no FODMAP actually) so they are good to have
Hi Joe,
As a former nurse, with a son about to take his med finals, I think your web site is excellent; well presented, informative and inspirational. Well done.
The following information may be helpful to others.
I’ve probably had un-diagnosed IBS for years; last year, I discovered FODMAP, which really helped.
Over the last six months I’ve had a permanently distended abdomen and breathlessness, so kept returning to see my GP, who kept saying I had IBS and printing off the FODMAP diet.
Unhappy with the lack of progress, I accessed our company’s private healthcare plan and requested a referral to a gastroenterologist, who ordered a CT scan, that came back clear.
I was then referred for a relatively new test for SIBO/ SBBO Small Intestine/ Bowel Bacteria Overload, a non-invasive (other than the Lactulose) test that measures Methane and Hydrogen gases.
The private hospital didn’t have the machine, so I was seen privately in the NHS hospital (!); the results are instant and mine came back positive, so I’ll start a course of specific anitbiotics.
The cost of the test is approx £200 which, in medical terms, is nothing.
The nurse said that since they’ve had the equipment, about six months, there has been a big rise in referrals and approximately two thirds of referrals come back positive.
At last, rather than just being told, “It’s IBS”, it may now be possible to be more specific and provide a swift solution but how sad I had to persevere and access treatment via private healthcare, rather than NHS.
This treatment is available on the NHS but it’s likely patients will need to request it and possibly make their GPs aware.
Hope this helps others.
Thanks for the insights Tim. Breath testing is emerging as a useful tool. it’s not 100% accurate yet so it’s not been adopted everywhere but I can see it becoming especially useful in the future
Hi Tim,
Thanks very much for the info. I went to a doctor too a million times after having a permanently distended stomach, just told me is IBS and there is nothing he can do to help other than prescribing some probiotics. Is your present treatment helping with the distended stomach? I forced to hold in my stomach all day long to avoid an embarrassment, I Lift weights and have an athletic body but my stomach is 5 times out of proportion.
I am on this diet and find it very helpful. However, I am trying to go vegetarian and don’t understand what meat replacement products are okay. I also need some advice on the way this diet can be compatible with a vegetarian diet.
Hi Penney,
To replace meat in meals I presume you want to replace the protein aspects of meals.
In this case you can use egg, hard cheeses, and a variety of nuts (see this article: https://www.dietvsdisease.org/low-fodmaps-food-list/)
Tempeh is also a good option, as is hard tofu and canned lentils. Note the portion sizes though.
I am on this diet and find it very helpful. However, I am trying to go vegetarian and don’t understand what meat replacement products are okay. I also need some advice on the way this diet can be compatible with a vegetarian diet.
Hi Penney, I recommend a book called “Low FODMAP vegan” by Joe Stepaniak.
I am new to being diagnosed with IBS-D, and as I was going through the list of low FODMAP items I came across a number of items that I already know are triggers. Mainly anything with a skin or seeds, including nuts. The reason I noticed the connection between these and my IBS symptoms was I would eat a lot more of these as I started to work out more, then I would slowly feel worse until I was in a full blown attack. I also noticed a number of items that I thought had a lot of insoluble fiber where I am told to eat more soluble fiber. Any suggestions would be greatly appreciated.
I looked over the large fodmap list you provide and didn’t see eggs. Is it on there and I just missed it? I’m a beginner on this diet and am having problems underdtsnding where to start in a slow pace.
Hi Susan, eggs are on the list, I think you may have overlooked it 🙂
Hello Joe,
THIS IS A SUPERLATIVE AND GENEROUS RESOURCE, THANK YOU AND YOURS!
I ‘misplaced’ the little section where people offered supplemental methods like imaging, meditation, etc. Would you please redirect me.
Thanks again, I am encouraged at 68,
Jan
Thank you for this valuable resource, it is one of the most comprehensive on the internet! Are there any App’s that you recommend to help with the FODMAP’s diet?
You’re welcome Chris. I’d recommend the Monash University app for low-FODMAP dieting. This is the university where FODMAPs were discovered as a problem for people with IBS, and the subsequent way of eating was invented.
The shopping list is missing critical information about protion sizes. For example 1 slice of white wheat bread is low FODMAP with 2 slices are high.
The most definitive source of information on the FODMAP content of foods is the Monash University GI department phone app. They are the group that developed the diet. The app cost about 10 USD/7 GBP. Updates are free and all of the money goes to support IBS research and improvement of the FODMAP diet
http://www.med.monash.edu.au/cecs/gastro/fodmap/iphone-app.html
There is no evidence to support the notion that “It’s thought that high temperature cooking can breakdown FODMAPs (potentially favorable), but to what extent is not yet known. “
When one says “It’s thought that” it’s a heads up that there is no scientific evidence to support the idea. I don’t believe the author here intended for anyone to think the idea was evidence based.
Its good to have tips that you can apply on your balanced diet. You can also add on your dietary meal the probiotics, it helps in digestion of foods and has a lot of health benefits. Thank you
What about ground flax seed?
I’m also on low FODMAP diet and all these makes it all easier to understand. Thanks Joe! please keep posting blog about fodmap
Hello Joe,
Is it possible please to sent me a list of high Fodmap food list because I do not have one.
thanks and regards
Hello Joe,
Is it possible please to sent me a list of high Fodmap food list because I do not have one.
thanks and regards