Stomach bloating after meals can be incredibly uncomfortable.
Research shows that 10 to 25% of healthy people experience it to some degree, yet most don’t do anything about it (1).
It’s even more common among those with gastrointestinal disorders, such as IBS.
Fortunately, diet changes alone can help to relieve or prevent most cases. This article explores what is scientifically shown to help stop bloating.
What Causes Stomach Bloating?

Stomach bloating is characterised by a strong feeling of pressure within the abdomen.
The term is often used interchangeably with dyspepsia (indigestion), stomach distention or water retention. These are separate issues, but they may occur at the same time as bloating.
It’s common in gastrointestinal disorders, especially irritable bowel syndrome (IBS).
However, it also occurs in the absence of other medical conditions (2).
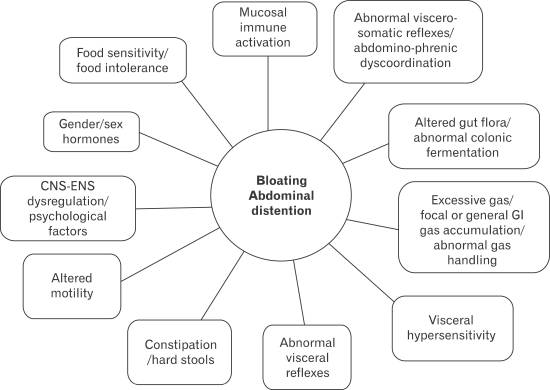
A comprehensive list of the proposed causes of bloating. Click to enlarge.
The exact causes of bloating vary from person to person, and sometimes between episodes. But it’s typically the result of (2, 3):
- Abnormal gut bacteria
- Unusually slow digestion
- Abnormal abdominal muscle reflexes
- Increased nerve perception of pain
- Food sensitivities (either FODMAPs or food chemicals like histamine)
- Psychological distress
Summary: Bloating is defined as strong abdomen pressure after meals. The causes vary by person and by episode.
1. Treat IBS and FODMAPs Sensitivities

Irritable bowel syndrome is a common disorder that causes a variety of digestive symptoms.
Bloating is one of the most common symptoms of IBS, with more than 90% of IBS patients complaining of it (4, 5, 6).
For many, eliminating trigger foods in the diet relieves the problem, which are almost always FODMAPs (5).
In one study on IBS patients, 43 participants were prescribed a low FODMAP diet, while 39 volunteers continued a standard diet to act as the control. Both groups completed questionnaires about changes to their symptoms.
82% of patients in the low FODMAP group reported improvements in bloating, while just under half of the control group reported improvements (7). So there is a notable improvement.
Summary: Studies show that FODMAPs are a common trigger of bloating in those who are sensitive. Following a low FODMAP diet should be the first step if you have or suspect IBS.
2. Probiotics Can Help Get Rid of Bloating
Probiotics are beneficial bacteria found naturally in certain foods and supplements.
There is loads of evidence they can help with digestive health, especially bloating.
In a study of 122 IBS patients, a daily dose of Bifidobacterium bifidum significantly improved bloating and pain symptoms compared to placebo (8).
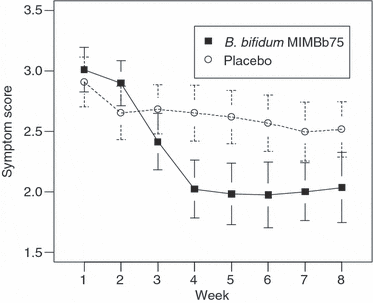
Comparison of B. bifidum and placebo on IBS symptoms measured by subjective global assessment (SGA) over 8 weeks. Lower score is better.
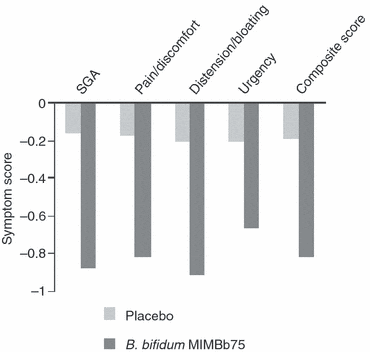
Comparison of change in IBS symptoms with B. bifidum vs. placebo before and after treatment. Lower score is better.
These results are supported by another trial that used a combination of strains for a 4-week period, one of which was also from the Bifidobacterium species (6).
Interestingly, it’s not uncommon for the placebo groups in these studies to experience digestive improvements. So there is certainly a placebo effect at play to some degree (9).
Note that only certain strains of probiotics at specific doses have so far shown to be useful for bloating, when taken for at least 4 weeks:
- Lactobacillus acidophius and Bifidobacterium infantis at a dose of 1 x 1010 cfu per day (10).
- Lactobacillus acidophilus plus Bifidobacterium lactis at a dose of 2 x 1011 cfu per day (11).
- Bifidobacterium bifidum at a dose of 1 x 109 cfu per day (8).
- Bifidobacterium lactis at a level of 1.25 x 1010 cfu per dose, plus a combination of Streptococcus thermophiles and Lactobacillus bulgaricus at 1.2 x 109 cfu per dose (6).
But there are also studies that have shown little benefit of probiotic supplements on bloating too, so there is still more to learn (2, 9).
If you decide to try a probiotic, ask a pharmacist to help you select one that does not contain FODMAP ingredients. Otherwise they should be safe, with the possible exception of those with a weakened immune systems (12).
Summary: Certain strains of probiotics are likely to help improve bloating. A pharmacist can help you to choose one that is low FODMAP and contains the appropriate strains.
3. Digestive Enzymes May Reduce Bloating
Digestive enzymes are chemicals within the body that help break down foods into smaller components.
Some people lack sufficient enzymes to break down certain carbohydrates during digestion (namely FODMAPs).
Undigested carbohydrates that reach the gut undergo fermentation, causing gas and bloating (4).
This is where digestive enzyme supplementation with meals may help:
- Alpha-D-Galactosidase supplements (such as Beano) help break down oligosaccharides. Small studies suggest that 300 to 1200 GalU of alpha-galactosidase with meals helps with some causes of bloating and gas production (4, 13, 14).
- Lactase is a digestive enzyme that aids in the digestion of lactose. Those with lactose intolerance may find it beneficial to have before consuming dairy (15). There are also dairy products that contain lactase for those who are lactose intolerant.
- Certain health conditions – including cancer, cystic fibrosis, and diseases of the liver and pancreas – cause impaired nutrient absorption, and sometimes bloating. In some cases a particular digestive enzyme may be useful, but these are almost always prescribed by a doctor (15).
With the exception of specialized enzymes for disease, digestive enzymes can be purchased over-the-counter without a prescription. You should always speak with your doctor before introducing new supplements.
Summary: Over-the-counter and prescription digestive enzymes may help those with FODMAP sensitivities to digest certain carbohydrates, which may reduce bloating.
4. Minimise or Treat Constipation

Constipation is a major trigger of bloating.
Hard stools in the digestive tract are believed to increase the diameter of the rectum, which slows down movement of food and gas through the digestive tract (2).
Constipation may also increase fermentation of carbohydrates in the gut, which can produce gas and further increase bloating. In fact, bloating is the number one symptom of constipation-dominant IBS, or IBS-C (2).
Regular bowel movements is the solution of course.
Drinking adequate fluids, exercising more, and eating low FODMAP fiber sources are some of the strategies that help you to stay regular.
Summary: Constipation is believed to contribute to bloating, either by slowing clearance of gas from the digestive tract or by increasing fermentation of carbohydrates. For many, treating constipation will fix bloating issues too.
5. Limit Products Known to Cause Digestive Stress

Several foods (other than FODMAPs) can contribute to bloating, at least in theory.
Coffee is one of those, especially if you are caffeine intolerant. In fact, cutting down on caffeine can have many health benefits.
Slowed clearance of gas from the intestinal tract is also a known cause. For this reason, it may help to avoid foods that increase gas volume:
- Carbonated beverages may introduce more gas into the digestive tract.
- Chewing gum and hard candy may also cause you to swallow excess air, thereby increasing gas production.
Many chewing gums and hard candies also contain sugar alcohols, which are largely indigestible. This is why excess chewing gum has a laxative effect and warning on the label.
Nutrition supplements can also cause digestive stress, particularly low quality protein powders and meal replacement powders.
Summary: Certain products are thought to increase the amount of gas in the digestive tract, which may cause discomfort if gas clearance is slow. Removing these items from the diet might be beneficial.
6. Modify Mealtime Behaviours
Small changes to eating habits may help to reduce bloating.
Studies suggest some are more sensitive to the sensation of the stomach stretching after meals (4).
In theory then, eating smaller meals may prevent the bloating sensation by decreasing stomach stretching.
Additionally, try not to eat quickly and avoid using straws (which can allow gas into the stomach).
Summary: Eating smaller meals, slower, may help with bloating.
7. Low-Intensity Exercise Can Help Reduce Bloating

Low-intensity exercise is believed to help move gas through the digestive tract, thereby reducing bloating.
In one small study, 8 volunteers (7 with IBS) received infusions of gas into the digestive tract (16).
They then alternated between rest and low-intensity exercise on a stationary bicycle while researchers took measurements.
Subjects at rest retained 45% of infused gas compared to only 24% during exercise, which is almost half the amount.
Summary: Mild exercise may help you to move gas through the digestive tract and relieve bloating.
Natural Remedies for Bloating
Small studies indicate some natural remedies may help stop bloating.
8. Peppermint Oil

Peppermint oil capsules are derived from peppermint plants.
They are believed to help increase intestinal transit time by relaxing stomach muscles and increasing the flow of bile.
In a recent study, 35 volunteers with IBS received capsules containing peppermint oil and fiber, three times per day. A second group of 37 volunteers received a placebo pill that only contained fiber.
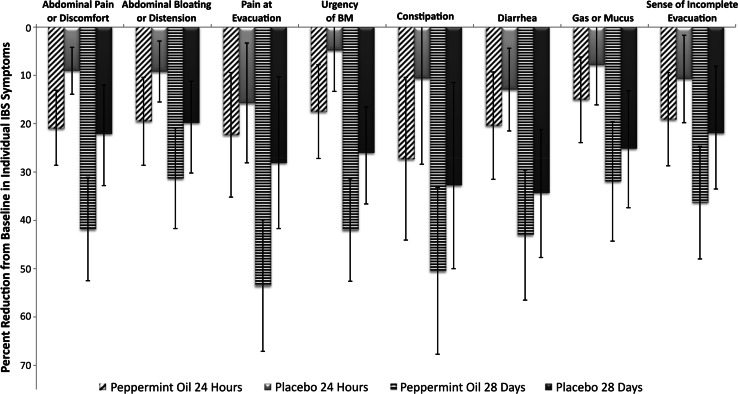
After 4 weeks, the peppermint oil group showed a 53.5% improvement in symptom scores for bloating and distention, compared to 28.1% improvement for the fiber-only group (17).
Comparison of change in IBS symptoms with peppermint oil capsules vs. placebo at 24 hours and 24 days. Higher score is better. Click to enlarge.
Note that placebo was also very powerful for reducing symptoms after one month, so it’s hard to say how useful peppermint itself is.
Additionally there was one study that found peppermint may slow intestinal transit time, which would worsen symptoms for certain people (18).
9. Meditation
Meditation is the ancient spiritual practice of connecting the mind with the body (19).
It’s known to be an effective strategy for relieving psychological stress, which is loosely linked to bloating (2, 20).
A small study of 13 IBS patients showed significant improvement in bloating with 15-minute meditation sessions, twice daily.
Study participants reported that the benefits continued at 3-month and 1-year follow-up visits (21, 22).
There are many free meditation apps available.
Summary: Small studies suggest that peppermint oil and meditation may relieve bloating in some cases. These strategies are generally well-tolerated, but more research is needed regarding their effectiveness.
What to do next?
Ultimately if you follow these instructions then managing bloating can be a “simple” process…
But that does not mean it’s an easy process because you need to be consistent with the changes you make. That’s often the hard part and reason people struggle more and more with bloating as they grow older.
If you want to learn more about how we might be able to help you, I invite you to apply for a nutrition assessment call with us.
Severe bloating and related digestive disorders is what we specialize in, and we are the world’s leading team to do this online.
What Can And Can’t I Eat On The Low FODMAP Diet?
Often it’s easiest to start with this giant list I’ve made of what foods to eat, and what foods to avoid when following a low FODMAP diet.
It’s based on the latest published FODMAPs data (1, 2, 3, 4, 5).
Print or save to your phone to use as a quick-reference guide when shopping or cooking. I’ve attempted to list foods in both US and UK/Aus names, with US first.
I’ve included a screenshot of the first page below. But the full PDF is 4 pages and suitable for printing. To download it simply tap the box below and it will then be emailed straight to you – it’s free!





Yes! Finally something about products available.
Hi hope you can help! Been on the fodmap diet for more than 6 weeks & still suffering from serious bloating, my intestine can be seen poking out through my stomach & it hurts! I am very slim only 40 kilos & have lost some weight too! What else can I do? I take probiotics, have just finished digestive enzymes, have been taking aloe vera, reduced caffeine, no grains except oats & a tiny amount of rice 1-2 a week, gluten free for more than 2 yrs,can’t eat cheese, which is supposed to be ok on low fodmaps… still constipated & having diarrhoea daily! still suffering & very confused about what to do now! Thanks! Sam
Thank you for your blog post. Jones and I happen to be saving to
buy a new book on this subject matter and your article has made all of us to save our own money.
Your opinions really responded to all our queries. In fact, greater than what we had known prior to when we discovered your
wonderful blog. My spouse and i no longer nurture doubts and a troubled mind because
you have attended to the needs in this post.
Thanks
It seems like everthing you eat can upset you. The bloating and pain never completely go away. Even headaches and upper digestive area are included. Peppermint ?????
Hi Jane, yeah there is a bit of evidence for peppermint I believe, such as peppermint tea. Give it a try 🙂
Do you know if peppermint oil inhibits iron absorption from plants? I’ve googled a bit and it seems that peppermint tea can, but I’m not sure if the substances responsible for that are in the oil as well.
If it does inhibit iron absorption, can it be effective when taken between meals, or is the bloating preventing effect only there if taken with meals?
I felt bloated immediately after eating certain foods earlier. On diagnosis and noting down the symptoms, my doctor suspect that I`m suffering from Gluten Intolerance. And, this condition is contributing to my abdominal bloating.
After searching and stumbling upon various forums, i find no way to treat my condition other than following a gluten free diet. Following a gluten free lifestyle helped me and now my condition has improved.
“During the mean time, I also figured out this amazing way of quick way to help my bloated stomach. Chewing Ginger on a bloated stomach cured my pain always”
Have hardcopy on fridge. Need electronic copy for mobility