A healthy and diverse gut bacteria is important for health.
However, an overgrowth of this bacteria in the small intestine – known as SIBO – can cause serious problems.
This article takes a detailed look at SIBO and what dietary changes are scientifically shown to help.
What is SIBO?
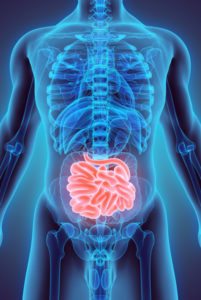
Small Intestinal Bacterial Overgrowth (SIBO) is a digestive disorder characterized by excessive bacteria in the small intestine (1).
These bacteria then ferment (interact with food particles and nutrients) to cause a wide range of symptoms.
Unlike the large intestine (also known as the gut or colon), which contains most of your gut bacteria, the small intestine should not have a large amount of bacteria.
SIBO is uncommon in young and middle-aged adults, but is thought to occur in at least 14% of older patients on average (2).
Large intestine (colon) is shown in red. Small intestine is shown in pink. Click to enlarge.
Summary: Excessive bacterial growth in the small intestine is known as SIBO. It becomes much more common as we grow older.
Common Risk Factors for SIBO

Researchers suspect SIBO is caused by a combination of decreased pancreatic enzymes, bile acids and gut motility.
Consequently, certain health conditions or lifestyle choices may increase your risk of developing SIBO:
- Gastrointestinal infections: Such as post-infectious IBS (Irritable Bowel Syndrome)
- Chronic use of antacids: Long-term antacid use reduces acid production in the stomach. Consistently low levels of stomach acid can lead to bacterial overgrowth in the stomach and small intestine (3, 4).
- Immunodeficiency Syndrome: Disorders that can suppress our immune system – such as AIDS and IgA antibody deficiency – provide an ideal environment for harmful bacteria to thrive (5).
- Celiac disease: Celiac disease can disturb how food moves through the intestines, particularly if it remains undiagnosed or is poorly managed. This leads to increased bacterial growth in the gut (6, 7).
- Aging: In general, older people are at increased risk for SIBO because our digestive tract gets weaker with age. This is thought to be caused by reduced physical activity, weight gain, ongoing medication use and general weakening of the gastrointestinal tract (8, 9).
- Alcoholism: Chronic alcohol consumption appears to increase risk of SIBO (10).
- Gastroparesis: There is a strong overlap between symptoms, and it seems those with gastroparesis (also known as delayed gastric emptying) are more likely to have SIBO (32).
Numerous other conditions are linked with increased SIBO risk, but more research is needed. These include hypothyroidism, Crohn’s disease, ulcerative colitis, fibromyalgia, rheumatoid arthritis, Parkinson’s disease and more.
Summary: Your risk of SIBO is greatly increased by several conditions and factors, most often related to reduced function and efficiency of the intestines.
Would you like more information on how to eat for SIBO?
Tap the blue button below to download our “Eat This, Not That” list as well as additional resources for SIBO and digestive issues (it’s free!)
SIBO Symptoms

Many SIBO patients experience different signs and symptoms.
These often overlap with other conditions such as IBS. The most common problems are (1):
- Fatigue
- Nausea and vomiting
- Bloating and diarrhea
- Poor nutrient absorption leading to deficiencies
- Malnutrition and weight loss.
Some people may also experience depression and skin problems like acne and eczema.
The intensity of symptoms can differ, too.
While some patients may have diarrhea and milder vitamin deficiencies, others may experience severe nutrient malabsorption and impaired digestion (2).
Nutrient Deficiencies
Left unmanaged for several months, SIBO can cause several vitamin and mineral deficiencies.
Vitamin B12 deficiency is one of the most common deficiencies, alongside the fat-soluble vitamins such as A, D, E and K (2).
Mineral deficiencies such as iron, calcium and magnesium are also common in SIBO patients.
Summary: SIBO symptoms range from digestive stress to severe nutrient deficiencies. They are often similar to IBS.
Diagnosing SIBO: Hydrogen Breath Test

SIBO is a severely under-diagnosed condition (2).
This is because a large portion of our small intestines is impossible to reach without surgery.
Fortunately, some non-invasive tests have been designed; namely the Hydrogen Breath test. This same test can be used to detect common food intolerances, IBS and H. pylori infection.
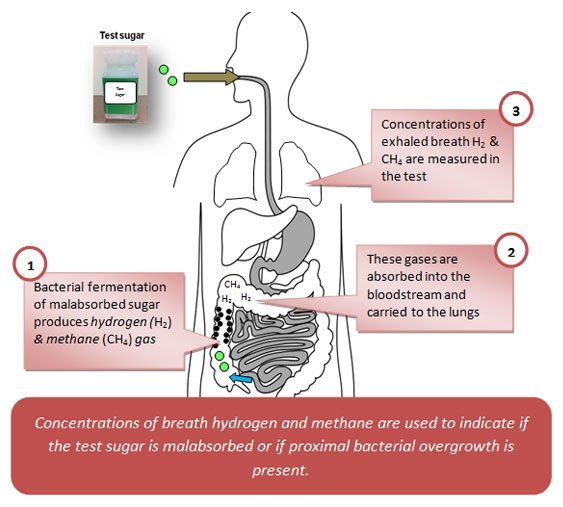
Breath Test for SIBO
The two types of Hydrogen Breath Test used for SIBO are the LBT and the GBT.
Both tests measure concentrations of hydrogen and methane in the breath.
While neither is perfect, the LBT seems to be preferred.
How a SIBO breath test works. Click to enlarge. Image source: Sanjosefuncmed.com
These two gases are only produced by bacteria (in the small intestine) and not directly by humans. High levels indicate increased bacterial activity and/or overgrowth.
In order to give an accurate reading, prior to the test patients follow a specialized diet for 1-2 days that does not feed the bacteria. On the day of the test, a formulated sugar drink is given in order to get a clear reading of the patient’s reaction to carbohydrates.
The test can be done with take-home kits or with your doctor in the clinic. But interpretation of results should always be with a health care professional.
Summary: The best non-invasive method for diagnosing SIBO is with a Hydrogen Breath Test. Request with your doctor if they have been unable to pinpoint your digestive symptoms.
First Line of Treatment: SIBO and Antibiotics
Diet alone will not rid of SIBO, so you’ll need antibiotics or herbs (or both) as your first line of treatment.
Conventional treatment for unwanted bacterial growth is antibiotics (2).
Antibiotics are designed to kill bacteria, which is why they are prescribed when you have an infection.
RN (I cannot put the full name of the antibiotics here as the search engines may penalize us for mentioning medication) is the most well-studied antibiotic for SIBO, with a success rate of about 50% after 1 week (14, 15).
Here is the recommended therapy, according to information from a SIBO symposium in 2014:
- Patients with a positive hydrogen breath test: 550 mg RN 3 times per day for 14 days (not missing any doses).
- Patients with a positive methane breath test: 550 mg RN 3 times per day + 500 mg NN twice a day for 14 days. Alternatively, 550 mg RN 3 times per day with 250 mg ME 3 times per day for 14 days.
- Antibiotics treatment should be followed by a pro kinetic (which enhances intestinal tract motility) for 3 months, a repeat breath test and then a low FODMAP diet (more on that below).
Herbal Antibiotics
Herbal antibiotics are also an option, with over 50% of patients who fail on RN reporting success with herbal treatment. In this particular study it was Dysbiocide and FC Cidal or Candibactin-AR and Candibactin-BR (16).
Some people may need to do multiple rounds of either herbal or pharmaceutical antibiotics to completely stop bacterial growth.
Just remember that herbal antibiotics must still be taken under the supervision of your doctor. They can interact with other drugs.
But Don’t Rely Too Much on Antibiotics
The problem with antibiotics, pharmaceutical or herbal, is they do not differentiate between good and bad bacteria — they destroy all bacteria.
Long-term use leads to serious imbalances in your gut bacteria, linked to numerous other health conditions such as insulin resistance and obesity (17, 18).
SIBO antibiotics are also only a temporary “band-aid” treatment, and do not address the root cause of the problem. This is why those only treated with antibiotics are likely to relapse and experience SIBO again (19).
In fact, a study on antibiotic therapy alone versus antibiotics plus guar gum supplementation (a fermentable carb) found that success rates were improved from 62% to 87% with the guar gum added (31).
This seems counter-intuitive because it showed the addition of guar gum (which feeds gut bacteria) was more beneficial than harmful. It’s also in line with studies showing that prebiotics and probiotics – additional bacteria – are beneficial (more on that below).
So, antibiotics are especially useful in the short-term (and often necessary), but are not a permanent solution, and certainly not a solution themselves.
Summary: Antibiotics are useful (and often necessary) in the short-term to treat SIBO. However, patients who solely rely on them are likely to relapse. They also kill both bad and good bacteria, which is very harmful to long-term health.
Low FODMAP Diet and SIBO

FODMAPs are a type of fermentable carb common in the foods we eat.
They act as necessary “food” for our gut bacteria, but can cause severe digestive problems in sensitive people.
The process of identifying and removing problem FODMAPs from the diet is known as a low FODMAP diet, and is clinically proven to treat IBS (26).
SIBO shares almost all the same symptoms as IBS. In fact, studies show that between 30-85% of patients with IBS also have SIBO (27, 28, 29, 30).
Due to this strong overlap, researchers suspect a low FODMAP diet may be beneficial for SIBO patients too, as it would “starve” the problem bacteria in the small intestine.
Unfortunately, there has not been much research in this area and the current evidence is not clear.
It seems the low FODMAP diet is incredibly helpful when starting off, but requires a bit more flexibility for SIBO when reintroducing fermentable carbs.
Just make sure not to start a low FODMAP diet until you have finished your course of antibiotics. The “bad” bacteria need to be active for the antibiotics to work.
There’s also limited research on the long-term effects of a low FODMAP diet. Following such a strict regimen for a long period of time may lead to detrimental effects on the bacteria in the large intestine.
Summary: A low FODMAP diet may help initially by “starving” the problem bacteria in the small intestine. But studies have not yet confirmed it as a reliable SIBO treatment.
SIBO and Probiotics
Probiotics is the name given to bacteria we intentionally eat for health benefits.
They are essentially the opposite of antibiotics (20).
It seems counterintuitive to treat SIBO – bacterial overgrowth – with additional bacteria, but recent research has seen success using probiotics instead of antibiotics.
One small study of 14 IBS patients with SIBO found that a daily probiotic drink altered fermentation patterns in the intestine, consistent with reducing SIBO (21).
Another early study found that 82% of patients receiving probiotics for 5 days reported improvements compared to only a 52% improvement in those receiving the antibiotic metronidazol. These findings are in line with previous animal studies that observed similar benefits of probiotics (22, 23).
To be fair, though, some research found no significant benefits. One clinical trial on children treated with omeprazole found that probiotics didn’t help, at least not in preventing SIBO (24, 25).
Until we know more, probiotics are not recommended until after completing the antibiotic protocol and a low FODMAP diet.
You also want to be careful of the type of probiotics you are using. Avoid any product with added ingredients like maltodextrin, which can end up feeding the bad bacteria.
Summary: Early studies have found probiotic supplementation may help with SIBO treatment. Its effectiveness has not been proven in clinical trials, though, but it’s a promising area. Consider using them only after you have completed antibiotic treatment and a low FODMAP diet.
SCD and GAPS Diet Plan for SIBO

There is a lot about gastrointestinal diseases and conditions that science does not yet understand.
SIBO is no exception, which is why the perfect diet plan just doesn’t exist yet. Several potential diets have emerged that are worthy of consideration, but we should be cautious and only trial them under medical supervision.
The following two diets are well-supported by anecdotal evidence (testimonials):
SCD
The Specific Carbohydrate Diet (SCD) claims to help treat several forms of bowel disease.
This includes ulcerative colitis, Crohn’s disease, diverticulitis and celiac disease.
Foods allowed:
- Meat, chicken, fish, eggs, some legumes, lactose-free dairy, ripe fruit, non-starchy vegetables, nuts and seeds, and honey.
Foods not allowed:
- All grains, starchy vegetables (such as potato, corn), regular dairy, some legumes, sugar.
Basically it shares many similarities to the low FODMAP diet, but not as much scientific backing at this stage. More studies are underway and I’m looking forward to the results.
GAPS Diet
The Gut and Psychology Syndrome diet (GAPS diet) is similar to SCD but with a few modifications.
It contains a different introductory phase, fewer legumes, and dairy protein is reintroduced more slowly.
There is some anecdotal evidence to support it, but these are for autism and other conditions related to brain function (hence the name) rather than digestive issues.
There are no studies of the GAPS diet in the medical literature, and the creator makes a lot of extraordinary claims, which is often a red flag.
Summary: The SCD and GAPS diet have emerged as potential diets to help treat SIBO, but neither was actually designed for this condition. They may be useful, but are not evidence-based.
Unproven Treatments
SIBO sufferers have looked to other alternative treatments to help reduce their symptoms and rid of bacterial overgrowth.
Keep in mind that these are all anecdotal, and there has been little to no research on these potential treatments. Be sure to check with your doctor before trying any option mentioned below.
Iodine
Some have claimed that taking iodine — namely Lugol’s 5% iodine — has helped them rid of SIBO.
However, the role of iodine as an effective antibiotic for the gut has yet to be studied.
It’s important to remember that iodine directly affects your thyroid. Discuss with your doctor before starting any protocol, especially if you experience thyroid issues.
Peppermint and Other Essential Oils
Enteric-coated peppermint oil has proven to be effective in reducing symptoms like bloating in patients with IBS (26).
In this study, the researchers found that peppermint oil decreases the production of hydrogen, a bacterial byproduct in patients with SIBO.
Other essential oils — including oregano, tarragon, frankincense, wormwood, and clove oil — may also lend some relief.
Do know that these oils can be potent. Before starting any essential oil regimen, check with a skilled practitioner to help you determine exact dosing.
Intermittent Fasting
Some people believe that intermittent fasting can help “starve” the bad bacteria.
But this may not rid of the bacteria completely. Instead, starving them may make them harder to eradicate.
Summary: There’s been some anecdotal claims that natural products including iodine and enteric-coated peppermint oil can help reduce symptoms and maybe even rid of SIBO completely. However, there’s been little or no research on these potential treatments.
Overall Recommendation for Diet and SIBO
It reportedly takes about 2 to 5 years on average for SIBO to be completely corrected.
For this reason it’s important to explore the different treatment options and find what works for you. Unfortunately, there is no single diet guaranteed to treat SIBO 100% effectively.
From the weight of evidence, two weeks of antibiotics is warranted first in order to deal with acute symptoms and bacterial overgrowth. A prokinetic may be required afterwards.
This should be followed by a low FODMAP diet to identify any food intolerance. The SCD diet is also something worth exploring, as is probiotic supplementation after a low FODMAP diet.
This all needs to be done under the supervision of your doctor and dietitian.
Would you like more information on how to eat for SIBO?
Tap the blue button below to download our “Eat This, Not That” list as well as additional resources for SIBO and digestive issues (it’s free!)



Starting in 2001 I began to notice I didn’t feel just right, but it came on so gradually and I couldn’t pinpoint the origin.
There was some nausea, but it would come and go. At mealtime, I would prepare my plate, but half way through eating it, I would get full.
This went on for years, but why I didn’t figure it out sooner, I don’t know.
I then noticed, after my noon meal, that I couldn’t eat again that day, it took about 13 hours to digest a meal. So one meal a day is all I could handle.
After reading about SLOW DIGESTION causing SIBO, I did a stool test and saw A LOT of Pathogenic Bacteria. Now how was I going to get rid of that?
I decided to kill it off with Iodine. How else could it be done? I knew of no other way. At the time I belonged to the Iodine Group at Yahoo.
So I found a LAB that made Lugol’s Solution 5% on the west coast of Canada, went to my local Pharmacy and ordered a bottle. The staff didn’t know what it was, when it arrived and neither did the Pharmacist. They were asking me what I used it for.
At the time I was reporting to the Yahoo Group, how my treatment was going weekly. So I started on a Friday and took one drop each day. The next Friday I started on 2 drops. By the end of the 3rd week at 3 drops daily all the nausea left me after 8 long years. I was so relieved to have found the answer.
Adding a Thyroid pill really took care of the slow digestion. I complained often to the Group about the bloating and finally a gal was kind enough to point out that a weak Thyroid, would cause digestion to slow down. I never made that connection.
Of course I continued increasing the Iodine at the same rate until I reached 16 drops per day (100 mg) in 16 weeks, still reporting to the group each week. At 12 drops my Type 2 Diabetes left, at 16 drops I no longer had bladder infections or sinus infections, shrunk my thick Uterus (the doctor was going to order a Hysterectomy very soon) and Uterine and Breast Fibroids disappeared.
Finally I lowered the dose to a maintenance level.
Thank you for allowing me to tell my story.
Bonnie I just recently read your article that you wrote about SIBO, I just recently was tested myself but have not gotten the results back yet I have been suffering for the past seven years and I’ve been to five gastroenterologist and just keep saying it’s IBS it’s IBS but I’ve had a lot of pain a lot of bloating a lot of fatigue just not feeling myself and I just have been beside myself trying to find out what this is with no help from anybody else could you tell me what group you belong to on Yahoo and how to get there and possibly elaborate a little bit more on the iodine solution I have a nephew who is a pharmacist here in the United States and I’m sure I could probably get him to help me out with that portion of it but I’d like a little bit more information and I’d love to be able to get into The group so that I can share some ideas or possibly hear her and try some ideas if you could just give me the information how to find the group and get in there I’d be greatly appreciative! My email is cadriscoll60@gmail.com, if you’d be willing to leave that information then I’d appreciate it as I’m not sure I can find my way back to this very specific page
Hi Bonnie,
I too suffer from years of SIBO, being in the mountain state does not help at all due to all local and surrounding doctors knowing nothing about the condition, nor have they ever heard of it. I have been doing this on my own for 14 years with diet, antibiotics, herbal treatments etc..etc.. the list goes on but nothing has helped. I am willing to give anything a try but was wondering what Brand of Lugol’s Iodine you purchased? I have noticed a lot of so called Lugol’s Iodine fakes out there and want to make sure i am purchasing the correct one and not wasting my money.
Thanks!
Donnett
What kind of thyroid pill??
Bonnie, you mention the Lugol’s Solution 5% and then you go on to say that adding a thyroid pill really took care of slow digestion. What type of thyroid pill?
Patricia
What type of Thyroid pill? I guess there are a few kinds on the market and she did start me on a pill that you buy prepackaged from the Pharmacy called ERFA but I reacted badly to it, too many fillers.
I ended up with Natural Dessicated Thyroid USP which was compounded for me.
Bonnie
Hi ? are you adding this to water? I read this the other day. I have SIBO too and sick of it!!!
Nevermind, I got the answer below. I just had my first glass of water with iodine. I hope it works!!
Leah, what has your experience been? I just ordered mine.
what is the normal maintenance dose to keep up forever or how long after reaching the 16 drops. you did not explain that very clearly and that is why I am asking . I am not informed on iodine intake so this is a special iodine ordered so a pharmacy iodine for cuts and bruises would not be suitable.My problem is just SIBO>
hi bonnie did you take selenium, citaminc C and other supplement as part of your iodine protocol. if yes, how much ?
also does iodine is effective for methane sibo
sorry i meant “vitamin c”, typo.
Hi Bonnie,
did you change your diet at all? Or what was your diet like when you started treatment with the iodine? What exactly did you take, just the iodine and the thyroid supplement? What was the thyroid supplement and the dosage you used?Did you take any other supplements during that time in addition to that? Did you do this under the supervision of a doctor? Im 25 and I have been struggling for over a year now with SIBO methane, new found food allergies I never had before and a wealth of other health issues, not to mention there is a history of thyroid issues in my family. Needless to say, I am desperate and I am willing to try just about anything. My western medicine docs look at me like I’m a nut job when I say that I don’t feel right, I’m constantly constipated, exhausted, and emotionally drained from trying to figure this all out while being broke as all get out. if you have any other information you can give me on what you did I would be beyond appreciative. It doesn’t sound like a long journey but it certainly has felt like it.
thanks,
alex
How are things now? My 22 year old has had stomach problems for years. Children, university of Chicago,
Mayo……. only thing they found was a small amount of ‘sludge ‘ in gall bladder. She had it taken out when she turned 21. Been dealing with nausea and back pain since. In November the Gi treated her for sibo as she had the signs for it (no test). The first two rounds of antibiotic helped. The third one has made the pain and diarrhea worse
Now she is being tested for c-diff
Meds just have not been all that helpful fir this. Wondering what kind of doctors were helping you with the thyroid, iodine procedure?
Thank you for sharing
Just wondering how iodine works with other Meds
Appreciate your sharing
How do I keep in touch with you?
Jeannie
Bonnie, do you have a blog site?
I am assuming that this is the same as Small Bowel Overgrowth from which I have suffered for many years. My specialist, a consultant surgeon, advised me against probiotics and to this day I have complied with his advice. Recently I have been keeping a complete record of my daily intake in the hope it will provide a clue as to what encourages the recurring bouts of diarrhoea, hopefully this will help me avoid the problems as a cure is not really forthcoming in the near future.
You say a cure is not forthcoming? My Testimonial shows that a cure is HERE right now. And I cured my Bacterial Overgrowth and you can too.
What information did you need that I didn’t supply in my Testimonial above?
Is it too hard to understand?
I don’t understand how your problem is SIBO. I have had it for 25 years and it causes severe diarrhea and cramping. Mine has gotten worse as I have aged – to the point it was lasting 4-5 hours a day. The only thing that helps me completely is Lotronex, which is incredibly expensive if you are on Medicare. Also another help is following the FODMAP diet.
I don’t understand why iodine. No doctor has ever recommended that before. I have a normal thyroid.
m. r.
Marcia
Marcia
You might be surprised if you ever decide to try Iodine.
There is a book for sale on Amazon called Breast Cancer and Iodine by Dr David Derry.
Apart from using Iodine to kill off bacteria, it is a necessary nutrient needed DAILY for the health of the Thyroid, Breasts, Ovaries and Prostate. These organs NEED Iodine (in tiny amounts) and without Lugol’s Iodine where will you get Iodine? We can no longer depend on eating Seafood to supply our Iodine, since the Nuclear Radiation Leak in FUKISHIMA, Japan a few years ago. This Reactor is still leaking Radiation, by the way, which reached the shores of California about 8 months later. So it is in the rain and in the air we breathe and will take a million years to clear AFTER IT STOPS LEAKING. You can protect yourself from this Radiation binding to your receptors, by taking a tiny daily dose of Lugol’s Iodine.
Hi Bonnie interested to know what maintenance dose of iodine is.Also how do you take it.Is it mixes with water.Will g it on the skin daily not work? Must it run thru the gut?
Hi Bev
A maintenance dose (for life) to support Thyroid health plus for the breasts, ovaries and prostate is 2 drops per day of Lugol’s 5% Solution. However to kill off gut bacteria, you need to go slightly higher for a short time. Taken in water, I don’t notice much of a taste.
Also why would you think it would help with gut bacteria, if you put it on your skin? That is very funny.
I find this whole blog here, hilarious. Some people read my whole testimonial AND DON’T GET IT. Their reply is like they didn’t even read it, when I included everything possible to encourage them.
That’s all I can do.
How about a little kindness? Sometimes when people don’t feel well they have trouble processing information. If you’re feeling better you must have a large reserve of grace and patience to draw from and extend to others who are not yet in your admirably healthy condition.
Yes!! M Szalewski you are so correct! Thank you for this.
Actually your blog is very interesting. I have a family friend that was just diagnosed with SIBO. I’m going to see what they recommend for her, and mention what I read from you. Thanks for the information, everyone should consider everything and everyone else’s testimonies on these issues, the doctor’s are not necessarily going to provide any real info, these things are not on all the regular radar…
Bonnie, thanks for offering some hope to those of us with SIBO. How did you take the iodine? Did you put the drops in juice or other liquid?
I’m anxiously awaiting your reply.
Thanks again,
Denise S.
Did your doctor really advise against probiotics? Which one are you using? I’m using Vitasolis probiotics and they work great!
For anyone who’s interested: https://offer.vitasolis.com/vitasolis-probiotic
Emma
Doctors don’t know everything. I said I had a stool test, identified the pathogenic bacteria, was sick for 8 years, took 13 hours to digest a meal, had terrible bloating and nausea, was called Gastroparesis and lost 70 lbs?
I wouldn’t wait 25 years to start looking for help.
Read my story again SLOWLY and see if it meets the criteria of SIBO. Lugol’s 5% Iodine was discovered in 1818 and was the only remedy doctors had for illness, it cured Syphilus in those days. It was made for internal use and treated a lot of serious health problems. As you MUST KNOW, IODINE KILLS BACTERIA and exactly what do you have in your gut? BACTERIA OF COURSE.
If I looked I might even be able to find Jacques Lugol’s notes on what this Iodine CURED 100 hundred years ago. You however will not benefit from that information because you can’t seem to understand it. Quit thinking about it and buy some, follow my instructions and be surprised. Or stay sick.
It’s up to you.
Wow why the harsh attitude, relax Bonnie
This article reads like most articles I’ve read on this subject. Take antibiotics but it probably won’t help. Change your diet but that probably won’t help either. It sure would be nice if there was a one size fits all fix, but that is clearly not the case. I have a 17 year old who was recently diagnosed with sibo. I was impressed that the doctor offered to test her for it. Treatment wise she only offered antibiotics. I personally think antibiotics is only a very short term fix if you don’t know why you have it in the first place. Does anyone know why they developed this problem?
The dr told me to stay away from fish with high iodine levels like tuna. I should just eat more tuna now after I read ur article. My symptoms are more like ibs with constipation. If I don’t find relief I’ll try the iodine. I also have thyroid disease so I’m wondering if iodine would b a good thing. Confusing, frustrating and u can’t plan anything because u never know how u will b feeling.
Please be very careful taking additional iodine if you have thyroid disease and have been asked to avoid iodine. It can be toxic. Talk openly to your Dr if you want to try Iodine, but please dont do it in isolation.
If your problem is IBS, then a low FODMAP diet works for 75% of people who have IBS.
I’m going to try the iodine. I guess sushi is a poor choice to prob ever eat with ibs and SIBO?
Laura
Did you try the Iodine?
Wow why the harsh attitude, relax Bonnie
This article reads like most articles I’ve read on this subject. Take antibiotics but it probably won’t help. Change your diet but that probably won’t help either. It sure would be nice if there was a one size fits all fix, but that is clearly not the case. I have a 17 year old who was recently diagnosed with sibo. I was impressed that the doctor offered to test her for it. Treatment wise she only offered antibiotics. I personally think antibiotics is only a very short term fix if you don’t know why you have it in the first place. Does anyone know why they developed this problem?
Hello
You say my article reads like most? Look up further and you will see my original story where I used Iodine to kill off the bacteria and it only took 3 weeks. This SIBO is usually the result of slow digestion.
Hi Bonnie did u change yr diet much when u started the iodine treatment?
No Beverly, I didn’t change anything. You need to read my Testimonial and MAKE NOTES on how to do it for yourself and what you need to have on hand.
The dosage and the type of Iodine.
good luck,
Beverly
Did you get started in the Iodine? If so what results did you have?
i TOOK BONNIE’S ADVICE, AND AFTER PROBABLY 15 YEARS OR SO OF SUFFERING, AND I MEAN SUFFERING FROM WHAT HAD ONLY BEEN DIAGNOSED WITH IBS,, I AM SEEING A PRETTY BIG IMPROVEMENT WITH TAKING THE IODINE.
I HAD BEEN TO MY GP, 5 GASTROENTEROLOGIST WITH ABSOLUTELY NOOOOOOOOOOOOOOO HELP. ALL DOCTORS DO IS TREAT SYMPTOMS…THEY DO NOT FIND THE PROBLEM AND TREAT THAT!!!
I DID GET TESTED AND FOUND OUT I TOO HAD SIBO.
YOU DON’T HAVE TO KNOW…………….ALL THE ANSWERS IN ORDER TO TRY IT, AND HAVE IT WORK.
AS BONNIE SAID, YOU CAN TRY IT, AND GET BETTER OR KEEP BEING SICK…………I CHOSE TO JUST TRY IT AS BONNIE SUGGESTED, AND AFTER ABOUT 3 WEEKS, I ACTUALLY COULD EAT A MEAL AND NOT HAVE TO TAKE MEDS AND LIE DOWN, AND YES SOMETIMES IT WOULD TAKE 5-6 HOURS OR MORE AFTER I ATE TO FEEL SOMEWHAT BETTER.
JUST TRY IT…………..THE ONLY THING YOU HAVE TO LOSE IS TO NOT BE SICK!!!!
BONNIE IS A MOTIVATOR,,,,,,,,,MAYBE A KICK ASS ONE, BUT SHE CALLS IT AS SHE SEES IT……AND HAS HELPED ME TREMENDOUSLY………..
THANKS BONNIE!!
Are you still improved/ing?
M Szalewski
Taking the iodine in 2008 eradicated my SIBO, how could i improve further?
It’s gone.
Bonnie
If anyone would like to know more information on getting rid of SIBO and IBS, feel free to e-mail me at: jeeplover1954@yahoo.com
Catherine
Interesting. Although I think my SIBO was triggered by taking a new probiotic and digestif at the same time I started taking fosomax,(I’ve stopped all 3 but the damage was done) I first thought I had a parasite. I even had the DNA stool sample screening; no pathogens there; I didn’t think SIBO bacteria visibly appeared anywhere except as a result of the SIBO breath test. My breath test said neg for methane & hydrogen separately, but pos for sibo when scores were added together. At any rate, Moda insurance refuses to validate the use of xifaxan for Sibo; they’ll assist with it benefit-wise only after one has tried numerous other antibiotics for IBS. Xifaxan is supposed to only work in the gut so theoretically, not as many side effects. I’ve given up the battle with Moda & have just started a naturopathic regimen of bitters at each meal & a berberine complex that will be rotated with either Neem or oregano oil capsules. I’ve been on the Fodmap diet for several months; I lost weight that I didn’t need to lose. And I didn’t find much else changed for me. Yet the other diets mentioned are diametrically opposed to some of the allowed foods in the fodmap diet. I remain confused about what else I can do. My bathroom business confines itself to the morning. I still wonder if I could have something else going on besides IBS & sibo. I will ask my naturopath about iodine. What a great discovery Bonnie made that worked for her. I’m open to other ideas……Thanks.
Insurance first balked at paying for my Rifaxamin/xifaxan, but my doctor called my insurance company and advocated for it. I guess that was part of an appeal process. It took about a week but I did get the med.
It worked only somewhat and i’m now weighing what my next step will be.
I did 2 rounds of 10 days each of rifaxim and all I got was a yeast infection on day 10 each time. It did nothing to help my SIBO. I have mostly gas and some bloating. I’m now doing Vivonex elemental diet for 14 days , and hope that will help. I think its okay to mix it with teas to make it more palatable and eat spinach broth or eggs for one meal while taking Vivonex.
I must say that some people take only Vivonex and no other food other than water for 14 days to 3 weeks, Very strict. but I just could not survive this as I am already underweight.
Why not try the Iodine?
At the beginning of the article it said that left unmanaged for several months SIBO usually causes several vitamin and mineral deficiencies.
I am not sure if I have SIBO but after taking strong antibiotics I have gas and belching. I did not take antibiotics to rid of this and I don’t know exactly how I can manage and overcome it.
Please can you advice?
Thank you very much
Joe
Hello Joe
Did anyone reply to your article above? In other words have found any help?
I’m another one who hasn’t had any luck with doctors, GI specialists included. They all seem to want to diagnose as IBS and be done with it. Terrible belching, gas, bloating and fatigue. I am over 60 and understand that digestion problems increase with aging but have noticed problems since before age 50. I do agree that some probiotics may contribute to SIBO but possibly the encapsulated ones that go through the small intestine without leaking contents may be the best – Renew Life being one of them. I will be asking for a SIBO test, have had CDSA’s before and in the meantime will try the SIBO diet and oregano oil/cat’s claw/olive leaf/digestive enzymes and Betaine before asking for an antibiotic. Iodine is worth a try. I have Hashimoto’s and am on NDT. What’s wrong with the doctors out there who can’t or won’t help with this?
I think my symptoms sound like yours. I had no idea that probiotics could make it worse. I’m also taking Linzess for ibs. I think that’s helped. I’ve been eating clean, no dairy, eggs, red meat, fermented anything and any sodas and I still have issues. I have hoshimoto as well.
Maureen
Have you tried Iodine?
I have sibo and have started seeing a CNC, doctors didn’t help at all. She has me on 2% iodine starting with 1 drop the first week and adding an extra drop each week for 5 weeks. I am a small person weighing only 103 pounds. She felt 5% might be too much for me. I’m on 3 drops a day now and I haven’t felt any difference yet. When this starts to work what differences will I notice?
Nancy
What will you notice? Well your SIBO should go away.
A 2% solution will take a lot longer.
Binnie
Sibo is not fun! After breath test that showed SIBO, GI dr did nothing except px Flagyl , then Bactrim. He did not see me – I would call his nurse who gave me wrong information. She said take fiber & Miralax daily. I did this for months til I realized it was making me worse, stopped both & was well! One & half year later, I have Sibo again. Taking Bactrim & just started Lugol this week! I am better today but you never know about tomorrow!
Emily
Bonnie, Am on week 13 of 2% iodine and what a difference. I feel so much better. I do the spit test each Monday and the last two weeks my spit just sat there and had no legs. My CNC says that is a good sign but we still have a way to go. Thank you for all your post and information, no one else has really helped me.
Nancy
Hi where are you reading information about iodine? I don’t see it anywhere on this post. Thank you
Holos Health in Boulder Colorado, practices Functional Medicine – Thyroid issues, menopause, nutrition and exercise. I’m currently being treated for SIBO with an array of supplements and a low fodmap diet – no antibiotics, please! It’s just been 30 days and I already feel much better. After losing 20 lbs of muscle, not sleeping and just a ball of anxiety and stress, things are now looking brighter. LK
Hi Bonnie,
I am very excited to try your testimonial treatment of: Up to 16 drops in 16 weeks of Lugol’s 5% iodine then dropping back down to 3 drops a day for maintenance. As well as the daily intake of the Natural Dessicated Thyroid USP pill as I have zero gut motility. Plus 200 mxg of Selenomethionine and 200mg of Vitamin C. I take a bunch of herbal supplements to simulate normal bowel functions with some degree of success, as well as 100 mg of Dicetel 2x a day, and 200mg of Xifafan 2x a day to reduce my SIBO symptoms, is that something that will get in the way of clearly seeing the effects of the Iodine solution Thyroid pil, vitamin C and selenomethianinel working? Should I halt what I usually take while trying your remedy? Or will the positive effects allow me to stop what I currently take afyer the fact?
I have SIBO, chronic constipation, and leaky gut. Chronic constipation since birth, gastric reflux intense enough to require Nexium as a PPI since I was 16, and SIBO and leaky gut since I was 22. I was recently fired from my finance job due to the smells my leaky gut was emitting in our open-air office all day every day. I am trying to get back into social as well as professional life and am running out of money and patience waiting for control of at least the methane smells before I do so, plus my results haven’t changed. I smell like: gas, feces food, and methane (which is very similar to pot when it comes out of the human body), and prevents me from going to social places or professional ones for obvious reasons. It’s been almost 2 years of the methane smells that have completely ruined my personal and professional life, 8 months since I was fired, and all the doctors want to do remove my Xifafan prescription so my symptoms can be really out of control I guess, and put me on low-Fodmap which doesn’t cure a thing.
I’m really hoping this testimonial of Bonnie’s will help me as well, as I pretty much do not have anything se medically I can try since I’ve been shut down by my family doctor on that end. Sorry fof he hugely long message I hope you’ll reply Bonnie, sorry for all the questions you’ve had to field so far.
I will be interested in following how you do, Gaelle! Your situtation sounds very severe and I’m sorry you’ve suffered for so long – I am in a similar boat with SIBO struggles for many years now…Please keep us updated as you start with the Iodine!
I was diagnosed with candida and sibo. I have chronic inflammation and diarrhea. I’m on flucanazole for the candida as it was pretty bad and now taking grapefruit seed oil for the sibo. Has anyone else tried this? I’m also on a biofilm defense to remove the layers of mucus these baddies are building. I’m incredibly nauseous all the time either from all these herbs and drugs or the biofilm im removing. I get metallic tastes in my mouth and the doctor says that is detox. I’m taking epsom salt baths but in pretty bad shape as I went downhill fast like all of you just got labeled as another head case or it’s just ibs. Now I’m suffering terribly. I am bedridden most of the time. Is anyone suffering from both? If so what are you eating? My doctor says my cholesterol is low but it’s because I can’t process fats seems like it just slips through me. I am only able to eat chicken, turkey, some beef, spinach, cucumber, zucchini and some olives. I try to have olive oil and coconut oil but just get terribly nauseous. I also don’t sleep like at all. I wake up in the middle of the night all the time as I found out the liver cleanses itself at 1 and 3 am and basically goes back down the intestinal tract which has so much inflammation. The other thing my functional doctor told me about is that proton pump inhibitors are the worse. They actually make your stomach less acidic. You rally don’t want that because the less acid you have you can’t properly break down food that passes to the small intestine causing food to essentially rot there if it isn’t chyme that is pretty broken down. I am not opposed to trying the iodine thing but I think I have to wait until I get some of this stuff cleared out. I also learned to be careful with probiotics they are not all what they are cracked up to be. I actually made my symptoms worse after taking this one that had a sugar starter. Thanks which is how the candida manifested. I literally had no lactobacillus in my body and so the bad guys are running wild. I had hookworms in 2011 so like many of you I think this is going on for a while. That was really tough. This is even harder. I went through three antibiotics earlier this year followed by a bad case of food poisoning and on and off birth control not to mention the stress of no diagnosis has left me in a really tough place. I can only hope and pray it will get better. I lost my job and tomorrow is my birthday and I just feel so down.
Hello Bonnie,
I was suffering from SIBO to the point I was afraid to eat anything unless I knew I would be around a restroom for several hours. After I did the 3 hour test at the Doctors office and come back positive. My insurance was dragging their feet to approve the Xifaxan. I finally just ordered the Iodine and started with a drop a day and slowly increased from there. All I can say is Thank You for this post. The stuff works great.
Xifaxan never got approved, doctor prescribed a different 10 day antibiotic, but after I waited a month and a half, for the insurance to get anything done. The iodine already had me back to pretty much normal. I took the prescribed medicine as more of a “go through the motions” deal, but saw no change from it. Anyone suffering from SIBO, Ludol’s Iodine is the trick.
I came across this post in the middle of the night. Desperate for help. Along with SIBO, having issues with histamine and possible vagus nerve damage. My hubby and I have become our own google doctors trying to figure this nightmare out. I finished two antibiotics a few weeks ago and had a honeymoon phase where everything was perfect, and now slowly all the symptoms are coming back. SOOOOO it’s ordered, will have to get the selenium as I missed that initially. Incidentally, I have always thought I’ve had a thyroid issue. A naturopath even had me on Armour, but it made me so dizzy. I’m anxious to see how this goes. Excellent info on titrating it up as well. Thank you for your testimonials. Would love to hear more.
Great information. One thing I didn’t seem to come across about the iodine was when to take it. At night, in the morning, with or without food?
Thanks for posting your successes and failures, all very helpful.
Hi Teresa, please follow the instructions on the bottle. Thanks.
After 4 days on Lugols 12% my sibo is already much better. I am quite sure that 3 drops per day will eradicate it completely in a month.
Take on an empty stomach. 3 to 4 times daily.
How do I find more info on this Ludols iodine?
What about a 7-year-old boy with sanfillipo and Sibo? What would be an option for him? I only give him soft foods in small pieces to avoid choking. He is losing weight but is very hungry and thirsty all the time. He does not have celiac.
Holy cow, thanks so much for this article. I am very happy with how informative this is, your citation of sources, and your impartiality when discussing various treatments or possible solutions.
I am 100% sketched out by “holistic” “doctors” who claim their miracle cures will solve all of your medical problems plus AIDS so it’s a miracle to encounter something like this. Keep up the great work and thanks do much!
Read The Iodine Crisis by Lynne Farrow.
So well researched, easy to read.
Iodine was the go-to for 100 years, but some doctors came up
against it for wrong reasons, and people got scared.
Re: Wolfe-Checkoff Syndrome.
Anyway, all the iodine info is there.
Marianna