Rheumatoid arthritis is one of the most common autoimmune diseases.
It affects up to 1.3% of the population worldwide, mostly women.
New research indicates that diet may influence traditional treatments for rheumatoid arthritis. This article summarizes the current science and recommendations.
What is Rheumatoid Arthritis?
Rheumatoid arthritis affects the structure and function of the joints.
A membrane called the synovium lines the joints, creating space and fluid for lubrication and movement.
In rheumatoid arthritis, the immune system attacks the synovium. This leads to an inflammatory immune response that causes pain, joint deformity and disability as it progresses (1).
The exact cause of rheumatoid arthritis remains unknown, but genetics and health of our gut bacteria appears to play a strong role.
That said, those who carry the genes may never develop the disease.
Summary: Rheumatoid arthritis is a condition in which the immune system attacks the lining of the joints. The exact cause is unknown.
Symptoms of Rheumatoid Arthritis
Common signs and symptoms of rheumatoid arthritis include:
- Joint pain or tenderness
- Redness or swelling in the joints
- Joint stiffness, especially in the morning
- Low-grade fever
- Fatigue
- Anemia (low red blood cell count)
- Firm lumps under the skin
- Poor joint mobility.
Rheumatoid arthritis symptoms may occur in “flares”, during which symptoms appear or worsen for a period of days to weeks.
If you’re experiencing two or more of these symptoms please speak with your doctor. Left untreated it can cause permanent bone and joint damage within the first year.
Summary: There are numerous symptoms of rheumatoid arthritis. Early diagnosis and treatment is key to preventing permanent damage to the joints.
Possible Foods to Avoid with Rheumatoid Arthritis

Medication is the first line of treatment for rheumatoid arthritis.
This includes non-steroidal anti-inflammatory drugs (NSAIDs), anti-rheumatic drugs (DMARDs), and corticosteroids.
However, early research and patient anecdotes suggest some pharmaceuticals and eating patterns can influence disease activity as well. This includes drugs such as adderall, and foods such as gluten and dairy.
Gluten
Those with an autoimmune disease, including rheumatoid arthritis, are more likely to produce anti-gluten antibodies (2, 3).
These are the same antibodies seen in celiac disease, which is why celiacs must strictly avoid gluten.
Researchers are unsure how gluten would directly impact rheumatoid arthritis, but it could be related to increased intestinal permeability or “leaky gut”.
Some small studies have found benefits with a gluten-free diet, while others found no difference (4, 5).
It seems that those who are producing anti-gluten antibodies will directly benefit from a gluten-free diet. For others, it will be an indirect benefit from cutting out junk foods that often contain gluten.
Eggs and Dairy
Early research suggests that egg and milk consumption may be problematic.
These foods produces certain immune antibodies and inflammatory markers associated with rheumatoid arthritis symptoms, at least in rodents (6).
However, these effects are related to food allergy, as opposed to gluten which is a food intolerance. Therefore unless the individual already had symptoms of egg or milk allergy, it’s most likely not an issue.
For this reason, if you suspect any food allergy or intolerance, see your doctor to be tested. Keeping a food and symptom journal is also helpful (a sample can be seen here).
Summary: Rheumatoid arthritis may increase risk of gluten intolerance or celiac disease. A gluten-free diet may offer symptom relief in those who are sensitive. Eggs or milk may also impact symptoms in those with allergies to either of those foods.
Foods and Nutrients That May Help
The addition of certain foods and nutrients may help reduce rheumatoid arthritis inflammation.
Most studies have used supplements rather than whole food sources, as a high nutrient dose is often required.
Note that patients should not add supplements without medical supervision due to the risk of drug interactions and side effects.
Omega-3s Fatty Acids
Omega-3 fats (especially DHA and EPA) from fish oil are known to have anti-inflammatory effects.
In a study of 140 rheumatoid arthritis patients, one group had 5.5 grams of fish oil per day while the second group (control) had only 0.4 grams of fish oil per day. All participants were also given several anti-rheumetic drugs throughout the study.
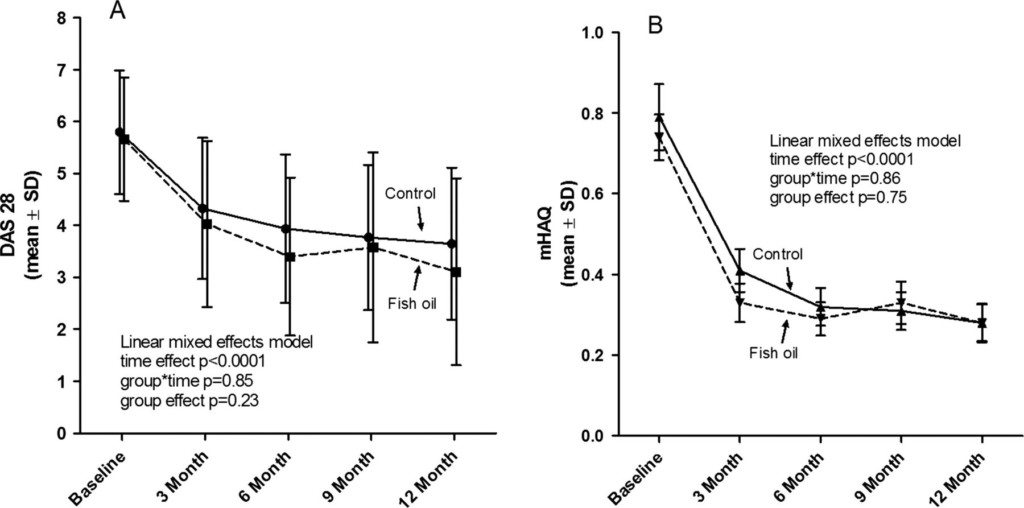
Both groups experienced a decrease in disease activity, but the first group had higher rates of remission (relief from symptoms) (7).
Change in rheumatoid arthritis activity (DAS28-ESR) and modified Health Assessment Questionnaire (mHAQ) over 1 year. Lower score is better. Click to enlarge.
So it appears that a fish oil dose of at least 2.7 grams of DHA plus EPA daily can boost the effectiveness of anti-rheumetic, at least in the first 6 months.
An earlier fish oil study also found similar benefits. Interestingly, the effect was much stronger when paired with a largely vegetarian diet (low in arachidonic acid) (8).
Note that fish oil supplements may interact negatively with certain rheumatoid arthritis drugs, so always speak with your doctor first.
Vitamin K2
New research suggests a specific form of vitamin K2 (also called MK-7) can help improve the effectiveness of rheumatoid arthritis medication.
Out of 84 rheumatoid arthritis patients, the first group received 100 mcg/day of MK-7 for 3 months, while the second group received dummy pills.
The first group had large improvements for markers of inflammation and disease activity score assessment. Additionally, MK-7 use increased the level of the active form of osteocalcin, an important marker of bone health (9).
It’s currently unknown if food sources of vitamin K2 have the same effects.
Vitamin D and Calcium
Those with rheumatoid arthritis are at increased risk of bone disease because of chronic inflammation, decreased physical activity, and use of corticosteroids.
While vitamin D and calcium do not appear to directly affect rheumatoid arthritis risk or symptoms, it’s important to maintain adequate levels to reduce risk of fractures (10, 11, 12).
Vitamin D is fundamental for good health and yet is the number one nutrient deficiency in the Western world.
Where adequate sun exposure is not possible, vitamin D + calcium supplements are strongly recommended. Food sources are also recommended, including fatty fish, egg yolks, fortified milk, and offal.
Summary: There are several foods and supplements likely to influence symptom management of rheumatoid arthritis. Fish oil and vitamin K2 have the strongest evidence so far.
What Is the Best Diet or Eating Pattern for Rheumatoid Arthritis?

Vegetarian Diet
Limited evidence suggests that vegetarian and vegan diets are beneficial on their own (13, 14).
In fact, many of the studies that endorse a vegetarian diet include more than one intervention for rheumatoid arthritis, such as fish oil, physical therapy or fasting (5, 8, 13).
Vegetarian diets also tend to be lower in omega-3 fats and vitamin D, nutrients that could be significant in rheumatoid arthritis (15).
Some may also find vegetarian diets overly restrictive if the sole purpose is for health reasons.
Paleo Diet
The Paleo Diet is an eating pattern that eliminates several food groups.
This includes wheat (gluten) and dairy, known to cause inflammation in some people.
Anecdotal (self-reported) evidence indicates a Paleo diet helps with rheumatoid arthritis. This is likely because those sensitive to either gluten or dairy will immediately notice improvements.
It’s also rich in omega-3 fats and cuts out junk food, which can only be beneficial.
Unfortunately the Paleo diet also recommends cutting out affordable, nutritious foods such as legumes and potatoes, which is unnecessary.
Mediterranean Diet
The Mediterranean diet consists of traditional foods that those in countries like Croatia and Greece ate before the 1970s.
It emphasizes fruits, vegetables, legumes, whole grains, olive oil, and seafood.
It’s shown promise for treating rheumatoid arthritis, possibly due to its favorable ratio of omega-3 fats to arachidonic acid (13).
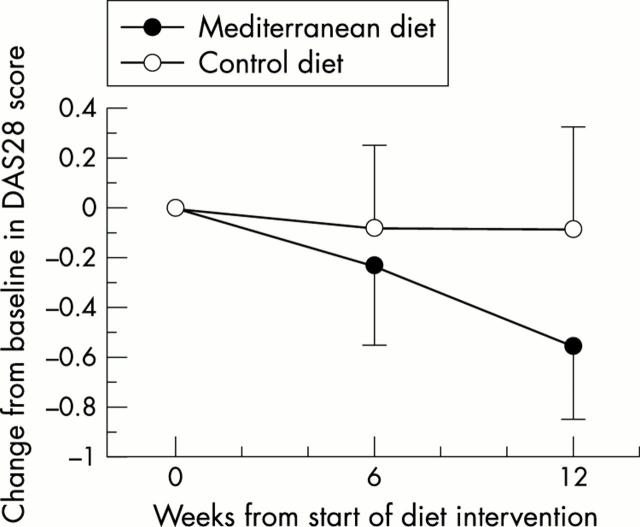
In a 3-month study of 51 rheumatoid arthritis patients, one group followed a Mediterranean diet while the control group ate a standard Western diet.
As you can see in the graph below, the Mediterranean diet group showed large improvements in physical function and vitality (16).
Rheumatoid arthritis disease activity (DAS28 score) at baseline and at weeks 6 and 12 of Mediterranean diet vs control diet. Lower score is better. Click to enlarge.
Summary: Limited evidence indicates a vegetarian diet is uniquely beneficial for rheumatoid arthritis. A Paleo diet may be beneficial for patients who are sensitive to gluten or dairy, but the additional food restrictions are unnecessary. The Mediterranean diet is quite well-studied in this area an appears the most useful.
Sample 3-Day Diet Plan for Rheumatoid Arthritis

The following is a sample meal plan based on the research summarized above.
It excludes gluten and incorporates principles from the Mediterranean diet.
Water is the preferred beverage with all meals.
Day 1
- Breakfast: ¼ cup rolled oats cooked in water (or milk), topped with ½ banana. (Oats are naturally gluten-free, but purchasing a gluten-free variety ensures the product was not exposed to gluten-containing foods during packaging.)
- Lunch: Lentil salad, 1 small apple.
- Dinner: 4 ounces oven-roasted salmon, 1/2 cup rice (cooked), ½ cup asparagus roasted in olive oil.
Day 2
- Breakfast: Smoothie made with ½ cup plain Greek yogurt, ½ cup almond milk, 1 banana, and a large handful of spinach.
- Lunch: Tuna and Cannellini Bean Salad.
- Dinner: One-Pot Mexican Beef Skillet with Quinoa.
Day 3
- Breakfast: Coconut Breakfast Quinoa.
- Lunch: Pumpkin & Carrot Risotto.
- Dinner: Pan fried chicken breast with roast potato and veggies.
Summarizing The Best Diet For Rheumatoid Arthritis
There is compelling evidence that diet changes can complement traditional medical treatment of autoimmune disease.
The Mediterranean diet in particular appears the most useful and well-studied diet for rheumatoid arthritis.
Patients with suspected food allergies or intolerances may benefit from eliminating gluten from their diet. Dairy and eggs may also cause problems, but this is based on weak evidence. At the very least it’s worth trialling a gluten-free diet for one month to see if symptoms improve.
Fish oil and vitamin K2 supplementation may also help combat inflammation, and are certainly worth a try alongside rheumatoid arthritis medications.
But due to the risk of side effects or drug interactions, be sure to speak with your doctor before starting a new meal plan or supplement.


Very helpful and informative…
This article has been copied and pasted and attributed to another author here https://healthlivinginfo.info/2017/06/05/best-diet-rheumatoid-arthritis-reviewing-evidence/
Thanks for pointing this out. They mentioned my name several times but they removed all links and have not linked back to my original article so I will complain to them.
(Herbal Cure For Rheumatoid Arthritis (RA))
I first lost my ability to stand up from a sitting position due to total body weakness. The physician I saw that same week ran a blood test and told me it appeared to be rheumatoid arthritis (RA) few weeks later i came across a testimony of one lady on the internet testifying about a herbal medicine home called perfecthealthherbalmedicinehome,run by dr sithuu, on how they cured her of rheumatoid arthritis (RA). And she also gave the email address of the herbal home and advised everybody to contact for help for any kind of diseases ,
Can we have the email so we can order this herbs please
so I emailed them,they replied and told me not to worry and they promised to cure me totally. Well i never believed it,,but i was so desperate,so i purchased the herbal medicine, well after used as prescribed, few weeks later i started experiencing changes,after 3 weeks usage i went to my doctor to confirmed if am finally cured of rheumatoid arthritis (RA),behold it was TRUE,i was totally cured , So friends my advise is if you have such disease or any other at all you can contact them via email: perfecthealthherbalmedicine @ gmail’com or website www’perfecthealthherbal’weebly’com
and I have two friends who have been cured by perfect health recently. they are very dedicated and knowledgeable. Thank you perfect health herbal medicine home …
Hi,
I was diagnosed with RA late 2015 and suffering till date. please advise.
I was always very healthy with a diagnosis of Hashimotos Thyroid about 7 years ago and minor allergies. I was given medication for thyroid. Then early this year starting having severe gastric symptoms, had diagnostic tests and found gastritis and hiatal hernia. Medication didn’t help and made it worse, so I started on Dr. Gundry’s diet, which is a combination of Meditrain, Paleo, wheat-free, lectin free, glutin free, and took lots of determination to follow. After 6 months, I lost 15 lb., and had no more gastric symptoms, have more energy, MD decreased my thyroid medicine, now have normal BP, no allergy symptoms, and highly recommend going off meds and choosing better food choices I am a retired RN, MS.
Hi Sandra, I’m glad the diet helped your symptoms. Keep it up! 🙂
Be careful with even certified gluten free oats if you have celiacs! I have celiacs and am cross reactive with the protein in oats, they give me a similar reaction as gluten.
Especially for people just starting to eat gluten free, recommending a meal based on oats is a bad idea, as they wont be able to tell if any digestive distress or other symptoms are lingering from gluten or being aggravated by the oats.
I’m in need of help I have severe pain in my hands. I went to the doctor but all test come back normal expect blood work that say I have RA.
Hi, you might be interested in the scientific literature on this topic as there were many diet studies a few decades ago. I’ve tried to summarize the literature here:
https://obscurescience.com/2018/11/28/dietary-causes-of-rheumatoid-arthritis/
In short, elimination diets were the most effective dietary approach and works for 35-40% of patients. Some of the key controlled trials demonstrating the effectiveness of elimination diets are:
* Placebo-controlled, blind study of dietary manipulation therapy in rheumatoid arthritis. https://www.sciencedirect.com/science/article/pii/S0140673686907749
* Hicklin JA, McEwen LM, Morgan JE. The effect of diet in rheumatoid arthritis. Clin Allergy 1980;10:463.
Food intolerances vary from person to person. Wheat and corn are the most common intolerances, but everybody’s intolerances are different. I hope that helps!
Rheum Arthr is NOT an autoimmune disease. Your body does not attack itself, rather it is a virus (symptom) caused by Epstein Barr virus. It is damaging you because the virus is being fed by certain foods. The object is not just to stop inflamm. but to stop feeding the virus. Some of the foods you mention are correct but you also need to eliminate…eggs, wheat, dairy, canola oil, alcohol, lower solium levels. Less red meat and other saturated fats is hard on the liver.
I am referencing Anthony William (medical medium).