Diverticulitis is an extremely unpleasant digestive disease.
Those diagnosed know it’s worth taking measures to avoid future episodes. Unfortunately, 1 in 5 will have another flare-up within 5 years (1).
This is a research-driven look at what diet changes may help treat diverticulitis, as well as some common myths about what foods to avoid with diverticulitis.
Note that each section in this article has a ‘summary’ box (like this one) to save time. Below this box is a contents menu to help you navigate directly to a particular section.
What is Diverticulitis?
Diverticulitis occurs when small pockets in the wall of the large intestine (colon) become inflamed or infected.
These small pockets or sacs – called diverticula – are formed when the muscles of the colon become too weak in certain areas. This causes them to push outward and form a “pocket,” which is common in the lower part of the colon.
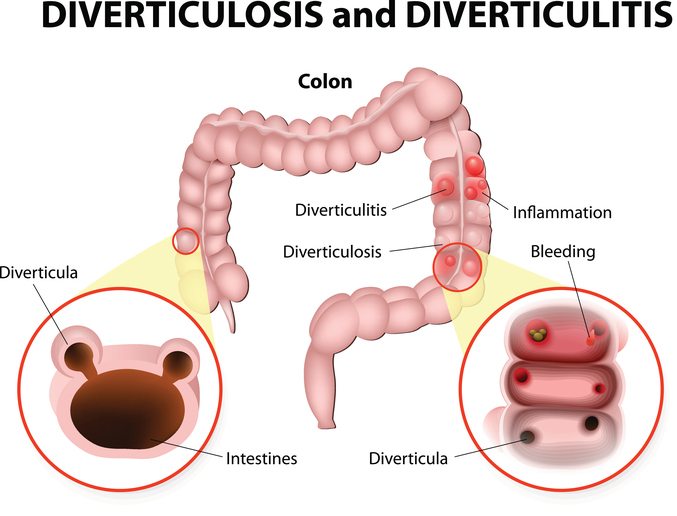
Diverticulitis becomes extremely painful during a flare-up. Even immediate surgery can be required to treat a severe case.
Diverticulitis vs Diverticulosis
Diverticulosis refers to having diverticula that have not yet become infected and painful.
This means diverticulosis always occurs before diverticulitis.
‘Osis’ refers to a medical condition, while ‘itis’ typically refers to inflammation or infection.
The risk of diverticulosis increases as we grow older, to about 70% of people aged 80 and above. Fortunately, it only progresses to diverticulitis about 4% of the time (2, 3).
What is Diverticular Disease?
Together, diverticulitis and diverticulosis are often referred to as diverticular disease.
The cause of this disease is complex and still poorly understood. Researchers suspect it to be a combination of numerous dietary habits, aging and genetic predisposition (4).
Summary: Diverticulitis occurs when small pockets in the lining of the colon become irritated and inflamed. Diverticulosis is simply the presence of these small pockets. Diverticular disease refers to either condition.
Diverticulitis Symptoms

Most are unaware they have diverticulosis until it becomes infected and painful (diverticulitis).
Symptoms can vary between individuals, but the most common are:
- Ongoing constipation
- Ongoing diarrhea
- Tender abdomen
- Cramping or bloating
- Fever
- Extremely painful bowel movements
- Blood in stool
- Nausea and vomiting.
Diagnosis is based on a history of symptoms in addition to some medical tests.
This can include blood tests, a colonoscopy or radiology as determined by your doctor.
Summary: Diverticulosis is usually symptom-free, however diverticulitis symptoms are typically severe and painful.
Would you like more information on how to eat for diverticulitis?
Tap the blue button below to download our “Eat This, Not That” list as well as additional resources for diverticular disease (it’s free!)
Treating Diverticulitis Flare-Ups and Using Antibiotics

Diverticulitis typically occurs as a painful “flare-up” with sharp pain and digestive symptoms.
It’s not uncommon for treatment to require a hospital admission, where the diet is heavily modified to allow the digestive tract some time to heal and inflammation to subside.
This includes a clear fluids diet for several days followed by a short-term “low-residue” or low-fiber diet and eventually progressing to normal foods.
In severe cases of diverticulitis, surgery and regular antibiotic use are required to overcome the infection. However, recent research suggests that aggressive antibiotic treatment is overused, particularly in less severe cases (5, 6).
This is why diet and nutrition are incredibly important for managing this disease, not only during a flare-up but afterwards as well.
The remainder of this article focuses on long-term dietary management of diverticulitis.
Summary: Acute flare-ups of diverticulitis are treated with a clear fluid and low-residue diet for several days to allow the gut time to heal. Antibiotics are definitely warranted in severe cases, but less so otherwise.
Diverticulitis and Probiotics

Probiotics are bacteria we eat for health benefits.
Studies show that a variety of different probiotic strains are effective in reducing symptoms of diverticulitis. Particularly those of Lactobacillus casei and Lactobacillus paracasei (7, 8, 9).
In this chart, you can see that a high-fiber diet plus the probiotic Flortec appeared especially useful for short-term abdominal pain (8):
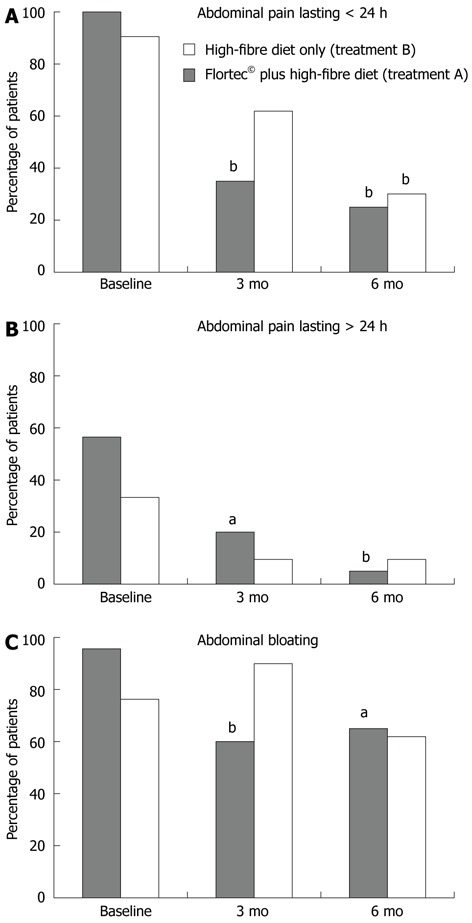
Probiotics have also been successfully combined with the anti-inflammatory drug Mesalamine to help reduce symptoms of diverticulitis. However, it’s uncertain if they reduce the risk of recurrence (10, 11).
Probiotic Sources
The best food sources of probiotics are fermented foods, such as yogurt, quark, Yakult, sauerkraut, kefir, kimchi, tempeh, and miso.
Probiotic supplements are also a great option, but recommended strains and dosage have yet to be determined. Always buy probiotic supplements (as with any supplement) from a reputable and trusted source.
Summary: Research suggests a variety of probiotic strains are effective in managing diverticulitis symptoms. Both fermented foods and supplements are useful sources.
Is It Better to Follow a Low-Fiber or High-Fiber Diverticulitis Diet?

Fiber is an indigestible carbohydrate we get from plant foods.
It was always thought that diverticulosis was caused by inadequate fiber intake. However, newer studies suggest it probably doesn’t prevent the diverticula forming in the first place (12, 13).
That said, it most likely does help prevent diverticula becoming symptomatic (diverticulitis).
One observational study found that those who ate 25 grams or more of fiber per day had a 41% lower risk of being hospitalized for diverticulitis compared to those who ate less than 14 grams per day (14).
Another study that followed more than 690,000 women without diverticular disease found that each additional 5 grams of fiber per day was associated with a 15% reduction in risk of diverticulitis (15).
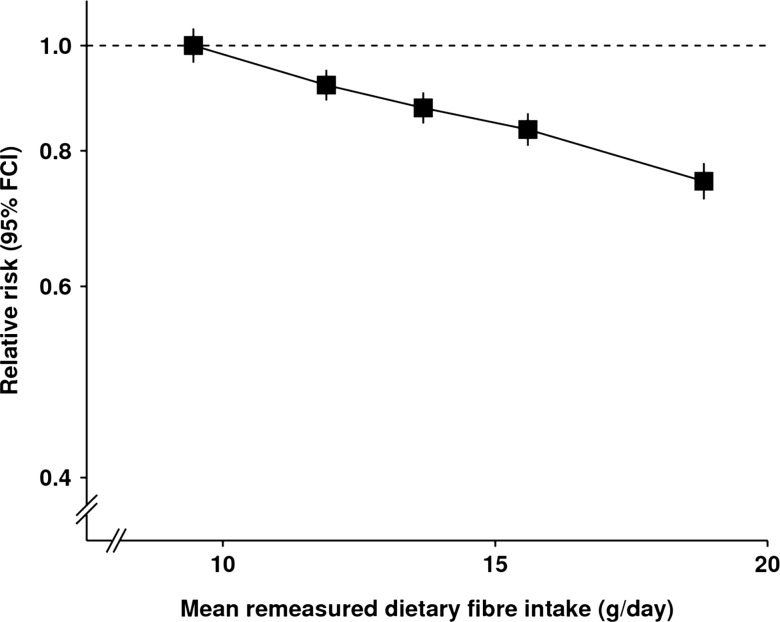
Considering that fiber intake has other known health benefits, such as promoting regularity of bowel movements and maintaining a healthy gut bacteria, it makes sense to recommend a high-fiber diverticulitis diet.
Additionally, today most people only consume half of the recommended amount. Women should aim to get at least 25 grams per day, while the average man should have at least 38 grams per day (16, 17).
However, with that said, there is no reliable evidence that a high-fiber diet improves symptoms or prevents complications in diagnosed cases of diverticulitis.
A recent review of 19 studies (9 looking at dietary fiber, 10 at fiber supplements) was unable to make any firm conclusions because each study varied so greatly in how they were conducted, the type and amount of fiber used, among other things (27).
The authors’ conclusions were:
“The presence of substantial methodological limitations, the heterogeneity of the therapeutic regimens employed, and the lack of ad hoc designed studies, did not permit a summary of the outcome measure. Thus, the benefit of dietary or supplemental fiber in SUDD (symptomatic uncomplicated diverticular disease) patients still needs to be established.”
So there is no definite answer, which helps explain why the Danish and Polish guidelines recommend fiber supplements, whereas the Italian guidelines argue somewhat the opposite (28).
Basically fiber supplements are an option, as is a high-fiber diet, but unfortunately a bit of trial and error is the only way to see what sits better with you. Many people report doing better on a low fiber diverticulitis diet, which overlaps heavily with a low FODMAP diet (more on that below).
And as mentioned above, a low-fiber diet is definitely recommended following a flare-up. After a few days on a clear fluids diet, you can progress to boiled and soft foods, including cooked fruits and vegetables (without skins), as you slowly increase your fiber intake.
Summary: A high fiber diverticulitis diet is strongly associated with a reduced risk of developing diverticulitis. However, for those who already have diverticulitis and need to manage symptoms, it’s unclear whether a high or low fiber intake (supplements or food) is more beneficial.
Diverticulitis and Vitamin D

Vitamin D is a critical nutrient for human health, best known as the “sunshine vitamin.”
There is increasing evidence that our vitamin D status may influence risk of gastrointestinal diseases such as Irritable Bowel Syndrome, Inflammatory Bowel Disease (including Crohn’s disease) and diverticulitis (18).
A recent study in those with diverticulosis found those with the lowest vitamin D levels were significantly more likely to experience a diverticulitis flare up (19).
So it’s important to have your vitamin D levels checked with your doctor, particularly if you don’t get much regular sunlight exposure.
Unfortunately, natural food sources of vitamin D are not very useful if you have a deficiency. This is one of the few instances where supplementation is far superior to food.
Summary: Low vitamin D levels are linked to increased risk of diverticulitis. Get screened for a deficiency with your doctor.
Are Nuts and Seeds Really Diverticulitis Foods to Avoid?

A simple search for “foods to avoid with diverticulitis” or “what not to eat for diverticulitis” will show you nuts and seeds, corn and popcorn.
You will also find recommendations to avoid seeds in fruits and vegetables like tomatoes, zucchini, cucumbers, strawberries and raspberries.
In fact, for years we’ve been taught these foods can literally get stuck in diverticula, causing irritation and eventually diverticulitis.
But this theory has never been proven, and research actually shows no link.
A large study in 47,228 men found no associations with nut, corn, or popcorn consumption and diverticulitis, after 18 years of follow-up (20, 21).
In saying that, anecdotal evidence (patient reports) consistently suggests that seeds are an issue, such as sesame seeds on a bread roll.
So evidence is really a mixed bag, it might be better to err on the side of caution and avoid seeds at least. I wish I could give a more concrete recommendation but there really is no consensus at this stage.
Summary: Nuts, seeds, corn, popcorn and fruits and vegetables with seeds may be safe to eat with diverticular disease, but the current scientific evidence clashes with patient reports. It might be a good idea to avoid seeds just in case.
What About Red Meat on a Diverticulitis Diet?

The idea that red meat intake increases diverticulitis risk is unproven.
It was formed on the back of observational studies that found vegetarians were much less likely to develop diverticular disease than the average person.
A recent study also found that a “Western” dietary pattern (including red meat, refined grains and high-fat dairy) was associated with an increased risk of diverticulitis versus a “prudent” diet high in fruits, vegetables and whole grains (22).
But the reason vegetarian and vegan diets are advantageous is because they’re almost always higher in fiber than the typical Western diet. Additionally, non-meat eaters tend to be more health-conscious than the average person (23, 24, 25).
So it’s considerably more likely the benefits lie in eating more fiber, rather than cutting meat or animal foods.
That means you should follow whatever eating pattern will help you eat more vegetables, nuts and other high-fiber foods. If going vegetarian will help you achieve this, and is something you can do long-term, then do that.
Summary: The idea that red meat increases risk is unproven. Vegetarian diets appear protective because they are typically higher in fiber.
Can a Low FODMAP Diet Help Prevent Diverticulitis?
Newer research is finding that a low FODMAP diet may help prevent recurrence of diverticulitis.
In fact, researchers believe that a high-fiber diet (basically high in FODMAPs) may be linked with IBS symptoms. Because of this, some recommend a low FODMAP diet for people with diverticulitis as well (26).
This makes sense given that the literature around benefits of a high fiber diet in diverticulitis is severely lacking (discussed in a section above).
Some high FODMAP foods to avoid include:
- Wheat
- Onions and garlic
- Certain fruits, such as apples, peaches and pears
- Certain vegetables, such as asparagus, Brussels sprouts and cauliflower
- Dairy foods
- Legumes
See this Beginner’s Guide to the low FODMAP diet to learn more about this fascinating diet.
Would you like more information on how to eat for diverticulitis?
Tap the blue button below to download our “Eat This, Not That” list as well as additional resources for diverticular disease (it’s free!)
Summary: New research shows that following a low FODMAP diet may help prevent recurrence of diverticulitis.
Diet Plan (Menu) For Diverticulitis and Diverticulosis
This is a sample 4-day meal plan or menu for diverticulitis diet based on recommendations outlined in this article.
But it’s certainly also appropriate for the average person with diverticulosis who wants to minimize the risk of getting diverticulitis.
Note that I’ve modified this to be low FODMAP, as the new evidence strongly indicates minimizing problem FODMAPs is beneficial for diverticulitis patients. Check out the full list of FODMAP foods and drinks, plus their recommended portion sizes.
Portion sizes of low FODMAP foods is extremely important for a diverticulitis diet, so please make sure you are not exceeding the recommendations. You can also find additional low FODMAP recipe ideas here.
Diverticulitis Recipe Ideas
Day 1
- Breakfast: Quinoa Porridge with Berries and Cinnamon
- Lunch: Tuna salad with baby spinach, rocket, tomato and cucumber dressed with olive oil and apple cider vinegar
- Dinner: Tempeh stir fry with veggies (carrot/broccoli heads/Asian greens/veggies working well in stir fries)
- Snacks: Carrot sticks with cottage cheese
Day 2
- Breakfast: 2 eggs (made any way you prefer) on 2 x plain white gluten-free bread + 1 cup of spinach/aragula/rocket drizzled with olive oil and salt.
- Lunch: Last night’s leftovers
- Dinner: Baked or pan fried chicken with low FODMAP roasted veggies
- Snacks: 10 almonds/pecans/walnuts or 20 macadamias
Day 3
- Breakfast: Gluten-free bread topped with cottage cheese and smoked salmon
- Lunch: Low-FODMAP Tomato and Leek Frittata
- Dinner: Chicken/beef/fish (any quantity) +1 tbsp ketchup/BBQ sauce/mustard + 2 small boiled potatoes + ½ cup broccoli.
- Snacks: 1 orange or 2 small kiwi fruit
Day 4
- Breakfast: ½ cup of oats + 10 raspberries/strawberries/blueberries. Add water and microwave to make warm porridge, or just add lactose-free milk/almond milk for cereal
- Lunch: Low FODMAP Minestrone
- Dinner: Salmon baked in foil in the oven with sliced lime and chilli on top, served with 1/2 cup steamed zucchini and squash, and boiled basmati rice.
- Snacks: 2 rice cakes topped with peanut butter and 1/2 banana
Remember that you may also want to consider vitamin D and/or probiotic supplementation alongside a health eating pattern.
Summary: Treating Diverticulitis with a Diverticulitis Diet and Food
There is no doubt that fiber is good for you, and that a high-fiber eating pattern may help prevent diverticulitis occurring in the first place
However, there is very little evidence it helps minimize symptoms in those who have already been diagnosed.
In fact, newer research suggests that following a low FODMAP diet may be the most beneficial in preventing diverticulitis from recurring.
There is also some evidence that probiotics (particularly some strains of lactobacilli) are useful for treating symptoms. However, researchers are unsure they help prevent recurrence.
Also consider vitamin D supplementation if you have low levels.
Lastly, there is little evidence that cutting meat or nuts and seeds from your diet is beneficial. If anything, nuts are more likely protective, while seeds are still a bit of a mystery.
Still, each person’s experience is different. You may find that certain foods worsen your symptoms and are best avoided.
Remember that diverticulitis is a disease influenced by many other factors too, including obesity, stress, physical activity levels and smoking status.
I hope this article cleared up some of the confusion for you. Let me know what helps or aggravates your symptoms in the comments.
What Can I Eat, What Can’t I Eat For Diverticulitis?
Tap the blue button below to download our FODMAP “Eat This, Not That” list as well as additional resources for diverticular disease (it’s free!)


I’ve heard that psyllium husk is a good way to get your fiber and help with Diverticulitis. is this true?
Yes Roy psyllium husk is good: https://www.dietvsdisease.org/best-fiber-supplement.
And higher fiber appears beneficial for this condition.
I find it helps, but hate the powder. Tastes like gritty glue to me. Solgar do capsules and I prefer those, but remember to drink plenty water.
I WAS WONDERING IS IT OK TO EAT CHICKEN AND RICE WITH HAVING Diverticulosis and Diverticulitis
Dear Barbara, I had my first “attack” a few weeks ago, and have been trying to create a diet ever since. I am a chef and foodie so it has been challenging. I find that chicken and rice works great for me. I put thighs, bone-in ones, that I trim of fat, then I sear skin side down in a non stick pan. After that I put them in a crockpot wit a bit of garlic, a bit of unfiltered cider vinegar, some broth and pitted prunes (which for me gives me the fiber …but if you are experiencing other issues, you may wish to avoid this.) Bay leaves, thyme too, seem to work fine. This dish is delicious with white rice, like Jasmine. Other chicken and rice dishes should work too. Oregano, and ginger may have medicinal qualities, and could add nice flavors, not together)…personally am trying to avoid anything too spicy for a while. Roasted hard squash cubes like butternut are great too as a side flavor. I use Himalayan pink salt as my only seasoning, too. Organic coconut oil, when needed.
Greg, I am wondering if rice would be able to be chewed enough to go through the digestive tract without getting into one of the pockets of colon wall?
Rice getting stuck in the pockets has not been proven. The benifits of fiber are pretty clear. Remember, if concerned you can blend food and to make cream style soups. In my experience blended soups will require seasoning (like oregano) to add flavor.
With any white rice you can cook it with a lot of water and get a soft porridge, add more water and it will be a soup. The Chinese call it congee or jook, add soy and other stuff to it and it is delicious. In an attack I turn to this for something to eat.
Just got out of th er with diverticulitis and uti diagnosis. Clear diet sounds daunting but I will do it. Greg, do you have other recipes? I need inspiration. Feeling really down.
I am in hospital with my first flareup of diverticulitis. I feel totally confused with the dietary advice – high fibre or low fibre?? Meat or no meat? Broccoli or not??
I too was in the same situation as you about a month ago. My dr. didnt bother to tell me after having a liquid diet for a few days to switch to a low fiber diet for a couple weeks and work up to a high fiber diet. I am vegetarian and have since gone vegan. For me it feels the only way I can get enough fiber. Good luck!
My mom is in the same boat. She sticks to a primarily low fiber diet but does take the husk for fiber. I stumbled on this page and will show her but she is adamant about eating only canned fruits and veggies, no beef, no nuts.. ugh!
Susan, I’m vegan too and I’m wondering how you are doing now and if you have any favorite recipes.
I’m vegan too- 8 years now with no problems in my diverticular. My gastro said I have a bad case of diverticular and have gotten worse but only recently had a real attack-no fever but queasiness especially after being prone like sleeping. I wake up with aches in my tummy. This was triggered by some Vietnamese peanuts. Little hard ones coated with spicey spice. I go on liquid diet for a few days, eat mashed stuff for a while, start adding regular food in regular portions and it returns. I would like to get rid of this before it gets to the fever and antibiotic stage. I’m 76 so it may also be age.
High fiber, since my first attach last month and second one three weeks later, I am trying to eat grilled vegetables, soup (I blend the soup), chicken, first thing in the morning drink water and lemon and drink mix one table spoon of psyllium husk in OJ or water for high fiber…it is a process and we will learn what to eat….wish you good health…
Stop eating fiber, it just irritates the bowels. If this continues with your high fiber diet try switching to a keto diet for awhile and see if that helps. Fat is low residue and passes quite nicely through the digestive tract.
You wrote about having two diverticulitis attacks within a short period of time on a web site. Was surgery recommended? Have you had surgery?
please help me. what should I eat? When can I start eating btocolli
with in the week ,i was in hospital ,the pain was unbearable. …..I started drinking water 8 or 9 glasses a day…plus took my meds ordered by the Dr. i tried broth but but ..was terrible ,,so i found i could eat potato,(baked,french fries,boiled in chicken broth .mashed . White Bread with Bologna …..sure this varies with each person,my Dr said eat bran cereal …going to try this …ok today ,,,but has taken me 2 weeks to fill better ,,,,yes i will watch what i eat ,,,OR how i eat it ..mostly what i have read i can eat any thing long as its SMASHED up …..just me ….
This is so conflicting, seems everyone has a different opinion on this subject. I guess you have to experiment for your self and see what works best. For me nuts definitely mess me up. Idk wtf to eat at this point lol
I was surprised by some of the suggestions for the diet above…cucumbers? I have eaten a couple of things (by accident) with a few seeds and boom, my pains were back. The ER nurse told me she also had diverticulitis – no nuts, no seeds & keep the antibiotics handy for the occasional flare up. When I get a flare up I go to mac & cheese, beef broth, clear apple juice but someone needs to come up with a recipe book for us when even a simple salad can be a hazard to our health. All I can say is thank God potatoes are safe!
I just got out of the hospital Jan. 2, 2018 with a severe attack of diverticulitis so am reading all your messages. Yes I’m finding diet info very confusing so finally talked with a nurse today from my Insurance Company. Yes avoiding anything with seeds. Believe for me right now is a low fiber diet until I see my GI doctor the end of the month. This attack came totally out of the blue with no stomach pain at all but a lot of hemorrhaging and diarrhea. Boy it scared me to death. I’m also going on a few websites for different opinions and comments.
I cannot eat mixed nuts anymore, apparently. Or maybe I just didn’t chew them enough. That seemed to cause my last flare-up a few days ago. I’m getting better, though. Thanks for leaving your comments. It’s encouraging to hear what people are doing, and not doing. I added vitamin D and probiotics to my diet.
The worst attack I ever had came after eating a few handfuls of cashews while I was on a four-hour Greyhound bus ride. I had to go to the emergency room first thing in the morning after I arrived. I think the flare up and having today is because I’ve had a habit of having some raspberry jam on a piece of toast most mornings and the seeds are what are hurting me. Occasionally I’ll let myself eat some nuts like pecans, but I make sure I chew them extremely thoroughly. I do avoid nuts because I think they are major cause of a flare-up. I haven’t been to emergency today because it seems to have settled down and I’ve taken something for the pain, however I’m a little bit concerned that maybe I should be getting antibiotics. I’ll see how I feel tomorrow. Thank you for your post it’s very encouraging and helpful to read everyone’s posts on here.
I’m with you on this one. I’ve had 3 attacks in 4 months. I have no idea what to eat either. So confusing
This life long diet is what works for me:
………I cannot eat anything that has seeds or nuts in it, hard chips or any hard snacks, raw or hard veggies that are hard/stringy etc. such as celery (unless juiced or blended) (and I love celery but I do eat it thinly sliced and cooked in soups”..Anything like tomatoes, jalapeno’s or zuccini etc. , I have to de seed!!
I also do not eat pasta dishes and pizza in most restaurants unless they use tomato sauce without seeds!! That’s pretty much all of it and usually am ok. I can get symptoms very quickly when I stray from this diet, so I watch it closely since I’m not a big fan of liquid diets for several days.
Sounds delicious Greg! Thank you for sharing your recipe.
Sometimes I think, in my case, it is stress as stress for me goes directly to my gut.
Stress is a huge risk factor and trigger. Mind-gut connection is very real thing
Thanks. I asked my doctor about this and she said it had no impact. I have had two attacks in 4 months and I am under tremendous stree.
I’ve had two diverticulitis attacks, last one was on two antibiotics for 10 days. I can tell you in my case, mine is caused by STRESS. Too much of it. If something ‘scares’ me, even a little, I feel my gut spasm. A direct connection. They don’t call your gut you 2nd brain for no reason.
I’m with you on this one. I’ve had 3 attacks in 4 months. I have no idea what to eat either. So confusing
I’m so bummed about my. Flair up. So much conflicting imfo the med are murder for me I don’t know what to eat with broth no broth bone veg jello cooked potato idk very bummed
Me too. I was hospitalized a week April 2017 with diverticulitis and a pinhole in my large intestine. I have had 2 flare ups since then. Antibiotics – Cipro & Flagyl – that made me feel really bad but did help with the diverticulitis. Thankful I did not have to have surgery as I had no eating or drinking in Hospital and inflammation subsided. But I then developed thrush. Another battle. I am constantly having twinges in my left lower abdomen. And trying to figure out foods is very confusing. I am trying to stay low fiber for now because seems like when I try to up fiber – I start small flare ups. This is sooo not fun. Just tell me what to eat and not eat and I will do it. Must be different for everyone.
I agree that stress is a major factor..when you get stressed your whole body tenses up, and it is hard to eat right and digest well.. my first flare-up was in 1989, I had a very stressful job, and a boss that was on top of everything I did.. he was new at his job and didn’t like women to run the shop.. so I was a target and it really got to my gut.. I was out of work for over 2 weeks on antibiotics, and on liquids for 12 days..then started on a low fiber diet and was fine til 1992..Then that same boss really cracked down by setting up his office in our bldg.. STRESSED out so bad.. I kept cool around him, but again another flare-up, and at the same time he fired me.. I was at work, sick and in pain..Anyway after all these years of never going thru that again.. I am going through another flare-up and it is horrible.. I watch what I eat, and do love fruit and veggies.. everything in moderation.. but I did have corn on the cob from the local farm, every day.. for 4 days in a row..got constipated and now suffering with diverticulitis.. I just thought at this age I developed IBS cause I worry so much..nope… the big D is back and so, on antibiotics, liquids and so hungry but nauseous too.. I pray it heals fast cause I caught it fast… I think.. To all here, feel better.. pay attention to the signs that your body gives you.. Everything in moderation..
I totally agree with you, Stress is the major cause in my case. My surgeon agree, he gave me a laxative to take every 3rd day to clean the colon . that really helps me a lot. I find that too much fiber cause pain and bloated stomach, so I try to balance my food intake. Starchy food and sugar definate no. I treat myself once in a while? I take probiotics every day. Hope you all feel better soon.
Me too! I eat healthy and am I fitness instructor that works out regularly. I had first flare up 3eeeks ago and now today fever chills body aches and pain. Horrible!
Hi! Had my flare up one month ago…and am almost scared of eating now. I get nausea, upset stomach and heaviness in my lower abdomen. I too work out, eat healthy (no meat for six years), but have enjoyed eating always…now, not so, too afraid of diverticulitis flare up. Reading these comments is helping as I think I am going nuts (literally).
Anybody else lost weight???
I have lost 15 lbs. I just suffered my first attack. I was in hospital 5 days. First 2 days they kept me knocked out till the antibiotics could start working. I’m home now and have not stepped outside for over a week. I can’t eat but a few bites at a time. I feel nauseous all the time. Glad i had retired so for once i can take my time getting better.
Yes, drop fast and then not eating for a while after
No, I keep gaining and hardly eating
I’ve dropped almost 40lbs in just under 2 mos.. likely it’s because I dropped my weakness.. soda.. from my diet. I’m to afraid to eat due to “the unknown”. I’ve had liquid diet 3-4 times since diagnosis. Eat 1 wrong thing and boom pain and discomfort is back. From what I’ve read so far.. this condition is pretty well individualized so I’m keeping a food journal and slowly introducing new items.. so far red meat is a no go :-(.. small bits of kiddos chicken nuggets seem ok lol.. not a fish fan but going to try that as well.. like other comments I’ve read I think moderation is probably the biggest thing for me. Stress is more than likely a factor as well.. it feels really helpful to have found others that are going through this bummer ordeal.. thanks
Yes – I am learning a lot from all these comments. We are not alone. Diverticulitis is no joke.
I took 2 ideas from you: keep a food journal and eat in moderate proportions. Easier said than done unfortunately.
Me too Brian…. I just had my first attack on Friday and I know it is the result of the very long and sustained stress at work. I am also a cook in a vegetarian kitchen. So I hope with paying more attention to my diet and reducing the stress it will make a difference. This will be challenging for me as I am sure it is for everyone.
Me too! I feel every emotion in my gut and have tried not to, to no avail..
Please give me some advice on rice and grains such as quinoa as I am thinking they are harder to chew well and might end up going through digestive trace whole and get stuck in the pouches? I know I need to increase fiber and avoid some vegetables with skins. Thank you
(I think this post is right on, except if you are doing the liquid diet for a few days.)
“For me, I have to avoid raw dense vegetables such as broccoli, cauliflower, carrots and any fruit with skin such as apples. I’ve had several flare-ups thst landed me in the hospital and its always been the raw veggies. So now I cook them to soften them and they don’t bother me. Nuts, seeds and popcorn have never been an issue for me.”
(I don’t think raw Vegetables are something I would recommend unless they were blended. Fruits without skin are probably fine. Also cream style soups can be easily made using a blender. Even canned soups like “progresso” brand and such can be blended. These will require some seasoning like oregano and such to add flavor.)
Hi Joe
In the midst of recovery from a nasty flare up with fever, diagnosed late 2015 with Pan Diverticular Disease following an initial acute episode, hospitalisation, IV antibiotics etc.
My regular diet is high in fibre, fish, chicken occasionally, almost never red meat, love nuts and seeds.
My question is regarding the recovery diet following a flare up. In this flare up, I have only taken clear fluids for 24 hrs, added dry rye toast when taking antibiotics, ( metronidazole/Augmentin Forte) miso, herbal teas.
Would value your input regarding progressive steps in the recovery diet.
Cheers Sandi
Hi Sandi,
I’m not allowed to give direct medical advice unfortunately. You have to follow your doctor’s instruction, so I’m assuming (hoping!) your doctor gave you recommendations.
The typical protocol is clear fluids diet, then fluids, and then soft food and then regular food once more.
I also suffer and find that if I do a once a week for a day “cleansing” of clear broth and liquids, it helps keep things working well
Hi Joe
In the midst of recovery from a nasty flare up with fever, diagnosed late 2015 with Pan Diverticular Disease following an initial acute episode, hospitalisation, IV antibiotics etc.
My regular diet is high in fibre, fish, chicken occasionally, almost never red meat, love nuts and seeds.
My question is regarding the recovery diet following a flare up. In this flare up, I have only taken clear fluids for 24 hrs, added dry rye toast when taking antibiotics, ( metronidazole/Augmentin Forte) miso, herbal teas.
Would value your input regarding progressive steps in the recovery diet.
Cheers Sandi
Sorry i was slow to reply, i replied to your later comment
For me, I have to avoid raw dense vegetables such as broccoli, cauliflower, carrots and any fruit with skin such as apples. I’ve had several flare-ups thst landed me in the hospital and its always been the raw veggies. So now I cook them to soften them and they don’t bother me. Nuts, seeds and popcorn have never been an issue for me.
Excellent suggestion.
Hello,
I’ve been searching for a list of the best things to eat after being on a liquid diet for a while. The symptoms have subsided and I’m nervous about reintroducing food. I’ve been existing on bone broth, herbal tea and lemon water. I’ve gotten so many conflicting views on what to eat and what not to eat that I’ve worked myself into a bit of a paralysis.
I had a flare up 3 weeks ago. Since then I have been on 2 antibiotics, Cipro and Flagyl. I also was told to do the liquid diet for 3 days and then a low-residue diet for a week. So that consists of the white rice, applesauce, bananas, jello, no caffeine, broth and saltines. I have tried to reintroduce higher fiber foods over the last few days and some are agreeing with me and some aren’t. It seems like any processed foods, ie Uncle Ben’s long grain and wild rice are not agreeing with me where as cooked veges are ok. Last night I roasted some beets. I only had like 2 bites, cause I am afraid too.
Best wishes! I am glad I found a blog because there is not a whole lot of info out there on our disease.
Hi Nella and Lynne,
Progress onto boiled and soft foods including boiled vegetables.
If you are trying foods and many are not agreeing with you, work with low FODMAP foods first as they are just a bit more gut-friendly to a sensitive tummy: https://www.dietvsdisease.org/low-fodmaps-food-list/
Hey Joe!
Great post, great to see large study cohorts and plenty of references where possible. I will definitely be arranging to come visit you for one on one consult if I ever develop Diverticulitis (as Diverticulosis I probably won’t have any symptoms just yet ^_^ ).
Keep up the great work!
Marlo Sarah Elms
Thanks Marlo, I really hope you don’t get it!
i am currently going through flare up taking antibiotics. i have battled stomach problems since i was a child., seeds i don’t eat cause they cause a flare up., what has help me a great deal to only have a flare up maybe 1 a year is green juice., nappa cabbage, kale. celery. cucumber carrots, apples., has help me a great deal. also listen to your body. you start feeling pressure on left side at least a week before a flare thats letting you know to eat less binding foods and you may even need to take stool softener to get things to move out. when it gets to stress remind yourself of this, you cant control things in your life, and if you are sick or need surgery, then you will wont be able to get anything done. so take care of yourself 1st cause if you are sick you cant take care of anything else. also i don’t really eat meat, what i am eating now flare up is trader joe organic chicken broth, i water down a bit add trader joe water crackers or sour dough bread to make it soft mushy., and in a few days i will grind up kale. cabbage. carrots, celery, cilantro and let it cook for hours and then strain it and have that. this is a crappy disease, but there are more worse illness out there. the positive to this is to listen to your body a week before you have a flare up you get pressure in left side and spams,that come and go, that’s letting you know your intestine is tired and needs a break.
The recipes are so helpful, as is the support! I am feeling really emotional over this! Ibs sufferer 50 years!
Thank you for this advice. With one brother having spine surgery and one deathly ill and having dialysis, it’s no wonder I’m having a flare up. Had blood test today. Pain is in lower left pelvic area. So, having chicken broth, a few crackers and juice. I’m gluten intolerant and type 2 diabetic. So, I need the sugar.
Stress was the trigger this time and maybe the Pork Skins I ate. I’m going to boil som veggies and make a broth for tomorrow.
I have been suffering with this now for the last 10 months, I was in hospital for 2 weeks and not able to eat for 5 days with antibiotics fed into my veins. I have found so many conflicting information, it’s hard to know what to do for the best.
What I have found is I now drink at least 1 large carton of PEACH JUCIE every day (yeah Peach Juice) and since I have been my symptoms have really calmed down. I tried different fiber supplements and everything seems to make me worse, I came across this by pure chance but it seems to have done the trick for me and I can almost eat as normal. I am no longer in pain when I go to the bathroom, and I don’t get spasms or pains as often. My diet I try to stick to foods that are not fatty or greasy and stay away from drinks that have bubbles.
I think you just have to find what works for you, but it tricky and I have been in so much pain spending at least 1 hour on the toilet per day. I still have to go to the bathroom a lot but since the Peach Juice I am able to go and not be in pain.
This is a great website. I love the chicken and rice recipe, of sorts. I think I will try that. I guess I was thinking of diverticulitis as a condition and not as disease. I really need to focus on diet and overall health. I was surprised to read about the possible role that a vitamin D deficiency might contribute to this disease.
Me too! I was just told that my labs show low vitamin D!
Me too! I am always deficient in Vitamin D when I have blood work done. I will make sure I take a vitamin d everyday from now on.
All questions and answers were so helpful. Doctors do not explain and help enough. Terrible.
I was just diagnosed with Diverticulitis and UTI two weeks ago. I was discharged without any dietary instructions. I came home and did my own research b/c I was afraid to eat. I put myself on a low residue diet for a week and then each day introduced some type of regular food back in my diet. Homemade hummus one day, seemed fine. Cheese pizza slice and a soda, seemed ok. Next day I had a half of a quesadilla with chicken, cheese, black beans, pickled jalapeños nbut without the seeds and only 3. Later that night I was back in severe pain and at the doctors office first thing in the morning. Now I’m back on the antibiotics and left with very mixed messages on what is ok to eat. I’ve heard the Fodmap diet is good for IBS but there are foods on that list I question. I don’t want to suffer through flare ups that are so painful over and over again. On one hand we think the seeds from strawberries, raspberries, nuts and popcorn would get stuck in the pouches then you read it’s ok to have it. It doesn’t make sense to me.
After a Diverticulitis flare up you should not have anything spicy at all for several weeks.. Hummus can be bland but it also is a fiber..Cheese pizza?? not a good idea, nor are the quesadilla, jalapenos, seeds or not..they are too spicy and hard to digest..plus the skins on them may get stuck in your diverticulae.. I read after being on liquids to start out easy.. mashed potatoes, eggs, toast, macaroni, all things that are easy to digest should be consumed..I think that should be good for a week or more..but spicy foods should be avoided for quite some time..maybe forever if you find yourself in pain after eating them.. Your body will certainly tell you what’s hurting it with this disease.. This is my first flare up in 25 years.. Stress, and eating too much fresh corn on the cob (4 days in a row).. and some spicy foods did it.. I knew what was happening right away.. You never forget that pain!!! Good luck to all here.. Every day is an adventure.. 😉
The study they cite was done on 45,000 healthy people without diverticular disease. From that study they conclude what people WITH diverticular disease can eat. Makes no sense, They didn’t study people with diverticular disease so they can’t draw conclusions about us.
I suggest you eat no seeds or nuts, and do not overeat, you will learn to stop before you get full.
The doctors continue to interpret the study wrong, so they are of no help. You will learn what you can eat. When you eat a hamburger, make sure you order a seedless bun, I forgot 1 time and had a flare up . Stress is also a major factor for me.
The study followed 47,000+ men who had no diverticular disease *at the start of the study*. In fact, some of them *did* develop diverticular disease during the course of the study, and their data formed the basis of the findings. Those who didn’t develop diverticular disease became the control group by default. The focus of the study was what *causes* diverticula disease, so studying people who already had it wouldn’t be productive. The study followed these men for 18 years, and researchers sent supplemental questionnaires whenever any of them was diagnosed with diverticulosis or diverticulitis. This helped the researchers gather data on factors that may have contributed to their diverticular disease.
Hi, I just want to tell you a fairly new miraculous remedy that has kept me from getting a full-blown attack & having to go on antibiotics. It is a mixture of 1 Tbsp Bragg’s Apple Cider Vinegar & 1 Tbsp of raw honey mixed in a glass of water. Drink this at least 2x a day. I have also been taking the brand 1MD Complete Probiotics Platinum, DrTobias GutMeister PreforPro Ultimate Pre-biotic, Zenwise Labs Advanced Digestive Enzymes, and Digestive Freedom Plus by Patriot Health Alliance. These supplements are not cheap & even though I’m living on Social Security disability I sacrifice in order to be able to take them as they have proven themselves to be mighty in my goal to remain as free as I can from the painful episodes of full-blown attacks. As far as my diet I am still learning & figuring it all out. I know for sure that some things I just cannot risk eating. The fiber I added is Acacia Fiber as it is gentle & the psyllium fiber hurt me. I also drink a lot of Peppermint tea especially after meals & if I’m having spasms. My doctor prescribes a drug Bentyl 20 mg & this helps enormously! When having the spasms it relaxes the gut so this is very beneficial for me anyway. Though I will give first credits to the Raw, unfiltered Apple Cider Vinegar & the Raw honey! Truly blessed to find!
I was diagnosed with Diverticulitis the end of March. I was on Cipro an Flagyl three times. I am still having trouble eating anything even with taking a pill for nausea. Nothing wants to stay down. I am drinking keifer and Boost. At this point I don’t even want to try to eat.
Hi Lori,
My last bout with D (Nov 17) and taking the Cipro and Flagyl left me feeling nauseated and vomiting. As soon as I could get off the clear liquid diet, I started taking my antibiotics with 2% milk and using the under-the-tongue anti-nausea pill every 8 hours or so. It really helped. I then could start eating white bread, cheese, chicken, and turkey as well as other easy to digest foods. I am now ready to start introducing more foods into my diet. I hope you find something that helps.
I was diagnosed with this disease 4 Years ago…and, I just had a flare up a week ago..I try and stay clear of popcorn,and, anything with seeds,,and, Yes, they DO cause a flare up,as, in my case here…and, here I sit taking antibiotics,and, still having issues…YES, there are certain things I CAN’T eat…but, SOME times I eat the heck out of them…I fins, Pizza,Nuts. Popcorn..are the main culprits for me…and, last week it was tortilla chips and salsa..UGH….this disease is Horrible,and, HURTS tremendously…
rd with severe stomach pain–dx was DV. Thanks for being here! So i have had liquid diet – bone broths and well-cooked veggie or chicken soup. Sun night, i added chicken that had been soaked in Nepalese herbs from local Nepali restaurant. Ayurvedic doc says to eat ghee in my soups and 1/2 tsp dried ginger with warm water after meals. My liquid poop is beginning to become liquid mush – looking forward to being more like cow-pies (yep, as in a field of cows). 1) i am under stress, 2) in 2 days,I meet my boyfriend in Lisbon for a 12-day fun (can be slow-paced) trip (16 hour flight-I live in SFBay area, CA) – So should I go on trip or stay here and continue to add to my diet. And, what to add next to diet? and when to add…had/have a v healthy diet and lifestyle. ,
I just got out of the hospital after 5 days of being in there. I am totally terrified to eat anything. As I’ve seen stated the doctors really don’t give you any kind of guidance on food. I have read such conflicting information that I really don’t know what to do. I’ve never really been so scared in my life. I had antibiotics intravenously UTI and I’m still on antibiotics for another 10 days. I’m confused and scared and don’t even know what to introduce back into my diet. I’ve never taking pills or medication before I’ve been so healthy up until this point. I’m trying to find somewhere where there’s some kind of diet for me to be on but again everything is so conflicting
I feel the same way. I just got out of the hospital on Monday I was in there for 4 days. It was the crazy pain I ever felt. I went in and did a CT scan and they said hey you have diverticulitis and a perforation. (I am also diabetic) I was given a crazy amount of antibiotics and for three days I had only ice chips. The day I was released I was in a liquid diet. i did that for two days. I am now moving on to baby food consistency type food. But this whole thing is scary. I just changed my eating habits a little over a year ago I became vegan. So I had plenty of fiber and water is the only thing I drink. So I so confused how this happened or when to even eat normally again. I don’t want to go back to the ER. I am still on antibiotics for another 10days. I also found everything is very contradictory on what to do and what not to do. Flare ups can be prevented…flare ups will happen inevitably. So confusing.
Jacki, Hi this is Patricia. Have you heard of or tried the Apple Cider Vinegar that is raw and unfiltered thus fermented? Mixing 1 or 2 TBSP of this with same amount of Raw Honey in a glass of water. This has very strong Antibiotic properties and has helped me avoid going into a full-fledge attack and antibiotics! Try, if you can. Much Love to you
Also Jacki, I have been trying Bone Broth and it has been very nourishing when in an almost-attack and also during an attack. Bone Broth is so good for us! We can make our own, though it is even in grocery stores now. Blessings
Thanks for all the useful info. Just wanted to share my experience. I normally have flare ups when I eat Chicken or raw coconut. I’ve been having psyllium husk powder but not sure if it’s helping.
I have appreciated the above questions and comments, this is my second time with it and I am on the liquid diet for a few days. It does seem a bit overwhelming, but my understanding from reading is that you move from: liquid diet, to soft, low fiber cooked fruits/veg foods for 4-6 weeks, to a higher fiber with raw fruit/veg. Including exercise/movement more through the day depending on your job. Would this be correct/true from your readings?
Hi.. This is my first experience with DV. And yes, my doctor only to,d me to use Metamucil.
So my first meal was Meatloaf, carrots, and mashed potatoes…. hmm. Wrong.
Finally did research online and settled with the Mayo Clinic information that made more sense. Started on liquids, added a few wrong things, but went to BRAT – Bananas, Rice, Applesause,dry Toast next..
Adding scrambled eggs now. Went to IHOP with the grandkids and ate 1/2 waffle with NOTHIznG on it. (In the old days it would have been swimming in syrup!). Bad.
Starting to add canned fruits and veggies this week, and will have some chicken . I will pretty much follow the Mayo diet until it’s been 6 weeks from the flare-up and will start a gradual transition to higher fiber foods. My sister also has DV and eats okay — but when she eats stuff she should not ( peanuts/strawberries) she winds up in the ER. Soo not worth it.
Seriously working on stress level. All my family are high stress people genetically, so will learn to meditate at some point. A good church family is also calming and nurturing. Good luck on your journey.
I’ve had 4 attacks in the last three months. I read and believe now that food combining is extremely important. Two of the attacks were after 3 days of fasting when the only thing I had was almond butter (a protein) and apples. I thought it was the nuts, now I know it was the combination. The last attack was adding blackberries to keto pancakes (coconut flour, eggs, cream cheese). In food combining no starches with anything but water veggies, and fruit by itself. I had been on a ketogenic diet (high fat, moderate to low protein, low carb) for a month and all of my belly symptoms completely disappeared, and quickly! Then I had one off day with the blackberries and protein pancakes followed a few hours later with popcorn and boom. Again, two instances of poor food combining as you should not eat starch (corn) so soon after eating protein. Also, food combining should in a ration of 9:1. Carbohydrates to Protein or Protein to Carb, depending on if it is more of a carb or protein meal. I’m convinced that Nutritional Ketosis plus careful food combining on the days I have the occasional starches will do the trick. I will report back in a few months. p.s. I add psysillium daily to make sure it is a high fiber diet. Dr. Mercola has a great book on this “Fat for Fuel.”
Check out the Simple Mayo Clinic diet online.
I am very aware of the quality of foods in this country re spraying with chemicals. I also follow Dr. Mercola too. I plan to try to buy only organic fruits and veggies when Inget tomthat part of the diet.
I’m relative free from problems so far following MayomClinic… in addition I’m planning on Haiti g out hospital GI Department until they add a recommended Diet Paper to their release patient information for DV patients.
You are leading people wrong about seeds and nuts in relation to diverticulitis. Every single time I eat either one of those, I get rectal bleeding and a stomachache for two days. Get your facts straight!!!!!
Hi, this is Patricia. In my experience with this disease almost everyone reacts differently to diet, etc. So, some people actually can still eat nuts, salads, effervescent drinks~ though I certainly cannot. This blog and other research has helped me immensely though our bodies change all the time, especially as we age.
I’m glad to know I’m not the only newly diagnosed person who is confused. I like research, but it sounds like those who have lived with diverticulitis flares have many different triggers. It seems so individual, and I think I was looking for a black and white answer. The idea of “trial and error” and the risk of another flare is certainly intimidating. Thank you for your posts and sharing of tips. It’s great to know I’m not alone.
My husband had his first ever flare up of DV at the end of April and ended up with emergency surgery as soon as the ER doctor took a CT scan. He was in the hospital 2 weeks after partial sigmoid colon removal. It is all so confusing because every nurse says to eat a different way!! So far we have seen that fiber from milk of magnesia is much better than from any other fiber. I will not even let him near seeds or nuts right now! He is having a weird pain right now that I don’t know is a flare up or a muscular pain (he said it feels like a back ache, at first and has been laying down too much, so it could be) but in his lower left side, so who knows). He has a doctor visit tomorrow so we shall see if they know what is going on. I am so glad to be able to read what everyone is posting here. Medically helpful and just nice to not feel so alone. I think everyone seems to have a different poison.
OMG this is exactly what I am feeling. My first attack and I am miserable. I’m trying to work but can’t stay focused. Just went on antibiotics and a clear diet (my first day). Thank you for writing as it is helpful to know that I am not alone.
I had been diagnosed with diverticulosis four years ago after going to the emergency room with a high fever and severe abdominal pain. I was given antibiotics intravenously. The gastro doctor suggested, after the clear liquid diet for at least three days, to drink Citrucel every day along with regular diet. After an average of three to four diverticulitis attacks a year I have found what works for me. I take probiotics, Greek yogurt, drink plenty of water and avoid all nuts and anything with seeds. If I don’t have a bowel movement in two days I take Miralax. Also, I eliminated the fiber drink. I have not had an attack in 18 months. My family doctor had told me that all of her patients that have diverticulosis always have flare ups after eating seeds and nuts. Again, this is what has worked for me and everyone is different. Best of luck to everyone that suffers with this disease.
With Diverticulitis,doctors put me on a liquid diet for now,can I have Ice Cream?
On here it says high fiber diet good yet when I goog led what not to eat for Diverticuosis it says avoid brocolli,cabbage,corn,beans,dairy,chese,fatty foods.I always notice beans bother me a lot.
Hi, this is Patricia. I was told that beans are very hard to digest so I rarely eat them. Broccoli and any vegetables really need to be cooked until pretty tender. I cannot eat anything with nuts or any vegetables or fruits with skins. Still learning…it is very individualized! Everyone is different with different triggers. See my post way above that I tell what has helped me immensely. Blessings
See my May 21st post!
My husband has been having issues with his bowel movements for a few months; either constipated or diarrhea. Finally got him to the ER and he was diagnosed with Diverticulitis about 10 days ago. No one mentioned a clear liquid diet to us, so it took me a while to catch on. He is now trying soft foods; eggs, white bread, mashed potatoes and chicken (poached).
He continues to have multiple bowel movements in a 24 hour period, but no pain. I’m concerned there may be something more going on that didn’t show up in the CT. I’d appreciate any help you may have to offer.
Hello all,
Just diagnosed with diverticulitis; good information here. A lot to learn
I had my first experience with a flare up in December last year. Horrible, but my doctor was great. I am now lactose intolerant, and am still finding out what foods hurt my stomach. I have been sick all week, but don’t know what could have set it off. The only thing I can think of was a piece of cherry pie….maybe the skin on the cherries? Doing the BRAT diet fir now
See my May 21st post! Blessings and add Bone Broth! Very helpful to me.
Just got diagnosed, on antibiotics and liquid diet, has anyone seen a nutritionist to get a good diet plan?
Diagnosed last night at 9:00 pm in the ER. (I’ve had problems for over 3 years but refused to go to a doctor until this last flare up.) They prescribed two antibiotics, pain meds (which I won’t take), and something for nausea that may be caused from an antibiotic. No one mentioned a liquid diet! I did get some prunes and fiber mix to start today. Now I’m worried about what I should eat! I am a picky eater (not a fan of most veggies – except green beans, potatoes, and may favorite … corn, which I am reading is a big no, no!). I’ve read (and heard from friends) no legumes, seeds, or nuts. It’s Fall, I live in the South…can I have boiled peanuts?
I have so many questions about what I can/can’t eat. I’ve heard a lot of different thoughts and I see that this is very individualized. I enjoy reading all the posts. This site is the most helpful I’ve found.
Hi there, I live in the South, love boiled peanuts but my last diverticulitis attack was after eating over several days some boiled peanuts. Had painful cramping and painful BM, followed by chills and fever, no more boiled peanuts for me!,!, Having to eat small amounts of food, chew more thoroughly!! Slippery elm tea helps, also trying more probiotic food. This is awful disease, Wishing you the best!! JJ
I am so grateful for everyone’s input! I was feeling very alone and very frustrated, and know I feel like we can all get through this together. I don’t have any answers yet, I am a few days out of the hospital and trying to get it all right. I am off to eat a bit of tuna. Good luck you all!I am so grateful for everyone’s input!
I came across this site while searching for a proper diet for this condition….I went to my doctor last week because I was and still am having left side pain that started over a year ago but he gave me a one dose prescription for it….it was a powder prescription with half cup of water…never had it b4 …doc is sending me to specialist but appointment is not until January 🙁 I’m suffering with pain everyday divercultists is what he suspects I am a believer in natural healing and I need to do this again….I hope to find something I done natural healing before for a cyst in my liver and it works I read the comments and I’m glad I found this thx
Hi – wondering how on earth the post above is September 10th? Maybe you live on a different continent. Anyhow, my diverticulitis comes on from a combination of dehydration (we’ve had a two month heat wave here), stress and possibly eating beans – that is to say, not green beans. Stress is one of the biggest things for me. The funny thing is, each time I have an attack (have had many – probably about ten or a dozen – in the last 10 or 15 years)….it seems hard for me to realize what’s going on – fever, chills, gut pain. Then after the fact I realize “it” is back again.
OK – the date thing is wrong on this page – it’s only September 9th!! Unless we have entered the twilight zone which is absolutely possible considering the horrific events happening on the planet at the moment 😉
Australia is almost 24 hours ahead of the US, welcome to the twilight zone!
Suffering from the big D.. Thanks for all the input. This disease is making me miserable and looking for ways to cope. God bless?
Thanks for the comment Connie. Good luck!
I have had Diverticulitis for over 8 yrs with many flare up’s I started juicing all my veggies in a juicer that separates the bulb from the juice. Since then I have had one flare up but nothing like the ones I had had before. They were shorter and not so painful. I got this off the Mayo Clinic’s website for Diverticulitis. I try to get all organic, but I juice a carrot, part of cucumber, kale, spinach, part of ginger root, celery stalk, and red cabbage. I find this to help when I feel a little pain going on but not really a flare up. I do this every morning and it has helped me in so many way. Not only is all those things very good for the tummy it is very healthy also. I stay away from brown, wide rice, I rarely do bread, never any nuts or fruit with seeds and no veggies with skin unless a steam them pretty soft. If I am in the mood for apple I peeled it and add to my juicing. I do a lot of white meat but I also eat red meat in moderation. I only use ground turkey if my recipe calls for hamburger . I have read all these comments and also find it helpful. I wish you all well and continue to support to a better living with Diverticulitis
I had a diverticulitis attack about 9 years ago that was “cured” with a round of antibiotics. I’ve always had digestive issues – don’t remember a meal that didn’t have some sort of symptom following it. I was then diagnosed with IBS a few months ago and now I’ve had another DV attack and am back on antibiotics with a CT scan to follow. My Dr. Said the FODMAP diet wasn’t scientific (?!) and just told me to eat high fibre as it was good for both IBS and DV. I, too, am confused about what to eat. There was no mention of clear fluids to start. I look like I’m 9 months pregnant (I’m 56 for gawdsake) and don’t even want to go out in public. Trying to keep my spirits up, but feeling a little discouraged. Glad I found this site and thank you all for your wisdom.
Thanks for the feedback Cassi and good luck with everything! 🙂
Cassi if antibiotics helped your Diverticulitis attack maybe H Pylori is part of the issues (causes ulcers and is cured with specific antibiotics), so ask your doc about a blood test for it to see if that might be contributing to your issues.
July 21 of this year I went to the add with symptoms of constipation, tender abdomen, and flu like symptoms (anyone recognize this). I actually only went to the Dr for a flu test, if not for those symptoms I’d have just gone home from work and slept it off.
The Dr assumed diverticulitis and ordered antibiotics and a CT scan, confirmed. I was referred to a surgeon since 2 abscesses were also found on 2 of the diverticula. He ordered an additional week of antibiotics and another CT scan to see if the antibiotics were working, things got worse and 1 abscess got bigger…
Fast forward to today, as of typing this I have lost 35 Lbs by being off and on a clear liquid diet for 2 months (only about 2 weeks worth of low fiber food in between). I had a colon resection surgery and wound up in the hospital for 2 weeks post surgery.
I am currently researching how to properly and gradually add back “regular” foods that I ate prior to my surprise diagnosis. I used to eat a diet rich in dark leafy greens, roasted and grilled veggies, high in protein and about 3/4 gallon of water a day. I used to hit the gym at least 3 times a week and thought Imwas pretty healthy, until…
Any tips others may have are helpful, this is very new to me and I am really not used to being so tired and weak as I am,post-op.
Hi Christopher. Sorry to hear about your health issues. I would suggest eating a high fiber diet. I will soon be adding a sample meal plan for diverticulitis sufferers on to this article so keep an eye out. 🙂
This is the most useful site I have come across. This disorder takes many forms and seems specific to the individual. There is a lot of confusing and contradictory information available on the web. Yes, it has been a frightening journey, with my body fighting the foods I was eating. I pared my diet down to the basics; boiled eggs, boiled chicken, fish, cooked vegs… for about 3 weeks. As I am growing stronger and feeling better, I am adding in very small amounts of “experimental ” foods like very lean beef, last night. I could tell a difference and a twinge of spasming today, but it subsided. So, very small amounts of this can be added occasionally. I’m going to try a few peanuts next. I still am on the no lactose milk for my morning coffee, and did not react well to a 0 fat yoghurt or probiotic chewies. I haven’t found a no lactose yoghurt yet, but would be willing to try it. Basically, this is a lifestyle altering disorder. You must be sensitive to your body’s needs and specificities. I will do anything necessary to avoid having that debilitating pain again.
Hi Ellen. Sorry to hear about your health issues. Good luck with your trial and error!
Fantastic site, just stumbled across the site and really took to heart how prevalent this has become (figure social media and such sites just bring greater awareness). I have not had a flare up for about 2 years but at least a dozen events in the last 20 years. It started Tuesday (today is Friday) previously my Dr. gave me some antibiotics as emergency kit in case I feel one coming on. Started the process and jumped on clear liquids. In this event it did not help, so off to CT scan and will get a follow up scan in 4 days. 2 shots and continuation of antibiotics. . How did this happen to me again? I have come to the conclusion that wearing a belt pulled tight does not help, each event I had worn a belt. Now I wear suspenders and no issue. Lost 20 lbs I thought, hey switch to a belt, so 2 weeks ago but that belt on and bam it is back. Just saying there may be a coloration of tightness around the mid section, at least for some.
Thanks Stephen for mentoring about your belt and tight ness = your flare ups…
I have a lab band and was just diagnosed yesterday with DV at the er after a week of fever ,chills and extreme gut pain …
Going to explore more if the band is an issue-because I do get that tightness and pain and before my diagnosis thought it was an issue with my lap band which it isn’t !
This site and dialogue is wonderful,so informative.
A lot to absorb (ha) right now ..
I am also part of that genetic link ..maternal grandmother and mother both had/have DV tas well .
Too self healing!
Cheers
Helene
I was diagnosed with severe diverticulitis July 2016.. went to ER with bloody diarrhea. Cat scan, colonoscopy and blood transfusion.. it was horrible.. now had flare up again and was
Hospitalized for it.
I’m just out of hospital today with flare up from diverticulitis. Went to Dr with pain for 10 days didn’t know what it was. She said you need to be in hospital and fluids, antibiotic and pain meds.. I just noticed this site while doing reaserch on this disease.. I’m so glad I’m not alone.. thank you
Hi Kathy, I’m sorry about your health issues, I hope you get better soon. 🙂
Hi everyone I have added a sample meal plan for diverticulitis in the article. Let me know if you have feedback 🙂
Hi Joe where can I find your sample meal plan, new to this and not sure where to look? Just returning to hi-fibre after first attack and need some inspirational recipes – Thanks 🙂
Hi Kate, I have recently added a sample meal plan to this article that you commented on. Please let me know if you do not see it. Thanks 🙂
HI Kate, https://www.dietvsdisease.org/diverticulitis-diet/#Diet_Plan_Menu_For_Diverticulitis_and_Diverticulosis
Hi, can you recommend a cookbook that I can get in paper version?
Have had dv for at least 5 years, I had inflammation for the 1st time 4 weeks ago. Given loads of antibiotics, been getting even worse wind then normal. Eventually had 3 days in hospital on iv drips, antibiotics intravenously pain killers. I find I have diahroea about once a week then get bound up and don’t pass a motion for about 5 day’s end up in agony and have to use a suppository or an enema. I had diahroea after the scan (for which I had to take something to loosen me but it only worked later. Consequently empty bowel 6 days then total impaction. Used enema and 2 days later starting to get uncomfortable again.Scan showed Dv but nothing else sinister am waiting to have colonoscopy when ever everything settles down. Just don’t know how to cope other than stop eating.
Is black coffee ok when flare up calms down?
Hi micki, Yes should be fine 🙂
Hello all ,
I read every response in this blog .
I am 50 years old 5’7″ and weighs 155lb , living a very healthy lifestyle , eating a middle eastern diet in general , drinking lots of water with lemon , no soda or junk food alcohol once a week if any , working out 5-6 days a week .
I have had some stomach aches for the past month , minor ,or so I thought , treated with gas relief tablets that worked sporadically .
Last Tuesday the 16th I had my first major pain with fever and chills , took some pain meds and went to bed , the next day the 17th I felt something was wrong , I checked myself into the ER at 5:30 pm , at 1 am on the 18th I was on the operating table for a severe diverticulitis with a perforation , Doc said I was lucky to come in when I did .
After 7 days at the hospital I am now home thinking what could I have done to prevent this , 50 is not the new 40 , get you colonoscopy early do not wait .
Now experiencing the food dilemma as you all , I am eating white rice, mashed potatoes , pasta with a touch of olive oil and parmesan cheese , toast with cream cheese , chicken soup , eggs(all varieties) , cukes ,skinned raw tomato , bananas, avocado , saltines , all natural peanut butter , lot’s of water , camomile tea , juices .
Doc said about 6 weeks to recovery .
I have had intestinal issues since childhood. I am a 60 yo healthy woman with moderate exercise. About 4 years ago I was hospitalized with severe stomach pain and, once released after colonoscopy, again diagnosis inconclusive. I have always had the pain (gurgles) in my lower left abdomen though. Fast forward to Sunday Oct 22nd after Church at Walmart – doubled over in pain. Thought it was my normal “once I go to the bathroom I will be fine” pain. NOT! Low grade fever, went straight to bed although I have experienced much worse pain in the past. The difference was this pain was continuous. Worked Monday and Tuesday through the pain and went to Dr Tuesday evening – blood tests, urinalysis. Dr called Thursday (office closed Wednesday) said I had elevated liver enzymes and white blood cell count – sent to CT Scan Friday – Friday afternoon Dr calls with “Diverticulitis” diagnosis and puts be on Cipro and Metronidazole. The Metronidazole after the 6th pill made me extremely sick. I told Dr that I could not take that anymore and would continue on Cipro. She said Cipro alone, after completion, may cause DV to come back with a full blown attack. I am pretty much surviving on toast, chicken broth with white rice, some yogurt. Is this true? Has anyone else just taken Cipro and recovered? I, too, like many of you are afraid of what to eat next that may send me to an attack. My grandfather had 28″ of intestine removed and my aunt suffers daily because of DV. Any help would be appreciated.
I took cipro and Pflagyl I was so sick I could not walk my eyesight was bad my stomach was sick and dizzy headed all I could do was lay around that pflagyl is some bad stuff took it for 10 days. I will never take that again as it was worse than the pain. I knew i had it 25 years ago but, never had any trouble till now. I have cut out so many foods, the dr. that done my colonoscopy said eat what you want it is a myth and never been proven that foods cause it. Prior to my attack I was taking an anti inflammatory med. and aleve. I think that was my culprit, When I googled meds, they were the first on the list.
I’ve had diverticulitis since 1985. I’m 63 and when I was 48, my doc said… It’s time for surgery. I had been on antibiotics every other month for a year or so. I said no thanks to the surgery, realizing the roller coaster I was on might have been due to the antibiotics. I asked a friend with natural medicine knowledge what to do. Aloe Vera juice (inner leaf without latex), fiber supplement (when not having an attack) and a diet full of fruits and vegetables. After all these years I can still have a flare up but if I start the aloe vera juice, 2 oz. four times a day, olive leaf supplements (antibiotic properties), 2 capsules twice a day, and slippery elm supplements, 2 capsules three times a day…. along with bone broth and maybe non grainy toast, I get over it in 24 hours. The antibiotic routine would leave me with high fever and severe pain and take two weeks to recover. In my case I’m suspicious of combining too many things like blackberry seeds, white flour, alcohol, maybe popcorn, and stress, too close together. I’m recovering from a twenty four hour episode now, fever gone and considering taking a small glass of aloe vera juice every day for a few months…. to see if I can prevent it from coming back. I was surprised no one had mentioned drinking it on this website. The tricky thing is recognizing the subtle symptoms when they first come on… more bowel movements, more gas, a momentary twinge of pain….. Don’t ignore!!!
Katy, when you start feeling an attack coming on, what do you do first? Yesterday I started feeling twinges, but everyone at work is getting a stomach bug. Last night I had pretty sever pain and I gave in and started ciprofloxacin. This A.m. I’m feeling better. Going to stay on liquids for a few days. I really don’t know what gets DV started. Could it be the roasted almonds I had for dinner last Friday? Was it that I let myself get too hungry, then ate too fast? Do you think ciprofloxacin alone will cause a relapse? Without flagyl. I’ve never heard of that. Someone put that in a a post. I’m getting aloe juice and slippery elm today. Seems like I have relapses about once a year, probably 5 in the last 5-6 years. One minute your fine and the next your bent over in pain. You do have to stay vigilant.
Thanks for the reminder Katy. Best of luck.
I forgot to mention that aloe vera juice isn’t hard to find.. usually. It’s in health food sections of grocery stores and even pharmacies. The supplements I mentioned are also in grocery stores and pharmacies.
i’m 48 female and previously healthy. I had mild dv diagnosed incidentally after colonoscopy two years ago as a result of ongoing IBS symptoms. no flare ups until Easter when i was admitted to a&E with acute left side pain, chills no fever and crazy fatigue that had led up to it. Prior to this I had been fit , energetic and mostly vegetarian since the start of the year! After IV antibiotics, liquid only and painkillers i returned home. CT scan showed huge infection and diverticuitis. was exhausted for over 3 weeks, following low fibre diet. moved to extra high fibre diet, added daily fibre supplement, bioglan probiotics, within a month same symptoms returned and GP prescribed cocodamol and 2 antiobiotics. after 10 days feeling dreadful gradually increased the fibre again. relief for a few weeks then repeated pattern almost every 5-6 weeks until now November! Antiobiotics make me feel terrible- foggy and cant drive! I worry abou the long term effects on my body now i’m on 5th lot since april. i get thrush every time too. Have added vit d, vit b3, a step for under my feet on the loo, seen useless dietician, drinking lots of water. hill walking whenever i can, having mostly normal daily bowel movements but pain is reluctant to leave and can keep me awake if sidelying at night. Am waiting to see colorectal consultant but NHS time is 6 months. I don’t want surgery but can’t keep on like this! I cant travel abroad, work and family life is affected. Honestly wondering if the high fibre diet is the problem? I was fine before i became veggie! Is there anything else I can try?
Hi Ella, for some people high fiber can make things worse. They’re the minority but it’s something that’s well known in the scientific community. You may want to try slowly lowering the fiber intake and seeing if that helps. Have you been tested for coeliac disease?
i’d like to add that this site is the most informative i’ve found, thankyou! There’s so much fiction out there. i’ve also just found this from the NHS’s National institutue of clinical evidence (NICE) which seems to suggest the evidence for fibre is …lacking…!
https://bnf.nice.org.uk/treatment-summary/diverticular-disease-and-diverticulitis.html
A no fiber diet is ideal for managing this condition. I don’t care what any study says. They recommend a low fiber diet during a flare up (duh) because fiber is the one thing our bodies can’t break down. Why discontinue a diet that helps to get rid of the symptoms? Fiber has to be shit out. What in the hell do you think is stuck in your colon in the first place? It’s common sense to remove the one thing that can get trapped inside of you: fiber. Eat some steaks cooked rare as hell and go enjoy life again. If you want some carbs eat white rice or some really ripe bananas. Throw away most of the plant food and never ever take fiber supplements. You know it is making your symptoms worse, so why do you take them?
Fiber doesn’t get trapped inside of you. On the contrary, it helps to speedily transport waste out of the body. The diverticulitis is caused by other factors and once inflamed need to heal thus the low fiber diet. But of course this is just what I think based on scientific evidence. Maybe you have scientific studies which give a contrary view. I’d be willing to hear.
Vegetarian, high fiber diet for 25 years. Last year my colon burst after terrible constipation, 12 days in hospital, 7″ of colon removed, needed 9 liters of saline to clean the fiber/feces out of my. My diet is always high fiber including fiber supplements but I was always constipated. Still suffering. Thinking low fodmap or maybe what the guy above says is true about fiber. I almost died, had a ileostomy bag for 2 months and was oio of work for 3. 49 years old, otherwise healthy. Maybe the answer is pasture raised meat and fermented vegetables. I don’t know. My high fiber diet keeps getting me constipated, which almost killed me…
What a lovely site…..I am struggling with this illness now for almost 6 years….I cant eat nuts, seeds, cheese, some vegetables and fruits…if I eat these things mentioned above I ezperience extreme pain in my abdomen and left side of my body. I had an operation in 2011 where 11 cm of my colon was removed, the operation made it worse, because now my stomach does not go out on its own, i need to drink Agiolex to help me go to the tpiler. This is bad.
I was just recently diagnosed with diverticulitis. I have one more day of my two antibiotics (7 day course) and have moved up from clear liquid to a more BRAT like diet (per my dr). I’m trying to find good information on what I can successfully start adding back, as I feel like I’m “starving” myself of good nutrients.
Hi Chery, that’s one thing that I have a hard time with too, I get so hungry towards the end of the meds. My doc told that when I started feeling better to start adding soft low fiber foods back to the diet and to keep the meals small, like the size of 1/2 sandwich. Mashed potatoes, scrambled eggs, white bread, boiled chicken, this what worked for me, after being so hungry I found these plain foods to be so scrumptious but after a few bites I would feel full so I would save it for later and eat small meals.
I know the opinions out there are so different but this is what works for me
I’m not alone! Somewhat comforting knowing others suffer with this and hearing new ideas on how to cope. Had my first bout 11 years ago, then another last year and 2 within the last 2 months. Most of the doctors just treat the symptoms and then your on your own. I ‘ve received more info reading this blog than what doctors have ever told me. The last bout I’m trying to cure on my own without a doctors help….so far so good. Thanks.
I agree Tom, nice to know we are not alone. I didn’t know anyone with this so I went to researching right away especially now after 2nd attack so soon. I will say I thought I was going to do the same thing this time around, just handle it myself. The pain got too much and I went to the doc and this time was told not to mess around with the pain because the last thing you want is one of these things to rupture and then you end up with emergency surgery possibly. So be careful
Hi Tom, glad I could be of help – good luck with your condition! 🙂
Best of luck Tom. I believe that is the way to go. We are ulitmately responsible for coping with our diseases. Doctors can sometimes provide info, relief. But generaly we have to make the decisions on who and how to treat ourselves. It’s a journey but hopefully a productive one. Whoops just read Debby below and was reminded of my mother’s emergency surgery on her colon 25 years ago. When one is in pain, get to a doctor.
For the pain I take 2 extra strength Tylenol, which has always been a great pain relief med for me, but I’m wondering if anyone uses an anti inflammatory with any success?
I was diagnosed with D in Feb 17 and just has my second attack 8 months later. I thought I was doing good with fiber intake but now not so sure. Its so confusing, one doc tells me this and another doc tells me that and all the reading online is conflicting of what to avoid and what to eat. So I’m going to pay closer attention to my diet and see if that makes a difference because as you all know, it takes a while to recover and I cannot afford to be down so long this often. Ive been looking for a cookbook, paper format, so I can make notes. Can anyone recommend a good cookbook? I’m hoping to find one that will include fiber amounts in the recipe so I can keep track of my intake for a while until I get used to it.
Thanks in advance
Hi
I have had DV for twenty years, been hospitalised twice in last 6 months , unfortunately it does not get better in time, from experience I have found that peanuts , whole corn, popcorn and raisins have caused me grief, also being too loose will be a problem, think of your bowel as a tube of toothpaste, if it’s nearly empty you have to squeeze it harder to get anything out. Its a balancing act, the over use of antibiotics if you don’t have infection is bad and makes longer recovery time I feel.. surgery is my next option , but I’ve had so long to think about it I’m up for it. Good luck all
I’m currently suffering from Diverticular flare up. Abdominal pain, constipation, severe wind then often diarrhoea. Have tried so many diets and different supplements over the years but just don’t know what to eat anymore. I also have coeliac disease for past 30 years. Constant bloating and look 6 months pregnant. So fed up with it all. This site is good but still so much conflicting advice..Help please.
Have many people considered or had surgery and if so has it been beneficial.?
Hi Marilyn. two of my friends have had the surgery for this awful condition, which I’m also suffering from, they are both so pleased that they had it and have never looked back. l would definitely try anything that could give me a better quality of life.
Something that might help: l stopped taking Aloe Vera juice over a year ago which did help a lot, l suppose l thought l was ok without it (not a good idea) so I’m going to start taking it again. l took 15ml about half an hour before each meal and as l remember it kept it under control.
I’m on my eighth attack in about three years. I can’t figure out any specific triggers. For treatment, I have taken the Cipro/Flagyl regimen the first four attacks. Since then I have used a combination of oregano oil, peppermint, and probiotics, twice a day, with the same success as the antibiotics, without all the awful side effects. I know this sounds hokey, but is being proven for me again as I am making good progress in symptom relief after three days (along with liquid diet). This was my most painful attack so far, but has still responded to this treatment. I can’t afford a cat scan every few months! If the symptoms ever do get worse when I’m treating this, of course I’ll go to the hospital. But at this time with now significant experience, I’m sticking with this!
Thanks for the tip!
I have just experienced my third flare up in three years and I am baffled and a little scared. In the past two years, I have added a great deal of fiber to my diet through morning kale/spinach/salad and almond/soy milk smoothies, i have increased my exercise, and still experienced a debilitating flare up.
Here I am, I reverted back to the internet for more advice. I am heavy, I need to lose at least thirty pounds, that I know, but I am beginning to think it isn’t just what you eat but how you eat it. I am reading more about eating several small meals slowly that include key nutritional elements, increasing the intake of water to avoid constipation, and being careful not to eat too much food in one sitting.
I am also reading about stress and the ways it can also add to the mix. My mother was diagnosed with it in her 40s and when I was diagnosed, I realized genetics are a part of it. But my sisters do not have it, both have active jobs and are on their feet much of the day. I am an office worker and sedentary more than they are, so although we were all more than likely predisposed, I believe my low exercise also contributed to the disease.
This week I have started a Food and Exercise diary. Although I have aimed for 3 hours of exercise each day, it is not enough. I realize that I need to specifically track my cardio and pay attention to how much cardio exercise I get each day. I need to eat the probiotics every day. i need to keep my diet in check and get my weight down. Tracking it may be the only way to keep myself accountable. Thanks for the article and the comments, I think these forums are very helpful to learn what causes the disease and how to properly manage it. Doctors can only do so much, people with the disease need to advocate and focus on what works for their individual body needs.
Thanks for your comment Heather and good luck on your journey!
I’m 52 years old and had my 2nd DV episode just before Christmas. The 1st was 9 months ago, and was mild enough to be handled with antibiotics. The 2nd more severe, 4 days in hospital and I’m now recovering (with a few setbacks). We’re talking about surgery partly due to my family history. My mother, and 3 sisters all had DV that eventually required surgery. Does anyone else have this hereditary link?
Also, my colonoscopy showed that I have diverticula along the full length of my colon, which the doc said was unusual. Anyone else have this too?
PS – this site is great and I appreciate everyone sharing their experience
Yes Sue me too! I’m 52 and have had several bouts with two hospital stays. My mother had this and her brother as well. Mom had the surgery removing two feet of colon. I have the diverticulosis through much of my colon.
Hi,my husband is on his second round of antibiotics in a month,suffering badly on this flare up,so much conflicting advice on fibre that he really does not know what he can and can’t eat,he’s on clear fluids at the moment but has to go back to work in the next couple of days,what can he eat to keep his sugar levels right?,he has a very stressful job which includes lots of driving so needs to have good concentration ,thanks karen
Check out this diet advice. https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/diverticulitis-diet/art-20048499
I too am coming off an attack a few days ago. I’ve had it for 6 years now. When I have an attack I try and not eat anything for the first day following, just drink tea and water. Next day I get some gatorade, I find it keeps my energy up and feels less acidic than fruit juice. It’s a feel thing, as to when to add more foods. I start with soups, smoothies, pudding and the whitest white bread you can find, food with almost no fibre. Then as days go on add more fibre-y foods. I supplement with psyllium husks, just dump a heaping tablespoon in a glass of water 2X a day, gross at first but you get used to it. Good Luck
I’ve just been to see consultant as my diverticulitis happens every 4 -6 weeks now I’ll be have scan and stuff again but he said I should look at fod map but I’m not sure I can tolerate half of that food as every think I eat flares my bowel especially in a attack is rather not eat but it’s really hard when your hungry ? any ideas ?
Hi Karen,, please see a dietitian for personalised advice. Sorry I can’t help more.
I put my diverticulitis in remission with a ketogenic diet. It was that simple for me. I love the ketogenic diet. People that don’t adapt to living in ketosis fail to get enough electrolytes, especially salt because of the dogma around the phony war on salt (really bad science from the 1950’s). I supplement with 1 teaspoon of salt every day plus 3 times the US RDA of magnesium. I also take a zinc and potassium just a few times a week.
I am now 6 years symptom-free with three minor “exception” episodes: when I attempted to reintroduce either white-colored dairy food or gluten grains minor symptoms returned. I was able to resolve each one with a 4-day water & coconut oil fast. BTW: I am fine with cheese.
Maybe a high fiber diet would have prevented diverticulitis in the fist place but after it has developed I think that high fiber diet just makes it worse.
For those that have to be on liquids I found a broth to make when flare ups exist that is simple to make and full of nutrients!
https://www.onegreenplanet.org/vegan-recipe/no-bone-broth/
My wife is hospitalised and is very poorly. Unfortunately a colonoscopy punctured her bowel to add to the diverticulitis, something I understand should not have been done.
As a vegetarian, she automatically has had a high fibre diet. She consumes high amounts of pulses including lentils and chickpeas (which supposedly are not good), She had musli, cottage cheese, other cheeses, plenty of green vegetables, very little processed food, plenty of fruit, including apples and bananas. She also takes vitamin D supplement. You would say a very healthy diet. Trying to find out what has contributed to the problem is not easy, and some of the information appears contradictory.
I’ve had quite a lot of episodes of diverticulitis over about 6-8 years. Was never hospitalized; as soon as I felt a twinge of pain I would stop eating anything but broth, black tea and herbal teas. Then would slowly work my way back up to normal food. Sometimes the pain was pretty bad and I would spend a few days in the recliner.
Haven’t had one for over 2 years now, and I’m sure it’s my diet. Husband and I both needed to lose weight and I chose the paleo diet, since we would simply not be able to stick with a vegetarian diet, and I’ve read that legumes and grains are not really healthy for people. So we eat lots of veggies, plenty of meat & eggs, and good saturated fats; coconut oil, butter & lard, and not so much fruit. We mostly avoid preserved meats like salami, ham, bacon etc. We’ve mostly weaned ourselves off dairy products, but we do love good cheese now and then. We missed the bread & pasta a lot, but are getting used to not having them. So in two years I’ve had no recurrence of the diverticulitis. I do eat nuts and some seeds, but never alone or as a snack by themselves; always as part of a meal, or just after a meal. I feel like that keeps them from having a lot of contact with my intestines/bowel and that the other food kind of smooths the way for them. So far it’s working.
I am happy to find this site. At the age of 76 I am starting to experience relatively mild symptoms of diverticulitis. Given the family history of problems with colon and bowel I realize this has to be watched carefully which is why I am raising the red flag now. I am a bit of a health nut in that I do plenty of exercise, eat a plant based diet (10 years now) which gives me oodles of fiber with great regular bowel movements. I have managed to lose all my extra weight through this diet but had many years of overweight and childhood obesity. So how come I have these symptoms? I have had 2 colonoscopies and there was where I was tipped off about the abundance of diverticuli lining my colon. I did not return to the doctor believing that with my regimen I could handle it. i think I have but recently I need to think about what causes these recent flareups.
1. I love nuts but keep away because of weight. But every one in a while I have a binge on nuts which I just had a few days ago.
2. Flare ups come when I overeat and feel bloated
3. Eating late and going to bed on a full stomach
4. I drink lots of tea but not much water
5. I eat too fast without chewing food adequately.
So for now i am taking all the above into account plus the suggestions described on this site: first a liquid diet for a while then low fiber and gradually back to my regular vegan diet. Meanwhile I am staying away from nuts and anything with seeds, except for my ground flax. I am at the moment cooking congee with is just a thin white rice gruel. The Chinese have many delicious variations but plain or with addition of a little soy it is comforting. Chinese medicine have many medicinal soups. They believe that good health is in what you eat. I may pursue this. Good luck to everyone in their journey to coping with this condition.
Hi all. I have celiac disease, collageneous colitis and most recently had a mild dv episode confirmed by CT scan. No antibiotics, liquids, BRAT diet. Im beginning to think perhaps The Plant Paradox (avoid lectins) may be an avenue I will pursue. Has anyone followed this? Food just does not seem to be my friend. I am one of 4 sisters with celiac, 2 others with IBS, dv. One sister in hospital right now, not responding to antibiotics. I believe there is a genetic connection to this.
Hi Joe,
I have just had my first divertulitis episode – unaware of having diverticulosis previously but uncomfortable enough to try experiment with low FODMAP diet in the past few months:
Your article is the best wrap up I’ve seen yet, including those provided by hospitals after an episode:
Thanks for the clear well organised and thorough article – great to find an evidence based article that is so well written and current – with links and menus as well.
Thanks again
Chris
Hi Chris,
Thanks for the feedback! 🙂
Let me know if you have any questions as you being the low FODMAP diet!
Thanks, Joe.
So this article totally contradicts what others say..I think I will stick to what doesn’t give me pain and running to the toilet..lolol
Three years with pain levels around 7 to 8,0 being good 10 constant pain,I am down to about a 1 pain level after getting all my teeth pulled. Possible the inflammation in my teeth may have cause the inflammation in my stomach,When the dentist pulled my teeth it was better than the oral surgeon he broke three of my teeth and left pieces of teeth the last finally work itself out TOOK three more months to heal than it should.I hoping three more weeks I should be pain free.I have learned to eat soft foods,yogurt, my safe foods are eggs,mash potatoes,biscuits from Dennys,and I get beans,rice,shredded beef,cheese,and sour cream,and Subway meatball sandwich,subway sandwich might be questionable, but so good.oat meal big no,no for me,I am questioning about bananas high acid And seeds???,Might cut them out of my diet.went from 210 to 175 with my Dennys diet and beans,rice, shredded beef cheese and sour cheese, At Dennys I would eat the eggs medium not scrambled they do not use real eggs in their scrambled, and the biscuit, save the mashed potatoes to mix with the beans and rice ,between the two together make about three to four meals.Thanks for listening if it goes to zero in three weeks I will post again,PS,I am 59 hoping 60 will be pain free.
I apprecaite this article and especially the cited research. Thank you for writing it.
The way diet impacts diverticulosis and diverticulitis is a case of science being a few steps behind reality. I had diverticulosis at a young age (33), got diverticulitis repeatedly, and had a left colectomy at age 36 to remove it. The one and only thing that kept it from coming back was eating a plant-based diet, which at the tiem I was not organized enough to do. I would try, but every time I started eating meat and dairy again I would get an infection. It’s simple. Those fodos don’t have fiber, and they are also loaded with chemicals, steroids, and whatever else that is not fit for human consumption.
The reason why western medical science doesn’t get behind plant-based diets is because plant-based diets result in less illnesses and people meeding to take less medication, and then big pharma makes less money. Our standard western diets keep us sick, and th medical money making machine keeps rolling. To point in the article about adding more fruits and vegetables instead of eliminating mats is silly. We only have so much capacity to consume, so we won’t be able to add many fruits or vegetables with a 12 oz. steak sitting in our stomachs. Plus, it’s not all about fiber. The steak likely comes from a factory farm, from some sick cow who is fed in a way that it grows three times faster than it normally would. Then we eat it and, go figure, our bodies have a hard time digesting it.
Hopefully some billionaire will come along and fund enough studies to make it impossible for western medicine to remian under the thumb of its big brother: the pharmaceutical industry. Or, may that billionaire could open a medical school that isn’t reliant on donations from big pharma and research provided by big pharma. We’re all sick wth digestive illnesses and cancer because we eat things our bodies weren’t meant to digest. As smart as doctors inherently are, it’s going to take a doctor or organization with legit ethics and even morality to start doing what is best for patients.
IBS and diverticulitis
hi, my wife suffers with IBS and diverticulitis, we are trying to start a diet based on the diet for foods that are acceptable for an IBS diet that are not acceptable for a Diverticulitis diet and vice a versa