Pseudomembranous colitis refers to inflammation in the gut that is associated with an overgrowth of C. diff bacteria.
This condition can cause very uncomfortable gastrointestinal symptoms that are very serious if not managed properly.
Unfortunately, pseudomembranous colitis is becoming more common with people often experiencing it more than once.
This article explores what to eat and drink during a C. diff infection, and what diet can help prevent pseudomembranous colitis from recurring.
What Is Pseudomembranous Colitis (C. diff Colitis)?
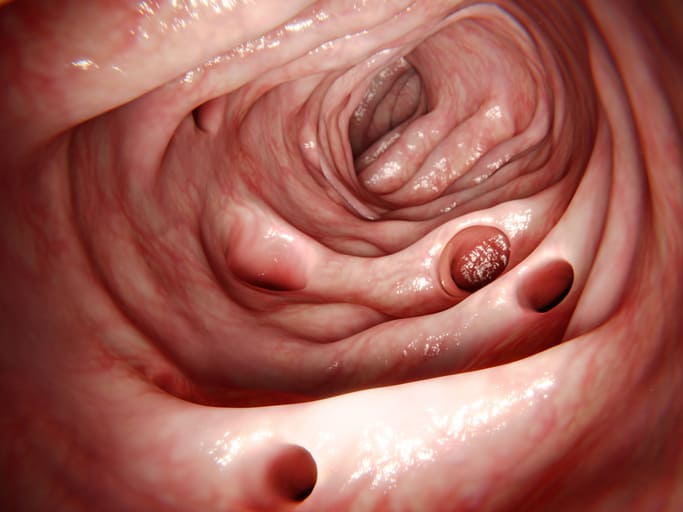
Pseudomembranous colitis is a type of inflammation in the large intestine (also called the gut or colon).
Unlike a similar condition called microscopic colitis, it’s caused by an overgrowth of C. diff (Clostridium difficile) bacteria.
One of the main causes of pseudomembranous colitis is excessive antibiotic use.
Antibiotics are prescribed to kill harmful, infection-causing bacteria. Unfortunately, they also kill beneficial gut bacteria, creating a void in the gut microbiota.
If C. diff bacteria are present, they can seize the opportunity to fill that void and multiply rapidly.
As C. diff grows and multiplies, it produces toxins that injure the lining of the large intestine. This causes inflammation and gastrointestinal symptoms.
Who is at Risk for C. diff?
People taking antibiotics, especially for a long time, have a higher risk of C. diff colitis (1).
Other risk factors for C. diff include (2):
- Advanced age (over 65 years)
- Contact with infected patients or with their healthcare providers
- Weakened immune system
- Taking proton pump inhibitors
- Tube feeding directly into small intestine.
Patients in hospitals and nursing homes are at particular risk, since they often face many of these factors.
Many are older adults who take antibiotics, have weakened immune systems, and are near other people infected with C. diff.
Summary: Pseudomembranous colitis, or C. diff colitis, is inflammation of the large intestine caused by a C. diff infection.
How Does C. diff Bacteria Get Into the Gut?
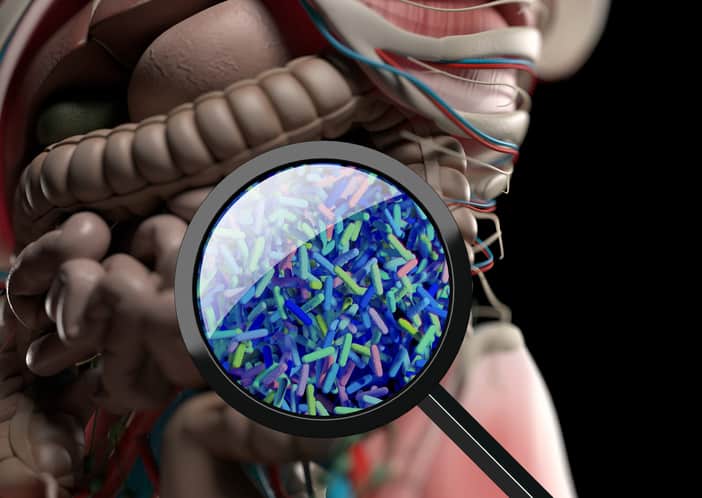
While C. diff can occur in the gut naturally, it’s most often spread through contaminated materials in healthcare facilities.
Approximately 2% of healthy adults naturally carry C. diff in their intestines with no harmful effects. If antibiotics create an opening, however, the C. diff may multiply and cause colitis (3).
Much more commonly, C. diff is spread from person to person.
People with C. diff shed spores in their feces. If strict precautions to prevent contamination aren’t followed, spores can be spread by hands, food and eating utensils. They can then be accidentally swallowed by others.
Summary: While C. diff can occur naturally in the gut, it’s most often spread from person to person. The bacteria produce spores, which can then be swallowed and reach the gut.
Pseudomembranous Colitis Symptoms

When pseudomembranous colitis is relatively mild, symptoms include:
- Watery diarrhea three or more times a day for at least two days
- Mild abdominal cramping.
If it becomes much more severe, it can turn life-threatening and may include symptoms like:
- Diarrhea 10-15 times per day
- Abdominal cramping and pain
- Fever
- Rapid heart rate
- Dehydration
- Loss of appetite
- Weight loss
- Swollen abdomen
- Kidney failure
- Increased white blood cell count.
Diarrhea caused by C. diff is usually very watery and has a characteristic bad odor. Stool may also be soft (rather than watery), and contain mucus. Blood may be present in stools, but is rare (4).
Note that in rare cases pseudomembranous colitis doesn’t cause diarrhea, which makes it much more difficult to diagnose.
Summary: Symptoms of mild pseudomembranous colitis include watery diarrhea and abdominal cramping. In more severe cases, patients may experience frequent diarrhea, cramping, rapid heart rate, loss of appetite, weight loss and increased white blood cell count.
Link Between Inflammatory Bowel Disease and C. diff Colitis
Several studies have found that people with Inflammatory Bowel Disease (IBD) have increased risk of pseudomembranous colitis (C diff. colitis) (6, 7).
Of the two main types of IBD, those with ulcerative colitis (UC) seem to be at especially high risk compared to those with Crohn’s disease (7).
In one study, hospitalized patients with UC were almost eight times more likely to be infected with C. diff, while those with Crohn’s disease were about twice as likely to have it compared to patients without IBD.
Additionally, patients with UC and C. diff had over three times the risk of dying as patients with UC but not C. diff. This increased risk of death was not seen in patients with Crohn’s disease (7).
When people with UC get C. diff it’s often severe. In one study, patients hospitalized for UC flare-ups who also had C. diff were twice as likely to have additional UC-related hospitalizations during the following year.
This group also had almost double the rate of colon-removal surgery compared to UC patients without C. diff (8).
Summary: People with IBD, especially those with ulcerative colitis, are at increased risk of C. diff. When infected they are far more likely to experience severe and even life-threatening symptoms.
Initial Treatment of Pseudomembranous Colitis
When pseudomembranous colitis is diagnosed, generally the first course of action is to stop taking the antibiotics that are suspected of causing the infection.
Ironically, pseudomembranous colitis is also treated with antibiotics. Typically, metronidazole is used for mild to moderate symptoms, and vancomycin is used for severe cases.
Most patients see improvements when treated with appropriate antibiotics. However, up to 35% will develop recurring diarrhea (9).
In fact, as many as 26 pseudomembranous colitis relapses in one person has been reported (10).
If you think you may have a C. diff infection, talk to your physician before discontinuing any antibiotics.
Summary: Discontinuing the antibiotic that is suspected of leading to the infection is usually the first line of treatment. Metronidazole or vancomycin may then be prescribed. While these antibiotics help most people, some will develop recurring pseudomembranous colitis.
What to Eat During a Pseudomembranous Colitis Infection

Choose low fiber, low fat foods and drinks that are easy on the digestive system and don’t make diarrhea worse.
Too much fiber and fat can cause cramps, gas and increased stool volume.
You might also consider limiting high FODMAP foods, or following a low FODMAP diet temporarily.
Many doctors recommend sticking with soft, starchy foods, including:
- Peeled potatoes
- Noodles
- Refined grains (rather than whole grains)
- White rice
- Saltine crackers
- Soup
- Bananas
- Applesauce
- Lower-fiber vegetables (green beans, beets, peeled zucchini).
If you have no appetite, you might find it easier to consume only liquids to start. Sip small amounts of broth or diluted fruit juices.
Once your appetite returns, eat small meals throughout the day, rather than three large ones.
It’s very important to stay well-hydrated. Choose drinks containing water, sugar and some salt to replace the water and electrolytes that you’re losing through your stools. Good choices include:
- Diluted fruit juice
- Caffeine-free soft drinks
- Sports drinks
- Popsicles
- Broths
In cases of severe C. diff colitis, IV fluids and electrolyte replacement may be necessary.
Summary: Soft and starchy foods that are low in fiber can help alleviate the diarrhea caused by C. diff. If you have no appetite, start with liquids like broth or diluted fruit juice, then progress to eating small meals throughout the day. Be sure to drink plenty of fluids to prevent dehydration.
Foods to Avoid During a Pseudomembranous Colitis Flare

Avoid the following foods, which may make diarrhea and dehydration worse during an acute flare up (12):
- Fried and greasy foods
- Foods with creamy sauces
- Cakes and cookies
- Fruits and vegetables that can cause gas and bloating. Typically these are high FODMAP foods like garlic, onion, dried beans, peas, prunes, chickpeas and other legumes
- Caffeine and alcohol.
Some people have a hard time digesting lactose, a sugar found in milk products. If these foods seem to bother you, either decrease your intake or avoid them completely.
You can also try lower-lactose foods like yogurts with live active cultures and aged cheeses (cheddar, Swiss and parmesan).
Summary: Avoid high fat and gas-causing foods, as well as dehydrating beverages or those you know you are sensitive towards.
Best Diet to Prevent Recurring Pseudomembranous Colitis

Not much research has looked at whether particular foods or diets can prevent pseudomembranous colitis.
However, there’s one interesting study that looked at the effects of drinking kefir.
Patients being treated for recurring pseudomembranous colitis who drank at least five ounces of kefir three times a day for at least two months were more likely to remain free of diarrhea during the following nine months than those who didn’t.
This success rate is equal to that of fecal microbiota transplantation, currently the most successful treatment option for recurring pseudomembranous colitis (13).
Foods that contain probiotics (live beneficial bacteria), like kefir, are known to beneficially impact gut health as well as overall health. It’s possible they may also help stop C. diff recurrences.
Yogurt, quark, sauerkraut, tempeh and miso may all contain probiotics. Check the packaging of these foods to make sure that they contain live active cultures.
Best Diet or Eating Pattern?
There is no one best diet for everyone.
However, the Mediterranean diet is an eating pattern thought to benefit gut bacteria and should be considered first for those with a C. diff infection (14).
It’s unknown if this eating pattern can directly lessen the risk of C. diff recurrence, but it’s a healthy way to eat overall regardless. It focuses on:
- Whole grains
- Fruits
- Vegetables
- Legumes
- Fish and poultry
- Nuts
- Extra virgin olive oil.
Summary: Eat foods that may benefit gut health, including those with probiotics. Early evidence shows kefir in particular may lower the chance of recurring C. diff colitis. Following a Mediterranean diet may also have beneficial effects on gut bacteria.
Probiotics and Supplements For Pseudomembranous Colitis

The use of probiotic supplements to prevent or treat pseudomembranous colitis has shown conflicting results.
While some small studies suggest small benefits, larger and more well-designed studies found minimal benefits (15).
At the 2015 Yale University workshop on probiotics, it was concluded that either the probiotic strains Saccharomyces boulardii or Lactobacillus GG are the most effective for treating diarrhea associated with C. diff (11).
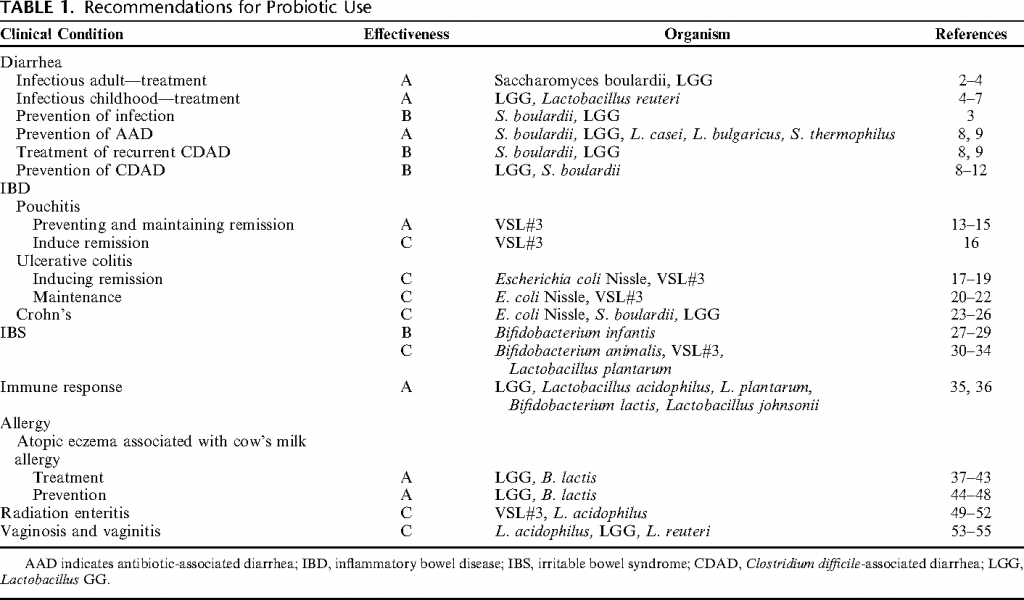
If you want to try a probiotic, go for a product that contains either of those as it’s primary probiotic strain.
- For Saccharomyces boulardii I recommend Nexabiotic (available on Amazon).
- For Lactobacillus GG I recommend Culturelle (available on Amazon).
It might not work but it’s certainly worth a shot!
Supplements for C. Diff
One recent study looked at another supplement called indole-3-carbinol.
Researchers found that mice infected with C. diff who were given indole-3-carbinol had significantly milder symptoms and were less likely to die than those not given the supplement (16).
While these results are promising, the effect of this supplement on humans is still unknown.
Summary: Probiotic supplements are still speculative, although products with Saccharomyces boulardii or Lactobacillus GG are worth a try. There aren’t any other supplements that have shown to be effective in humans with C. diff.
You Can Overcome Pseudomembranous Colitis
Pseudomembranous colitis is an inflammation of the large intestine associated with an overgrowth of Clostridium difficile (C. diff) bacteria.
If you’re having diarrhea caused by C. diff, it may help to eat starchy, low-fiber foods like white rice, saltine crackers and soup. Eat these as part of small meals, and be sure to drink plenty of fluids.
To prevent pseudomembranous colitis from recurring, choose foods that benefit your gut bacteria. These include products with probiotics like yogurt (with live active cultures), kefir and sauerkraut.
There are two types of probiotics that may help too, which is worth considering if you have been experiencing recurring flare ups.
As for a general eating pattern, the Mediterranean diet appears to be a good choice.
Following these recommendations and being consistent with your diet changes and improvements can go a long way to prevent the inflammation from recurring.
What Can And Can’t I Eat On The Low FODMAP Diet?
Often it’s easiest to start with this giant list I’ve made of what foods to eat, and what foods to avoid when following a low FODMAP diet.
It’s based on the latest published FODMAPs data (1, 2, 3, 4, 5).
Print or save to your phone to use as a quick-reference guide when shopping or cooking. I’ve attempted to list foods in both US and UK/Aus names, with US first.
I’ve included a screenshot of the first page below. But the full PDF is 4 pages and suitable for printing. To download it simply tap the box below and it will then be emailed straight to you – it’s free!


I didnt see any recommendation to stop eating conventional food with roundup involved as in keeping the orchard free of weeds (almonds), drying the crop several days before harvest (wheat especially but any cereal grain, and dozens of other crops). Glyphosate is patented as an antibiotic so it kills the good bacteria so the bad can flourish?