[Last updated 10th April, 2019]
There’s a lot of information online about hypothyroidism and Hashimoto’s disease.
Some of it is accurate and unbiased… but most isn’t.
This guide summarises the best recommendations from both science-based and alternative medicine, all in one place.
Fundamentals and Causes
What Is The Thyroid and How Does It Work?
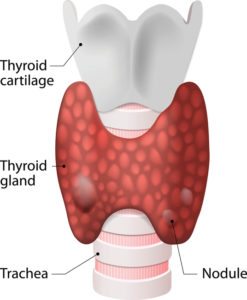
The thyroid is a small butterfly-shaped gland on the front of your throat.
It produces two types of thyroid hormone – Triiodothyronine (T3) and Thyroxine (T4). These hormones help to regulate metabolism, sending instructions to every cell in your body.
Many metabolic processes shut down without them.
Watch this 3-minute TED-Ed animation:
Summary: The thyroid is a small gland on your throat central to regulating metabolism.
What Is Hypothyroidism?
Hypothyroidism (also known as an underactive thyroid or low thyroid) is the term to describe a thyroid gland that does not produce enough thyroid hormone.
It’s estimated that up to 8.5% of people from Western countries has hypothyroidism. That’s around 20 million Americans (1).
It’s caused by poor function of the gland itself, or by not receiving adequate stimulation to “switch on” properly. There are several reasons why this might occur (2, 3):
- Hashimoto’s disease
- Removal of thyroid
- Radioiodine treatment
- Diseases and conditions that affect the pituitary gland.
Left unmanaged, hypothyroidism leads to numerous health problems such as rapid weight gain, fatigue, poor memory and hair loss.
Summary: The inability of your thyroid gland to produce adequate hormone is called hypothyroidism. It’s estimated to affect around 8% of the Western world.
What Is Hashimoto’s Disease (Hashimoto’s Thyroiditis)?
Hashimoto’s Disease is easily the most common form of hypothyroidism in the Western world.
It’s also known as Hashimoto’s Thyroiditis and Hashimoto’s Hypothyroidism.
It occurs when your immune system mistakenly attacks and damages the thyroid gland. This is what is known as an autoimmune disease, with Hashimoto’s being the first recognised condition.
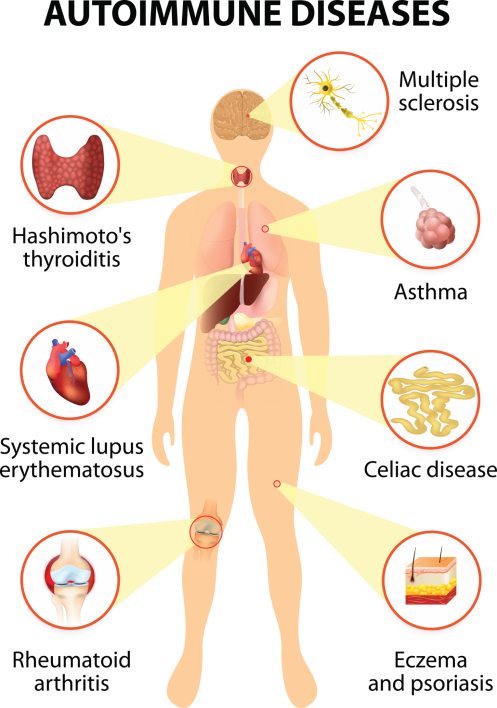
There are many theories as to why people develop autoimmune diseases. The main reasons remain unclear to researchers, but it appears to be multifactorial. Your genetics, environmental factors (including stress, infections or drugs), and the balance of gut bacteria (gut dysbiosis) are thought to be key triggers (4).
The main focus of this guide is Hashimoto’s disease, although many aspects still apply to other causes of hypothyroidism.
What Is Leaky Gut and Is It Real?
Leaky gut (syndrome) is a condition thought to cause autoimmune diseases, including Hashimoto’s. At least, theoretically.
The idea is the lining of our gut (intestine) can expand or “leak” under stress. This can allow large food molecules and other compounds into the bloodstream, rather the just the usual small nutrients.
These large food molecules then interact with the immune system to cause severe problems. It’s said to be the root cause of mental health problems, autoimmune disease, irritable bowel disease and more.
The concept is recognised in medicine as intestinal permeability, and is known to be a symptom in patients with inflammatory bowel disease or celiac disease. However, no studies indicate it causes diseases or conditions, nor that it occurs in otherwise healthy people (5).
The science in this area is far from conclusive though, and the theory could very well hold some truth. But to confidently claim it’s the root cause of numerous health conditions – based on our current understanding – is misguided and misleading.
Summary: Hashimoto’s disease is an autoimmune disease caused when the immune system mistakenly attacks and damages the thyroid gland. It’s not understood why autoimmune problems occur, but diet and stress both play a large part.
Hashimoto’s and Hypothyroidism Symptoms
There are many well-recognised symptoms of hypothyroidism (Hashimoto’s and otherwise), which you can see here.
The most common from that list include:
- Excessive fatigue
- Rapid weight gain
- Constipation
- “Brain fog”
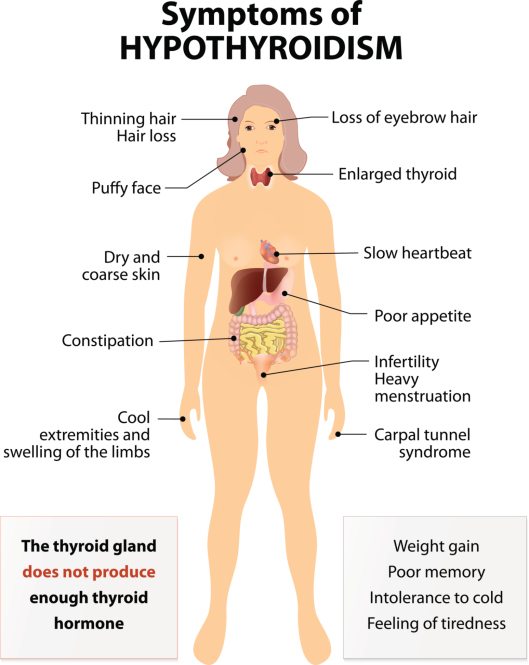
If you experience three or more of these hypothyroid symptoms, it’s recommended to have your thyroid checked at the doctor.
How Is Hashimoto’s Diagnosed?
Diagnosis is based on a combination of physical examination, blood tests, medical history and family history.
What Doctor Should I See?

Your doctor or GP provides the initial examination and blood test.
Depending on the result, you may be referred to an endocrinologist (also known as an “Endo”). This doctor specialises in the endocrine system, which includes the hormones and related organs and glands.
You might be referred to see an endocrinologist if you:
- Are taking thyroid medication but symptoms persist
- Have a goiter, which is a lump or growth on your thyroid
- Are pregnant or intend to become pregnant and already have diagnosed hypothyroidism. Patients often require up to 50% more thyroid hormone during this time.
- Have hypothyroidism caused by a pituitary disorder
Summary: You will most likely be referred to an Endocrinologist, who specialises in hormones.
Physical Examination
You will typically be asked to drink a glass of water while the doctor feels (palpates) your thyroid.
Your doctor is looking for thyroid enlargement (goiter), or any strange lumps in the area around your thyroid (6).
Your doctor may also look at some other clinical signs related to hypothyroidism including:
- Assess your reflexes
- Look at your weight history
- Listening to the thyroid through the stethoscope
- Examine your eyes and face for puffiness, and your hair for thinning
- Measure your body temperature.
Summary: Physical checks usually involves palpating areas around your thyroid.
Blood Tests For Hypothyroidism
Blood tests are the most important for diagnosis as specific tests reveal exactly how well your thyroid is working.
TSH is always performed, while other tests are used where needed:
Thyroid-Stimulating Hormone Test
TSH (Thyroid Stimulating Hormone) is a hormone that controls thyroid function.
It (usually) fluctuates in line with the amount of thyroid hormone in your system. If thyroid hormone levels are low, then TSH secretion is increased. If high, TSH is reduced.
This makes it a useful marker for testing thyroid function, and has been the gold standard hypothyroidism diagnosis test for decades. You doctor will usually re-check TSH every 3-6 months.
TSH reference ranges alter slightly as we grow older and if you are pregnant:
TSH levels for premature birth (28‑36 weeks):
- 0.7‑27 mIU/L (milli-international units per liter)
TSH levels for children:
- Birth to 4 days: 1‑39 mIU/L
- 2‑20 weeks: 1.7‑9.1 mIU/L
- 21 weeks to 20 years: 0.7‑64 mIU/L
TSH levels for adults:
- 21‑54 years: 0.4‑4.2 mIU/L
- 55‑87 years: 0.5‑8.9 mIU/L
TSH levels during pregnancy:
- First trimester: 0.3‑4.5 mIU/L
- Second trimester: 0.3‑4.6 mIU/L
- Third trimester: 0.8‑5.2 mIU/L
Those on Levothyroxine have a goal TSH range of 0.5-2.5 mU/L. However, some organisations believe a reading of 2.5 or less is truly ideal, with anything 2.5-4.0 mIU/L considered “at risk”.
Also note slight variations in results can occur depending on the laboratory used, as well as the time of day your blood was drawn.
Free T4 Test
T4, or thyroxine, is the active thyroid hormone in your blood. Free T4 refers to the amount of total T4 available in your tissues.
Your doctor may test how much free T4 is in your blood to help diagnose Hashimoto’s, but the test is used to complement the TSH test.
Normal Levels for Total Thyroxine (T4):
- 11.8-22.6 mcg/dL (152-292 nmol/L) in newborns
- 6.4-13.3 mcg/dL (83-172 nmol/L) in babies and older children
- 5.4-11.5 mcg/dL (57-148 nmol/L) in adults
Normal Levels for Free Thyroxine FT4:
- 0.7-2.0 ng/dL or 10-26 pmol/L.
Free T3
This test measures free T3 hormone levels, however is rarely ordered to diagnose hypothyroidism.
Free T3 levels will only be low if the hypothyroidism is severe. These are classified as normal levels for the T3 blood test:
Total T3
- 105-245 ng/dL (1.6-3.8 nmol/L) in children ages 1-14
- 82-213 ng/dL (1.3-3.28 nmol/L) in adolescents ages 12-23
- 80-200 ng/dL (1.2-3.1 nmol/L) in adults
Free T3
- 260-480 pg/dL or 4.0-7.4 pmol/L in adults
Reverse T3
Reverse T3 (rT3 or REVT3) is an inactive form of T3.
Normally your liver converts a large percentage of T4 into T3, with a smaller percentage becoming rT3 before being eliminated from the body.
However, in certain period of stress, as much as 50% or more of T4 will convert to rT3. This is a problem because rT3 competes with T3, and ends up inhibiting T3 production.
Reverse T3 is not a conventional test used by endocrinologists, although integrative practitioners believe it should be used more often.
The test is typically used to diagnose Sick Euthyroid Syndrome
Antibody Tests
With an autoimmune disease, antibodies are malfunctioning immune cells that mistakenly attack the body’s healthy cells.
In the case of Hashimoto’s, these antibodies attack the cells of the thyroid gland.
An antibody test such as a TPO antibody test or anti-thyroglobulin antibody test can reveal the level of harmful antibodies in the blood. These are the antibodies that inhibit important enzymes involved in thyroid hormone production and function.
Summary: TSH is considered the gold-standard for diagnosing hypothyroidism, however occasionally additional tests will be required. There is some disagreement between conventional and alternative practitioners on the significance of certain tests.
Is TSH An Accurate Marker For Hypothyroidism?

Endocrinologists have long considered TSH the most sensitive and accurate indicator of hypothyroidism.
However, recent research suggests it’s far from perfect. The medical system’s systematic reliance on it may actually be leaving many hypothyroid cases under-diagnosed, or even completely undiagnosed.
Some clinical trials showed that TSH and T3 can decline at the same time, particularly in obese individuals that lost weight (7, 8).
That means when T3 levels are low, TSH may remain in the normal range rather than becoming elevated.
Some medications, such as metformin, have also been shown to lower TSH levels in PCOS and diabetic patients with hypothyroidism (9).
Considering the pituitary gland (which produces TSH) is unique in its function, it makes sense that several outside stressors and metabolic processes can influence TSH activity.
This is certainly something to discuss with your doctor if your TSH readings are high-normal, yet you still feel seriously unwell.
I’ve written in much more detail about TSH here.
Summary: Certain outside stressors may influence TSH, so it’s not always 100% reliable on its own.
Possible Complications If Left Untreated
Left untreated, Hashimoto’s disease can lead to a number of serious health problems:
- Goiter: An enlargement of the thyroid gland that may affect breathing or swallowing.
- Heart problems: It has been linked with an increased risk of heart disease, an enlarged heart and, in rare cases, heart failure.
- Mental health issues: Such as depression and memory problems.
- Myxedema: A very rare and severe form of hypothyroidism. If you experience extreme cold intolerance and drowsiness seek medical attention.
- Birth defects: There may be a higher risk of birth defects (ie. cleft palate, heart, brain and kidney problems) in babies born to women with untreated Hashimoto’s disease. If you are planning to get pregnant or if you’re in early pregnancy, be sure to ask your doctor to check your thyroid.
As an autoimmune disease, it also increases the risk of developing additional autoimmune issues, such as (10, 11) :
- Rheumatoid arthritis
- Graves’ disease
- Addison’s disease
- Premature ovarian failure
- Type 1 diabetes
- Lupus erythematosus
- Pernicious anemia
- Thrombocytopenic purpura
- Vitiligo
In very rare instances, Hashimoto’s disease may increase the risk of developing a thyroid cancer known as thyroid lymphoma. Be sure to report any quickly growing thyroid nodules (lumps) to your doctor as soon as possible.
Summary: Hashimoto’s disease must be treated properly in order to avoid several other dangerous health conditions. It may also increase your risk of developing additional autoimmune conditions.
What Is Subclinical Hypothyroidism?
Subclinical hypothyroidism is like a mild form of hypothyroidism.
It’s diagnosed when you have a combination of:
- No symptoms or very mild symptoms of hypothyroidism;
- A slightly raised TSH level;
- A normal thyroxine (T4) level;
- Tested positive for antithyroid antibodies.
In this case you may or may not require thyroid hormone medication, depending on your doctor’s assessment.
About 1 in 10 people with subclinical hypothyroidism will develop hypothyroidism within 3 years (12).
Summary: Subclinical hypothyroidism is a mild form of underactive thyroid that may not require medication. However, it does increase your risk of developing hypothyroidism within 3 years.
Hypothyroid Medication

Hypothyroidism is treated with hormone medication, also known as Hormone Replacement Therapy.
It’s necessary to restore thyroid function and hormones to a healthy level.
Diet and lifestyle changes are also fundamental for treating Hashimoto’s disease, and help support thyroid health and minimise (or even eliminate) symptoms.
What Medication Is Used?
The most commonly prescribed medication is Levothyroxine, and has been the “gold-standard” treatment since the 1960s.
Although Levothyroxine is man-made, it’s identical to the natural thyroxine (T4) produce by your thyroid gland.
Levothyroxine goes by several other names and brand names including:
- Synthroid
- LT4
- Thyroxine
- Levoxyl
- Levothroid
- Levo-T
- Novothyrox
- Unithroid
- Tirosint
Summary: Levothyroxine is the main medication, and is identical to the natural thyroxine your thyroid produces.
Optimal Levothyroxine (Synthroid) Dosage
It’s rare that a hypothyroid patient finds their ideal dose right away, especially if already experiencing symptoms.
Doctors will typically use weight as an initial guideline for determining dosage, but this will almost always change when you have regular check-ups. Treatment is for life so your needs will change as your body changes.
Broad reference ranges can be seen here, but requirements are also on a case-by-case basis.
Synthroid is the most commonly-prescribed brand of Levothyroxine, and is available in 12 strengths for easy dose adjustment.
Also be aware that thyroid hormone fluctuates throughout pregnancy, so you will have to get blood tests more regularly to manage the dosage.
How Long Does It Take To Manage Symptoms?
Thyroid hormones act slowly in the body.
This means it takes several weeks to months for your symptoms to resolve. This also depends on how well you tolerate your thyroid hormone dosage.
One of the first improvements reported with Levothyroxine is improved energy levels (less fatigue). It’s also been shown to gradually lowers cholesterol levels and may help reverse weight gain.
Summary: Dosage requirements are calculated on an individual basis with your doctor. It can take weeks or months before noticeable improvements.
When Should I Take Levothyroxine?

Levothyroxine must be taken on a fasting stomach.
This is because absorption is greatly reduced if consumed alongside food or drinks.
That means take it either before breakfast, before you go to bed, or any other time that is at least 1 hour outside of meal times.
What Time Is Best?
There have been 4 large clinical trials investigating best time.
Out of the 412 patients studied, one study found T4 hormone absorption was better in the morning, one found it was better at night, and two found no significant difference (13, 14, 15, 16).
Ultimately, neither option is better or worse than the other.
If you want to have your medication in the morning, most find it easier to have a late breakfast (often at work). Alternatively, you can also get in the habit of skipping breakfast altogether.
For those who prefer to take their medication at night time, that typically means committing to no food or drink after 8pm (which is a good thing). But insomnia is a common complaint of those who take their medication before bed, as is increased urgency to urinate during the night.
Summary: Thyroid medication must be taken on a fasting stomach, at least 1 hour (but preferably 2 hours) before or after food and drink. There is no difference between taking Levothyroxine in the morning vs evening, so choose what is easiest for you to stick with.
Is It Safe For Me?

Levothyroxine is widely regarded as the safest and most effective form of thyroid hormone.
However, there are certain health conditions that can influence its effectiveness.
To confirm it’s safe for you, tell your doctor if you have:
- Anemia (low red blood cells)
- Osteoporosis (more on that below)
- Pituitary gland or adrenal gland issues
- History of heart disease or stroke
- Type 1 or type 2 diabetes
- Food or drug allergies
- Received iodine radiation therapy
- Thyrotoxicosis (a thyroid disorder)
Summary: Levothyroxine is the safest, however it may not be appropriate in certain conditions.
Levothyroxine (Synthroid) Side-Effects
Undesirable side-effects of Levothyroxine are reported quite frequently, unfortunately.
Common symptoms include:
- Fever
- Heat intolerance
- Irritability
- Difficulty with swallowing.
If you experience any of these then you must speak with your doctor.
Summary: Side effects of Levothyroxine are not uncommon.
Does Thyroid Medication Cause Osteoporosis?

Osteoporosis is a progressive bone disease that increases your risk of fractures.
It’s thought that hyperthyroidism (overactive thyroid producing too much T4) increases fracture risk, particularly in postmenopausal women and older people (17).
For this reason, the long-term use of Levothyroxine (T4) to treat hypothyroidism has come into question.
But it’s the age of the patient, and dosage they take, that are the important considerations.
There seems to be no significant relationship between the daily levothyroxine dose and fracture risk in “non-severe” osteoporosis patients, such as young adults. However, doses of >150 µg per day are associated with a higher risk of fracture in elderly patients who already have severe osteoporosis (18).
Other studies have also found long-term use may increase risk in postmenopausal women, particularly at high dosages (19, 20).
Unfortunately, high doses are more common than they need to be, with approximately 20% of levothyroxine patients being over-prescribed (18).
This highlights the importance of monitoring your thyroid status and medications regularly with your doctor, especially after menopause.
Summary: Long-term or high dose Levothyroxine use does not appear to increase risk of osteoporosis in hypothyroid patients prior to menopause. However, it could very well affect elderly men and women, especially if they already have osteoporosis.
Alternative Treatment Options
Some people do not tolerate Levothyroxine well, regardless of the dosage.
The most commonly reported side-effect is severe nausea, to the point where it affects their day-to-day life.
Fortunately there is an alternative.
Desiccated Thyroid For Hashimoto’s Disease

Desiccated thyroid is a thyroid hormone supplement made from animal thyroid glands, typically pig thyroid.
It’s a popular natural alternative to conventional thyroid medication, and actually became a commercial thyroid treatment before Levothyroxine.
It consists of a mixture of T4 + T3 hormones, whereas Levothyroxine is only T4.
It’s a prescription supplement in most countries, and is available under several brand names including:
- Armour Thyroid
- Nature-Thyroid
- WP-Thyroid
Summary: Desiccated thyroid is an alternative to Levothyroxine, typically made from pig thyroid gland.
Desiccated Thyroid vs Levothyroxine
Clinical trials using a mix of T4 + T3 (desiccated thyroid) have found it is, at best, equally as effective as Levothyroxine for treating hypothyroidism (21, 22, 23).
Note that it never surpasses the effectiveness of Levothyroxine.
This is why products like Armour Thyroid are typically used as a back-up option for those who do not respond favourably with Levothyroxine.
Summary: Studies show desiccated thyroid can be as effective as Levothyroxine for replacing thyroid hormone, but not consistently.
Is It Safe For Me?

Desiccated thyroid is generally safe.
However, even though they are FDA regulated, supplements aren’t subject to the same strict safety and effectiveness requirements that pharmaceutical drugs are.
In fact, a study on “thyroid support” supplements found that half of brands contain a low range of T4, while 1 in 10 contained no T4 at all.
In other words, taking desiccated thyroid comes with more risk for potentially no extra benefit than standard Levothyroxine.
Summary: Desiccated thyroid is recognised as safe, but the quality and consistency of doses is not regulated in the same way as medication.
What Are The Benefits of Desiccated Thyroid?
The benefits are far fewer side effects for those who cannot tolerate Levothyroxine.
In fact, most users (including the participants in the studies cited above) report better tolerance and preference for desiccated thyroid (24).
Anecdotal evidence (personal testimonial) suggests desiccated thyroid still treats symptoms effectively, without the common side-effects of Levothyroxine.
Summary: Users report much better tolerance than Levothyroxine, which suggests it’s a good alternative.
What is LDN (Low Dose Naltrexone)?
Naltrexone is an FDA-approved drug that blocks opiate receptors.
These are the receptors that heroin and opiate drugs binds to, which is why naltrexone was a popular opiate addiction treatment in the 1980’s.
As the name suggests, LDN is a low dose of naltrexone. More recently is has been used to “boost” the immune system, with some theoretical and anecdotal evidence it can help treat autoimmune diseases, such as Hashimoto’s.
There is some early scientific evidence that has found promising effects, particularly for Crohn’s disease. However, much more research is needed before it should be recommend for other conditions, particularly Hashimoto’s.
Summary: LDN is emerging as an alternative treatment for autoimmune disease, but research is in its infancy.
Diet and Lifestyle Changes
The health of your thyroid is greatly influenced by your eating pattern.
Understanding what nutrients are key is especially important when your thyroid is underactive.
Nutrients To Maintain Thyroid Health
There are several nutrients known to help optimise thyroid health and function.
Iodine

Iodine is a trace element the thyroid gland requires in order to produce thyroid hormone.
An iodine deficiency can cause hypothyroidism, however, this is very rare in developed countries. Iodine is abundant in our food supply, with most countries adding it to food-grade salt or bread (25, 26).
As an example, the World Health Organization (WHO) deems a population iodine deficient if urine concentration levels are less than 100 microgram/L. Americans had a median level of 160 microgram/L in 2003-2004, while Australians were at 124 microgram/L in 2011-2012 (27).
Nevertheless, including iodine-rich foods can be a good idea to be extra safe. The best sources of iodine include:
- Seafood
- Iodised salt
- Eggs
- Navy beans
- Potatoes
- Cow’s milk
You can learn more about dietary iodine here.
Selenium

Selenium is an essential mineral that helps the body to recycle iodine.
That’s the reason the thyroid has the highest selenium content (per gram of tissue) of all our organs (28).
It’s thought that low selenium levels contribute to hypothyroidism through alternate mechanisms related to iodine. For this reason it’s fundamental to eat a diet that contains many selenium-rich foods, such as:
- Eggs
- Legumes
- Brazil nuts
- Tuna and sardines
- Beef and chicken
Zinc

Zinc is an essential mineral required to regulate the hormone that stimulate thyroid hormone production, TSH.
In fact, the metabolism of zinc and thyroid hormones are closely interlinked, which is why a deficiency can lead to hair loss (known medically as alopecia) (29).
Studies show that zinc deficiency is very uncommon in the developed world. In any case, it’s still recommended to eat a variety of zinc-rich foods such as:
- Oysters and shellfish
- Beef and chicken
- Legumes, nuts and seeds
- Milk and yoghurt.
Summary: Iodine, selenium and zinc are the main nutrients to be aware of. You are more at risk of a deficiency in one or more of these nutrients if you are vegetarian or vegan
Should I Supplement These Nutrients (Thyroid Support Supplements)?
Natural thyroid support supplements typically contain one or more of the important nutrients for thyroid health.
But are they necessary? This is a very common question, and you can’t expect an unbiased answer from the supplement manufacturer.
Let’s break down the 4 main nutritional aspects that thyroid support supplements claim to assist.
Iodine Supplements
Iodine supplements are unnecessary.
This is because iodine deficiency is almost never the cause of hypothyroidism in developed countries (27).
The big exception to this rule is if you are pregnant or breastfeeding. Iodine requirements increase by more than 60% as iodine is required for mother and child.
Women who fall into this category should definitely be supplementing with iodine, as per the World Health Organisation’s recommendations.
Note that in some instances of Hashimoto’s, concentrated iodine sources such as iodine drops, seaweed or kelp tablets may worsen hypothyroidism. This is another reason to be weary of iodine supplementation, and you should certainly inform your doctor before trying anything new.
Selenium Supplements
Selenium is a popular thyroid supplement, and theoretically could help if you are actually deficient in selenium.
A large review of the research in 2013 concluded evidence is lacking to definitively support or refute the use of selenium for thyroid health. Some studies found it could help, but they were heavily biased (30).
In other words, it’s unclear if is beneficial from a scientific standpoint. It does look promising for those with Graves’ disease, and anecdotally it helps, but you need to try for yourself (31).
Note there is also the risk of side-effects to consider, including digestive issues, fatigue, irritability and even hair loss if used long-term.
Zinc Supplements

There are few studies on zinc supplementation, with one finding it may only be beneficial for patients with goiter (32).
Therefore, there is no way to give a solid recommendation for or against its use.
If you are experiencing hair loss, it may be worth trialling a zinc supplement on its own (as opposed to a supplement that also contains selenium).
Vitamin B12 Supplements
Vitamin B12 is a micronutrient that helps regulate energy release.
Low levels can make you feel exceptionally lethargic, so in theory this supplement could help fight fatigue that comes with underactive thyroid.
Generally speaking it doesn’t hurt to give it a try, and anecdotally they work very well. But much like iodine, low levels of vitamin B12 is very rare in developed countries if you eat a wholesome and varied diet.
Summary: Generally speaking, supplemental iodine and vitamin B12 are not necessary as your levels are likely optimal. Selenium and zinc supplements are certainly beneficial if you have low levels, but effectiveness will vary greatly between individuals. Always consult with your personal doctor before trying any new supplements.
Hashimoto’s and Gluten

Gluten is a protein that naturally occurs in wheat and grains.
It’s poorly digested by around 6% of the population, and many studies have found a strong link between gluten intolerance (as well as celiac disease) and hypothyroidism.
In fact, roughly 16% of those with celiac disease (another common autoimmune disease) have antibodies that damage the thyroid (33).
Based on this link, many researchers suspect that individuals with Hashimoto’s may improve when gluten is removed from the diet.
However, current research is a mixed bag. In other words, it really depends on the individual.
If you have a family history of autoimmune disease, or your symptoms are not improving despite lifestyle changes and thyroid medication, removing gluten from your diet may be of great help.
To learn more about the studies and recommendations, click here.
Summary: Numerous observational studies and anecdotal reports suggest gluten-free is beneficial for hypothyroidism. It is certainly warranted in some cases.
Hashimoto’s and Goitrogens

Goitrogens are substances that, in large doses, can aggravate the thyroid and disrupt the production of thyroid hormones.
Cruciferous vegetables such as cauliflower, cabbage and broccoli are the richest source of goitrogens in our diet. Theoretically then, eating these foods would be bad for your thyroid.
However, studies show this is only the case if you are severely iodine deficient (incredibly rare in developed countries), you have a goiter, or you consume ridiculously large quantities of cruciferous vegetables.
Context Is Important
The idea that goitrogens harm the thyroid really took off in the mid 1990s.
Rats fed a diet rich in raw cabbage suffered thyroid problems after 60 days, even with optimal iodine intake. However, for the purpose of that study, cabbage made up a whopping one-third of the rats’ diet (34). For a human to eat this amount of raw cabbage – for 60 days straight – is impossible.
Then there was a stand-alone case study of a Chinese lady that “overdosed” on goitrogens. She was diagnosed with severe hypothyroidism (myxedema coma) after eating an estimated 3.3 lbs (1.5 kgs) of raw bok choy per day for several months (35). She believed it would help control her diabetes.
Assuming you don’t eat phenomenal amounts of raw cruciferous vegetables every day, they are safe to eat. In fact, cruciferous vegetables are so nutrient dense that they will do you much more good than harm.
Additionally, cooking cruciferous vegetables and other foods containing goitrogens are thought to greatly reduce its potential impact. A small study in 10 subjects showed that eating 0.3 lbs (150 g) per day of cooked brussels sprouts for four weeks straight had no negative effects on thyroid function (36).
The other concern is that goitrogens inhibit the absorption of thyroid hormone if consumed at the same time. While this may be true, thyroid hormone should always be taken on an empty stomach at least 1 hour before any food.
Summary: If you don’t have a goiter or an iodine deficiency, cruciferous vegetables are safe to eat. Cooking food is thought to greatly reduce the activity of goitrogens in any case. The risk only outweighs the benefit if cruciferous vegetables are consumed in ridiculously large quantities and/or raw.
Diet Plan For Hashimoto’s Disease and Hypothyroidism

You can find a set diet plan (meal plan) – including the shopping list – here: 14-Day Meal Plan for Hypothyroidism and Weight Loss.
Otherwise this list highlights the important nutrient and diet considerations for hypothyroidism.
Do eat:
- Iodine-rich foods such as potatoes, seafood, eggs, navy beans and iodised salt.
- Cooked cruciferous vegetables such as cabbage and broccoli in reasonable amounts. These are completely safe if you don’t have goiter.
- A high protein diet, which helps curb appetite and keep you feeling full. Focus on eggs, dairy foods, legumes and seafood.
Don’t eat:
- Gluten if you suspect you have an intolerance or celiac disease, or if you continue to feel unwell despite thyroid medication.
- Desiccated thyroid unless Levothyroxine gives you unpleasant side-effects.
- Any food within 1-2 hours of taking your thyroid medication, as this inhibits absorption.
- Any new supplements without first speaking with your doctor.
- Anecdotal evidence (individual reports) suggest caffeine should be limited to less than 300 mg per day as large amounts can aggravate the thyroid. This is equal to 2-3 regular coffees.
Exercise For Hashimoto’s and Hypothyroidism

We should all aim to be more physically active, hypothyroidism or not.
Not only does exercise improve strength and metabolism, it influences how our body responds to hormones. This includes insulin and thyroid hormones (37).
A study of 60 subjects found that short bouts of moderate-intensity exercise (70% of maximum heart-rate) increases circulating levels of T4 and free T4, which is beneficial (38).
If mobility is a problem for you, regularly lifting weights (or bodyweight exercises) is an equally great alternative. Youtube is a great starting resource for beginners who want to try some resistance exercise programs at home.
Summary: Regular exercise, whether cardio or weight training, can improve how your body responds to hormones such as T4.
Yoga and Meditation For Hashimoto’s Disease
Several complementary or alternative practices have been trialled for hypothyroidism treatment.
Small studies on hypothyroid patients found certain forms of yoga helped improve lung capacity and self-reported quality of life scores (39, 40).
However, there is no evidence it directly helps improve thyroid health or symptom management.
Meditation and breathing exercises are also popular alternative treatment options. The one related study I found looking at transcendental meditation and its effect on hormones showed no positive influence on TSH levels (41).
There is no doubt that stress management practices improve overall health, but there is no direct link to thyroid health at this stage.
Summary: Studies do not support a direct link between yoga or mediation and improvements in thyroid health.
What If Those Changes Didn’t Help Me?
If several months of diet and lifestyle changes have not improved your quality of life, the next step may be the Autoimmune Protocol diet.
Also known as the AIP, it’s a strict elimination diet designed to help manage all types of autoimmune disease, including Hashimoto’s.
It’s based on the premise that all autoimmunity issues come from a gut bacteria imbalance plus low-grade inflammation of our cells (42, 43).
The AIP diet helps you to identify and remove known and suspected food chemicals that cause these problems; at least theoretically.
The lack of studies on autoimmune diseases in general – let alone on the effectiveness of elimination diets – leaves us without any science-based recommendations. In theory the AIP may help if you can stick to it long-term, and the anecdotal evidence (patient testimonial) is impressive.
It’s worth considering given there are no other alternatives at this stage. To learn more about this diet plan, click here.
Summary: The Autoimmune Protocol diet (AIP) is a strict elimination diet that can be considered a last option. It’s not evidence-based, but theoretically could help.
How To Lose Weight With Hashimoto’s Hypothyroidism

Losing weight with hypothyroidism is typically more challenging than normal.
This is because your metabolism has slowed, coupled with always feeling tired.
But weight loss is one of arguably the best way to improve how your body responds to TSH and thyroid hormones (44).
Breaking down each step makes the weight loss process much easier. These are the fundamental steps to follow:
- Correct your thyroid medication dosage
- Reduce added sugars
- Base meals on vegetables and a protein source
- Consume more zinc and selenium
- Exercise regularly each week
- Trial the Autoimmune Protocol diet (if all else fails)
For much more detailed information on how to lose weight with hypothyroidism, see my article here.
Summary: Weight loss with hypothyroidism can be more difficult, so it’s important to take a planned, structured approach.
Where Can I Get More Info and Support?
The most reliable, objective information you can access will be from your endocrinologist, doctor and dietitian.
Online Resources
The online world is a bit different, and I recommend these first:
- NCBI Hypothyroidism
- NCBI Hashimoto’s disease
- Thyroid Change, a collaborative network of medical professionals and patients providing information.
Alternatively this website has a lot of science-based information in the Autoimmune section.
Online Peer Support
There are several great forums and online groups where Hashimoto’s patients interact and support one another.
Another individual’s personal experiences can be insightful and helpful, but be mindful that information shared on these platforms may not necessarily be accurate.
- Endocrine Web Hashimoto’s forum
- Underactive Thyroid Page Facebook group
- Underactive Thyroid Facebook group
- Reddit forum
- Dear Thyroid: A whimsical site for people to share their thyroid frustrations.

Very interesting. I admire your balanced and scientific approach. Minor thing though, from someone training to become a GP in Canada 1) there is no blood test to diagnose depression, we mostly look for anemia and diabetes. We use the age old method of talking to the person about stress and sleep and mood to screen for mood disorders/anxiety/insomnia. When someone is tired, both can coexist. 2) most hypothyroidism patients get managed by their family physician only, at least in Canada. The uncomplicated hashimoto is very common and straight forward. Referral to endocrinology is an option, but not the norm. 3) non severe osteoporosis, such as young adults? Sound like a typo. Like you said, the target for older people >65 is a higher TSH for that, and also cardiovascular Heath. 4) Anedoctally, I’ve never had patients complain of side effects of synthroid. I hope you don’t take this a critique, I rarely see ressources that consider both medecine and alternative treatment with an equally unbiased and critical eye.
Thanks for your feedback and suggestions Alexe, I will go over my wording in those sections 🙂
I had a reaction to syntroid or probably the fillers. It was a clear cause and effect. I took a low dose for a couple of years and was breaking out on my face and arms. I never had acne as a kid so just thought my turn. I quit take the rx for several years and it stopped. Once i went back on it for 1 year again with the breakouts. Painful on the face and scarring on the arms. I thought ok peri menopause. But when my dose was uped wow it got worse. I threw them away and found a doc willing to give me anything but syntroid. I ended up on tirosint and wowno more breakouts and finally after 4 years the arm scars are pretty much gone. When i had been complaining. . They gyno sent me to the derm then derm suggested the gyno.. well both were wrong. All kept saying no skin issues with synthroid. Wrong!
Haha wow i made a lot of typos! I see not a good idea thumb typing on a little screen. Oops 🙂
Alexe, your saying that Hashimoto’s is no big deal and super common–?! Are you kidding?
What is it with people in Med School? I have done more independent study than you will over the past quarter of a century, and I don’t pretend to have all of the answers – and you will hopefully learn that good physicians know to not use “always” and “never”.
I saw no reference to a blood test fr Depression, of course there is no such thing. YOU EVEN SPELLED “MEDICINE” WRONG! Well, now I have something to laugh about, so than you!
“The uncomplicated hashimoto is very common and straight forward [sic]”. – Go ask ten people who have this stupid thing if they agree that their life is not difficult because of this. Then come type that again, I dare you. You do seem to have the arrogant part of “being a doctor” down pat, hurray. You are not even a practicing physician, how can you say you have no patients who have had side effects from synthroid? Again I must stress that all people are different. We look the same in your medical books, but when you actually meet many human beings, you will see very different types of people who do well or not so well with medications. It took 4 years to get my meds right in my original illness – so please do not upset people who think they are “weird” or anything negative if they have side effects from medications.
I was dx’d, because of my last CBC, with Hypothyroidism and sent e-mail that said I have to take this medication for “probably [my] whole life”. It did not however, address that I have also had another illness for 25 years that requires food and meds throughout the day that have me so frustrated and clueless as to when in the world I can take my synthroid (I am also allergic to so many things, so the “syn” bit? SO SCARY!) So please, if you do become a Doctor? NEVER talk to patients the way you wrote here. we are all unique, we all matter, and a kind doctor can usually do WAY more for a patient than one who is arrogant and seems to be the last person who should have gone into a line of work in which he or she has such intimate care and knowledge of human beings.
I apologize to the wonderful person or people who run this site, it was a great help & comfort to me, and I am not as worried about how to continue my plant-based diet with my shiny new diagnosis. So you were a bright spot in my day and I was distracted by one icky comment. That was definitely not the plan initially! 🙂
Lovely put Sarah. Nothing more than arrogant nurses and doctors flare my hypothyroid.
Oh, thank you Sarah! You put into words my thoughts exactly. Having suffered for over 20 years with Hashimoto’s and being one in the 15% who are not “cured” of all symptoms by Synthroid, I can totally relate! Why is is that doctors think if they don’t understand or can’t prove something, it doesn’t exist!?! Does it ever occur to them that they don’t know everything?
Selenium is essential for conversion of T4 to T3. Research also indicates selenium could be essential in iodine absorption. Considering the importance of selenium and iodine to thyroid function/health, selenium could be an overlooked key to hypothyroidism: http://healthandscience.eu/index.php?option=com_content&view=article&id=738:selenium-and-iodine-make-a-strong-team-but-are-you-getting-enough-us&catid=20&lang=us&Itemid=374
Yes, there was a great section on selenium, I took notes as I read, ning especially the foods that are best to consume for this mineral. This site is so incredibly thorough and helpful, especially for those of us who were not even told in person that we have a potentially life-long illness that will always require meds.
Thank you very much for such useful information. I, personally suffer from hypothyrodism disease which was diagosed in 2010 with very severe conditions of heavy menstrual flow, with heavy blood clots, constant anaemia, dizziness, loss of eyebrow hair, dry skin, tiredness, lack of sleep, excessive hair loss, weight gain, memory problems, joint problems, mood swings but due so many hospital visits, reporting one problem today and the other another day, my doctor advised me to see an orthopaedic who finally found out I was suffering from the disease. But during that time, my joints were cracking excessively and were so painful. As I speak now, I seem fine, only that, since I am approaching menopause, I was given primolut to help stimulate some of the hormones since I was so anaemic. This treatment also caused the hormone to increase although it was later controlled. thank you so much for this useful information and for letting me it can be passed on. I will also look out for the same signs in my children.
this link make me very informative , so tank u very much !!!!!!!!!!!!!!!!!!
As a dietitian I have some serious concerns about this article, primarily with your advice to avoid gluten if a person suspects they may be intolerant or their levothyroxine is not working. In these cases I would always recommend seeing a doctor and being tested for Coeliac disease before commencing a gluten free diet. If a person has not had an adequate response to their levothyroxine dose they need further thyroid function tests and evaluation of their medication.
I also question this autoimmune protocol that you’re recommending whilst admitting it is not evidence-based. This diet sounds highly restrictive and without an evidence base I would weigh risks vs benefits on why it would be recommended to a patient with autoimmune hypothyroidism.
This article has been shared thousands of times yet I wonder how carefully the average Internet user would read it. You have described in detail some nutrients indicated for “thyroid health” and then only separately discussed the fact that a person whose thyroid is already damaged by autoimmune disease would not benefit from these in the same way that a person with a healthy thyroid would. Why does a person with hashimoto’s need zinc to produce TSH? Their body doesn’t respond to TSH appropriately. Of course zinc is part of a healthy diet but a casual internet reader would not understand this.
I practise in Europe and I’m sure their will be variations in the advice we give but I must admit I would not feel comfortable sharing this post with my patients or the general public for the reasons outlined above.
I am also a Dietitian, and agree with your comment about gluten. The person who came up with the idea of “gluten-intolerance” has since done more research and proved himself wrong. He retracted the findings of the gluten-intolerance, and so there is only celiac disease, which can be diagnosed by a doctor through blood tests.
I otherwise liked this article and found it helpful. I haven’t spent much time on hashimoto’s learning.
Hi Ana, gluten can cause more than just Celiac disease. One should be looking at a complete blood profile, food sensitivity tests, IGG, and Ige antibodies, a thorough hormone panel, and nutrigenomic testing to reveal the genetic mutations that can alter methylation, hormone production, DNA repair, as well as providing the enzymes so proteins can catalyze to other proteins. I have read at least 50 articles on Hashimotos, lots of good info, some bad, but a difficult thing to “cure”. My daughter suffers with this!
Great article. Thank you
I am a bit shocked about the thing you wrote about vitamine b12. It is more commen in people with already a auto immuum decease than you state here. The vitamine b12 needs to connect with a substance in your stomach, if your body attacts that substance or just dont make enough you can eat whatever you want rich on vitamine b12 but your body can not process it. I know i have hypothyroidism plus a malnutrition problem for vitamin b12. So please dont make it sound like it is nothing.
After 30 years finally my first vitamin b12 shot and a whole new world opened up to me. I did not have to sleep after work anymore, did not survive i lived. I finally knew what is normal and i was already so much better from being stable on my thyroid medicin.
For the rest a great explenation of thyroid problems
This was a decent general over view for the layman on basic thyroid and autoimmune. Most traditional endocrinologist rarely check Free T3 and I found in myself that I did not convert T4 thyroid well for a variety of reasons. As I am an Integrative Medicine physician, most of my patients have autoimmune of at least one or more systems, and I find it annoying when nutritionist focus on only celiac and fail to acknowledge the gluten irritation to the gut bacteria and how this triggers inflammatory stress (and often autoimmune) in the body. My clinical experience is that most people feel better off of gluten, end of story. Watch “what’s with wheat” Movie to see how we are causing inflammation and autoimmune. Blessings,
What’s with wheat and also What the health- very informative and a bit shocking documentaries. I highly recommend both.
I googled hypothyroidism as I was just given the diagnosis today by my doctor. Thank you for publishing such an informative article! It answered the many questions I had and explained why I hadn’t been feeling great! Also, what happens next.
Glad you found it helpful Ann 🙂
From a layman point of view, i so much appreciate the article, was able to gather more information on hypothyroidism.
Glad it helped Akinbola 🙂
I have Hashimoto’s. I no longer have my thyroid, it was surgically removed. I still take Synthroid. Would I still want to treat my system as if I still have a thyroid? I’m confused as to if I still have Hashiomoto’s or not?
Hi Stacye, Yes you need to take Synthroid because you don’t have a thyroid which means you need to take synthetic T4 hormone as a replacement.
Weight gainer supplements are crucial for muscle development and overall fitness.
There are numerous elements that help or hinder excess fat loss: some
of these are objective whilst others are completely personal or subjective.
According to CDC, Americans generally get enough of the proteins of their diet that is
required for their body plus they should target other nutrients that might help
their body functions.
For me Thyrolin works in the best way. I use it since some time already and I’m happy with results. How it’s gonna work on the long run? I’ll find out later. I buy it here: http://nplink.net/5zbalpML