MTHFR mutations are well-known genetic variations that can impact folate metabolism.
But there is a lot of confusion whether we should eat more or less folate.
This short article explains it in human terms.
Folate vs Folic Acid
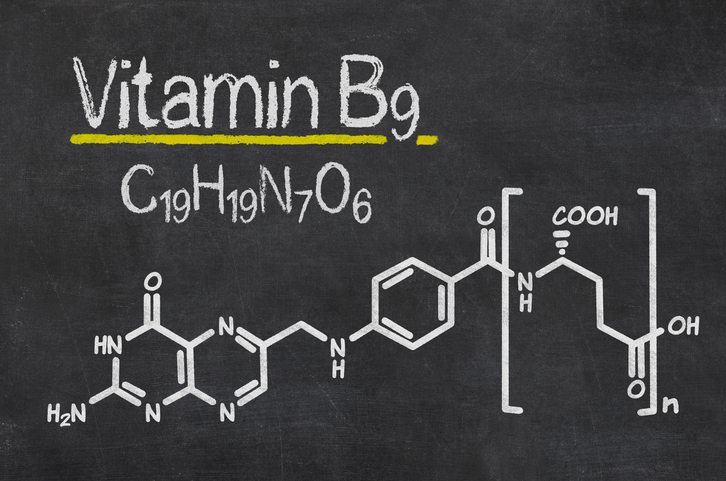
It’s fundamental to differentiate between folate and folic acid to understand the concept.
Firstly, both are similar types of vitamin B9 that we eat.
Folate refers to a family of different compounds that occur naturally in foods like leafy greens and legumes. This includes (1):
- Dihydrofolates
- Methylfolates
- Monoglutamyl folates
- Polyglutamyl folates.
The name folate even comes from the latin term “folium”, or what we call “foliage”.
Folic acid is one of the folate compounds and can be found naturally in foods too, in small amounts.
However, a “synthetic” version (it’s identical to natural folic acid) is also used in dietary supplements and added to foods, such as wheat flour.
High doses of folic acid are typically used to treat folate deficiency and other conditions, such as Neural Tube Defects and high homocysteine (2, 3).
The Noticeable Difference
The difference between folate and folic acid occurs during metabolism.
In particular, the process of converting them to the active form of folate, called L-methylfolate or 5-MTHF.
In this form, folate can be transported into cells and even across the blood-brain barrier.
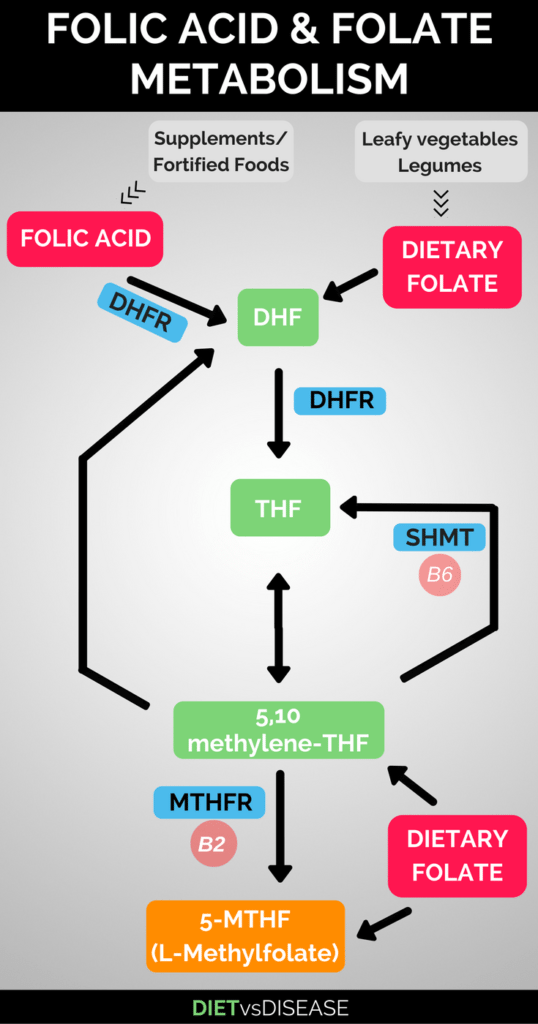
Click to enlarge.
The human body must do this conversion because it cannot use folic acid or folate in its basic form (chemical structure).
Folic acid we eat must always go through this entire sequence (above image), from top left corner to the bottom step, L-methylfolate. Notice the last step requires the MTHFR enzyme (blue box), produced by the MTHFR gene.
On the other hand, dietary folate can either start on the top right, corner or bypass the entire sequence completely…
This is because much of our dietary folate is already in the active form of L-methylfolate.
Summary: Most of the folate and folic acid we eat must be converted into the active form, known as L-methylfolate or 5-MTHF. However, some dietary folate is already in the active form when we eat it and therefore does not rely on MTHFR.
Some Natural Folate Is Already Methylated

As mentioned above, natural folate we eat comes in a variety of compounds.
This includes the active form of L-methylfolate.
That means we all need to eat more natural folate, MTHFR mutation or not.
I could not find a reliable source that lists the exact ratios, but many websites suggest these are the top food sources of L-methylfolate (methylated folate):
- Romaine (Cos) Lettuce
- Sprouted legumes (buckwheat, mung beans, chickpeas, etc)
- Broccoli and cauliflower
- Asparagus
- Kale and spinach
- Cabbage
- Fermented foods such as miso and kefir
- Berries like strawberries and raspberries
- Citrus fruits like oranges and grapefruits
Natural vs Supplemental L-Methylfolate

It’s clear that an individual with no methylation (MTHFR) issues could get adequate amounts of active folate from food alone.
Either directly as L-methylfolate or from other forms of folate (such as folic acid) that are converted during metabolism.
However, an individual with a “severe” MTHFR mutation would need to consume large quantities of these foods consistently to restore – perhaps to maintain – adequate folate levels.
For example, according to one germination study, 100 grams (almost 1 cup) of soybean sprouts contains about 0.8mg of total folate maximum. 100 grams of mungbean sprouts contained about 0.7mg total folate (4).
How much L-methylfolate was in those total folate amounts was not shown, but the average person just does not eat large amounts of those foods consistently.
The recommended starting dose of an L-methylfolate supplement is 0.5mg, but that is pure L-methylfolate. Prescription varieties start at a whopping 7mg, so there is certainly some use for supplementation.
Summary: Many foods naturally rich in folate already contain L-methylfolate. So the potentially harmful effects of an MTHFR mutation could be offset through a folate-rich diet in some scenarios. However, there is still a use for supplements.
What Is The Issue With Folic Acid?
Those with an MTHFR mutation may not produce enough MTHFR enzymes.
This means they may not consistently complete the final metabolic step that converts folic acid (and some folate) into the active form L-methylfolate.
MTHFR enzymes are necessary for this to happen (as well as vitamin B2).
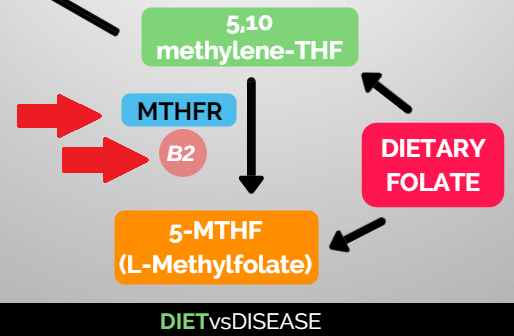
Therefore folic acid supplementation and foods fortified with folic acid may be largely ineffective in these people.
This could be a big issue if they have a folate deficiency, high homocysteine or are in the early stages of pregnancy and rely on folic acid.
Some suggest that unmetabolized folic acid can bind to folate receptors, effectively blocking access by L-methylfolate. I couldn’t find any studies to confirm this theory though.
Others also say that unmetabolized folic acid in the blood is uniquely harmful, but there’s no evidence of that in the medical literature. The body is simply getting rid of excess (a good thing), which goes from blood to kidneys, and then out through urine.
Summary: Those with an MTHFR mutation may not benefit from folic acid supplements or fortified foods. Theoretically a build-up of unmetabolized folic acid could be harmful, but it’s yet to be proven.
Everyone Should Eat More Natural Folate
Foods high in folate contain many different compounds, including L-methylfolate (methylated folate).
For this reason we should all aim to eat more, particularly leafy greens and sprouted legumes… as though we needed additional reasons to eat more vegetables.
If you have an MTHFR mutation and do not frequently eat the folate-rich foods mentioned above, you may be at risk for issues related to low folate.
This risk may be increased if you eat single sources of folic acid, such as folic acid supplements or fortified foods.


I am homozygous for the C677T variant. I have a question. What chemical is tested at the lab when one’s doctor orders a Folic Acid test? If one is taking no multivitamins and has a nuturient rich diet including many vegetables with L-15methylfolate, what would one expect the lab test to show? I consume several servings most days of folate rich foods. The lab test revealed that my Folic Acid level was just barely into the normal range. Any comments, information or advice would be greatly appreciated.
If one is homozygous for the C677T variant of the MTHFR gene and the lab test for folic acid is low despite a diet replete with foods having the natural L-methlyfolate, does that mean that a supplement would be in order? What does the lab test actually test for – L-methylfolate or an inactive form of folate?
I believe if you call a laboratory and ask for that information they will be happy to explain. I have made inquiries directly to the labs with no problem. Request for a lab technician. (They will also give you lower prices for their tests if you have no insurance, btw.)
All three of my children do not process folate and we found this out by having specific genetic testing done. We also found out which prescription drugs their bodies cannot process, which ones they should not take, etc. They each have a card with this information that they carry on them and can provide to the E.R. or to a doctor they have not seen previously. The test was covered by medical insurance.
Hello,
How do you know which prescriptions your kids can no longer take? Was there a test that determined this?
Ty.
Mary
What test do you refer to that indicated which drugs you and kids can’t take? Thank you
Hi Mary.
Do you know the specific tests that determined which prescription drugs your children cannot take. My daughter has MTHFR A1298c mutation and was tested deficient in folate among other nutrients. She sleeps all day and I am trying to find the right supplement combination for her. I wonder if her birth control or anziety medicine are playing a role in all of this.
Julie
The test is a general test for folate levels, it does not break it down into folic acid, folate and methylfolate since these levels are constantly changing as your body is always in dynamic activity, chemical conversions constantly going on.
Tests of conventional and organic foods show organic foods have higher nutrient levels. If you take a vitamin supplement you will do best with an organic whole food multivitamin. Go low and slow with vitamins. Your body gets bit crazy if you give it too much at once. It starts trying to get rid of all the chemicals stored in your tissues and blood which it could not excrete before and you will feel awful.
Plants have not just methylfolate, but also folic acid and folate forms in them. The folate levels shown for plants are measurements of total folate levels, meaning all three. Vitamin levels in conventional foods are lower than organically grown foods. If you still need to take a vitamin supplement stick with an organic whole food multivitamin supplement. Go low and slow with vitamins as too much will make you feel sick, when the body gets vitamins levels it is not used to having it starts pulling out of tissues the chemicals it stored there which it was unable to excrete before when it was low on vitamins. Your body uses vitamins to make the hormones and enzymes it uses to detoxify Chemicals and get them out through either urine and/ or BM. Of course those hormones and enzymes are used in other functions throughout the body also.
I have similar questions. Also, could a normal or high result for the serum test for B12 disguise a deficiency of methylcobalamin?
When I had my B vitamins levels checked my Folate levels were high and my doctor said it was because I wasn’t absorbing it properly and told me I needed to take methlyfolate. So yes, I think the same could be said for B12 and methlycobalamin.
From what I have read from biologists and within the natural/alternative, you can have a normal serum test for any mineral or vitamin and still be deficient, as these substances leave the blood and reside elsewhere like in flesh , fat, and organs… and can be measured for their usability in urine or feces. So many practitioners in the holistic/natural/alternative fields (not in the convention medical system) will test you for all three specimens – blood, urine, feces – to determine how your body is using them or not. I do not know if this can be done for all though. A Functional Medicine doctor or practitioner , or Naturopathic Physician, or other holistic practioners, and some Chiropractors, perform these. Call any of these to find out.
The same is true with your thyroid hormones. Several tests need to be performed and read together to determine the condition of your thyroids – not many doctors are familiar with this. In addition, your adrenals have an affect on your thyroids as well like cortisol levels… all working with the pineal and pituitary glands – it’s a whole network like a symphony. These are better understood by Naturopathic Physicians, as in natural medicine the training is in the whole system, not parts.
Also if you have metal toxicity – mercury, aluminum, lead, etc – which abound in food, dental, vaccines, medications, environment – these can displace nutrients and keep the body from using nutrients . One thorough testing is Quicksilver which uses hair, urine, and feces to determine levels and then a chelating substance combines with other natural chelations to draw and safely bond to excess and pull out via your intestines. Other forms do the work via your kidneys which could adversely affect them if you are toxic laden heavily such as having amalgams. These are DMSA, EDTA (not recommended) and others.
Conventional Medical doctors are not trained in Nutrition nor in chelating heavy metals – (nor are they trained in how vaccines work, btw) in medical school (some only have 12 to 23 hours of random Nutrition) ….you can ask any. They are trained solely in synthetic medicine targeting targets to force-fix a component to not create a symptom. They have no training in natural knowledge. So they are incapable of giving proper advice in Nutrition or diets. It is only now that they even consider giving advice on diet, it used to be “oh that is not important… you get everything you need from food.” – yeah…. fake, toxic foods full of sugars and nutritionless carbohydrates. Not only that, overindulgence in some foods as well as medications, can displace or inhibit nutrients. So someone trained in the balance of these and how systems are affected by their lack will be more helpful in healing. Like those mentioned in above comment. Conventional medical doctors that you see using natural methods train themselves in natural knowledge which exists outside of their medical training box.
Medicine has its place and is great at emergencies, surgery, (and synthetic for these purposes are very good for immediate conditions, though naturals are still needed in the ER to also save lives) and diagnostic technology… but they fail at healing and regeneration (healing is not depending on synthetics for life, and when those synthetics produce secondary conditions and diseases).
I’m curious about the food sources for L-methylfolate because I do want to get things from my diet instead of pills.
I’m curious why no meat sources were mentioned? I notice you link another site, but I’m still curious as to your thoughts on it?
From what I have found Liver is one of the foods that is just packed full of all the B vitamins. It also should be B-Vitamins that are in an active form that our body can use. Since it’s coming from an animal source, from what I understand it’s going to be the active version since the animal’s body already converted it.
Thoughts? Information and such doesn’t have one source I can quote. It’s been something I have found/learned over the course of a few weeks and speaking with my doctor as well (she focuses on genetic mutations in relationship to depression and such)
I do not eat liver for two reasons, first it tastes awful to me and second the liver is one of the organs involved in detoxifying the chemicals and poisons in your body.
They feed animals all sorts of nasty things they are not allowed to feed humans. I stopped eating non-organic meats when I found out they feed them garbage and even read where they found them feeding cows ground concrete.
Also, 80 percent of antibiotics are fed to animals to make them grow and get weight faster. Having an impaired methylation system due to the MTHFR gene mutation I avoid all unnecessary and avoidable chemical exposures.
I guess if you like the taste of liver you could eat organic liver if you could find it. It still yucks me out that it’s main function is waste disposal.
If there is a “natural” form of folic acid , as opposed to the synthetic folic acid, that occurs in food BESIDES FOLATE form…… then the synthetic should not be named “folic acid”, because for a synthetic to be patented it MUST be molecularly unique. A synthetic form is usually made by deleting an electron or “mirroring” the structure (like reversing it) which no longer is IDENTICAL to the natural one. Which is the whole purpose of developing a “copied” version to be able to patent it and own. So the synthetic can never be said to be identical or react identically because it simply is not. Otherwise millions would not be spent to turn the natural derivative to a synthetic – if it were to remain natural or original. To say it is identical then the patent is a fraud…….So….. what is the “natural” form of “folic acid” mentioned here – or was naming it folic acid a mistake? There can’t be 2 “folic acid” and each be different. My understanding is that “folate” is natural and “folic acid” is the synthetic – no 3rd one exists.
Show me the patent for Folic Acid…
He says it himself, here’s the quote from this page:
Folic acid is one of the folate compounds and can be found naturally in foods too, in small amounts.
“Folic acid is one of the folate compounds and can be found naturally in foods too, in small amounts.
However, a “synthetic” version (it’s identical to natural folic acid) is also used in dietary supplements and added to foods, such as wheat flour.”
As you know, synthetic means man-made which has to be patented.
Synthetic is a substance derived from a naturally occurring source whose molecules have been man manipulated chemically to produce a “similar” molecule but different in structure which cannot be fount in nature. Nature recognizes it partially. This difference makes the molecule act differently and when interacting with other natural molecules, and it is responsible for adverse effects that are stronger and unpredictable which means it is causing some damage.
I have not spent the time to search for a patent, as it may be time consuming, but understand that many patents become universally available after a certain time, especially in medicine. Generic medicines are an example which are further copies from proprietary synthetics, allowing other makers to make the drug available and more cheaply. That is why doctors may recommend only the original version of the drug – because of those differences that produce another or slightly another result.
Patents are legal licenses the government gives to a product developer which are only good for 25 years. Folic acid is out of patent for over 30 years now.
The problem is not only with folic acid. Folic acid is constantly referred to since it is the one vitamin the government and physicians constantly tell women they need to take if they get pregnant. The problem is with all chemical vitamins, in fact all chemicals, if you have the MTHFR gene mutation you have trouble not only with turning chemical vitamins into bioidentical forms your body uses to make hormones and enzymes, your body has trouble turning Synthroid ( which is T4 ) into the T3 form it uses to function. That is why so many us have Hypothyroidism and we still have low thyroid symptoms when taking Synthroid. We need to take Cytomel ( T3 ) to get rid of the low thyroid symptoms, but most physicians do not know this. All medicines have the same problem in us, we need the bioidentical form for them to be effective.
People with just one copy of the MTHFR gene mutation have less of a problem since their methylation system runs at 60-70 percent efficiency. I have two copies, so Synthroid is almost useless for me, I have to take Cytomel.
cytomel is synthetic also?
Cytomel (liothyronine sodium) is a synthetic thyroid hormone used to treat hypothyroidism (low thyroid hormone).i understand it is synthetic t3, is that still ok for homozygous mthfr. ive been getting the wrong thing for a while and my total t3 is still low.
Yes, Cytomel is synthetic T3. Synthroid is synthetic T4. The thyroid gland makes mostly T4 and a small amount of T3, the body depends on the methylation system to convert T4 into T3 as it is needed over the day’s 24 hours. So if you have a MTHFR gene mutation you will have problems, with two copies you may hardly convert any T4 to T3 when you need it. If you go down to Robin’s November 06, 2017 post, you will be able to read what I posted today about the MTHFR genes, the methylation system, and thyroid medicine. It explains how I was able to go from hypothyroid to having normal thyroid blood levels .
Any new drug does not have to be patented. You can decide not to patent a drug if you want to, it is just the process the government put in place so a company could recoup the money they spent developing the drug by not having competition for 25 years.
Agreed
My husband is just newly diagnosed. I need help in knowing what foods he can and cannot eat.
I would read labels and avoid products that are enriched with folic acid. I was surprised that my egg beaters contained folic acid. Pasta, cereals and white flour are also enriched
Your husband can safely eat grass-fed meats and organic fruits and vegetables. Anything processed could contain folic acid.
All wheat flour contains folic acid, they are required by law to add it to wheat flour. The idea was to replace the methylfolate that is removed in the processing of the grain into flour. They use folic acid because it is a very stable chemical. If they added methylfolate back to the flour then the flour would go rancid fast because the processing also removes the antioxidant VItamin E which would keep the methylfolate from degrading. So they add folic acid to the flour instead and call it “enriched” .
Pretty much any food product that has been processed and comes in a box or bag could contain added folic acid. You can check the ingredient list on the package, but in the case of flour only “flour” or “enriched flour” will be listed.
It is also best to purchase organic fruits and vegetables because the same methylation system that converts chemical vitamins into bioidentical form, is part of the body’s detoxification system. With the MTHFR gene mutation if you have one copy of the gene your body is 60-80 percent efficient, so you would better off than a person who has two copies. A person with two copies has a methylation system that works at only 10-20 percent.
Pesticides in non-organic foods will build up in the body along with every other chemical you take in by eating, drinking, get on your skin, or inhale. Is it any wonder that we who have MTHFR gene mutation get sick and develop so many medical problems?
Everyone with one copy, or even two copies, should also be checked for the SUOX, CBS, MMTR, MTR , COMET, MOA-A, and MOA-B gene variations as these also reduce the efficiency of the methylation system.
Approximately 40-60 percent of people have the gene mutation, you might consider being tested since you may need to avoid folic acid as well. And it is much easier to follow the proper MTHFR diet when everyone in the house is eating the same way.
It is interesting to note that 98 percent of people with Autism have the MTHFR gene mutation. A recent study has found that when the mother has high blood levels of folic acid the baby will be born with Autism. In children who are not born autistic, but have the MTHFR gene mutation, they can become autistic. This happened to my son when he had his six month old immunizations. The high mercury level in the immunization caused him to have a seizure. The brain damage made him autistic.
Hope this information helps, if you have any questions you can email me at aelxahill@gmail.com
He can eat whatever he wants. He should take a daily supplement for mthfr (just look on Amazon). This contains the methylated form of folic acid. Just don’t take vitamins or supplements with folic acid.
Eat whatever you want if having symptoms of Mthfr???
Yes, you can eat whatever you want. However, you will develop high blood levels of every chemical you eat ( and drink, inhale, and get on your skin). The MTHFR gene mutation impairs the methylation system and the methylation system not only converts chemical vitamins into forms the body uses to make hormones and enzymes. It also is the system that processes and detoxifies every single chemical our bodies absorb.
I eat only organic food and grass-fed and organic meats, and drink water I filter myself. The hardest part was giving up perfume, makeup, nail polish, room fragrances, and anything scented. It made a huge difference, I was able to discontinue three of my prescription medications by doing this.
Hello, I have just been diagnosed as having the homozygous c677t mthfr mutation. The doctor that had me tested immediately put me on folic acid. From what I’ve been reading this is a bad thing, right? If it’s the wrong thing to do, what symptoms might I experience or expect? I have been taking it for about a week now, and to be honest, I feel perfectly terrible. My joints, muscles are already affected by osteo-arthritis, and since beginning this med, it has felt much worse. Dizziness, which I have had spells with have become worse. Is this related?
I would appreciate any information, especially from sources which I can cite to the physician. Thank you!
Yes this is a very, very bad thing! I hope you are no longer taking the folic acid. Good grief, what kind of stupid idiot is your physician? Get yourself another physician, unless he or she is teachable this person could cause you great harm!
With the MTHFR gene mutation you CAN NOT convert folic acid into methylfolate that your body can use. Your body needs bioidentical vitamins to make the hormones and enzymes your body needs to function.
Also every chemical you eat, inhale, and get on your skin will make you worse, because the methylation system that processes and detoxifies chemicals is not functioning well.
With one copy of the MTHFR gene mutation it only works at 60-70 percent efficiency, and with two copies it is down to 10- 20 percent. So medicines can be a problem, I have two copies and have a list of 30 medicines I can not take. I either throw them up, or get an asthma attack, or get sick as a dog from them.
For sources you go to NIH.gov and search using MTHFR as the search word. If you can read and understand the studies it will make you ill to see how harmful folic acid is to people with the MTHFR gene mutation.
I have heterogeneous A1298C mutation.
A few years ago I was on pregnancy multivitamins with folic acid and my folate levels were still very low. I went to a naturopath and she put me on folinic acid instead and my levels improved. Since then I have had the mutation confirmed and also low thyroid. My doctor has prescribed Pure Natal by orthoplex which has both folic acid and L-5-MTHF plus mediherb Thyadren support.
You only mention folate and folic acid, not folinic acid and synthetic L-5-MTHF. Is there any research on these 2 synthetic forms?
I would like to get off these and onto a wholefood solution. I have been to a nutritionist, however they have only given me a list of suggested foods to eat more of. You mentioned the amounts of total folate in 2 food types. Is there anywhere to find how much is in all of the main folate rich foods and what the conversation is from total folate to the usable form? Also, is there any information on how much of the activated form people with different mutations need? Ie how much of what foods need to be eaten instead of supplements?
You have a naturopathic physician so they should be teachable. In the last five years alot of good new studies on the MTHFR gene mutations have come out, so physicians are not aware of the serious dangers of folic acid in our foods.
Here are the facts. About 40- 60 percent of people have one or more MTHFR mutations.
These mutations make it almost impossible to convert enough chemical vitamins into bioidentical forms that the body uses to make the hormones and enzymes the body needs to function correctly.
Blood test levels of vitamins will be high if you take chemical vitamins but most of the vitamins in circulation will be in unusable, unconverted forms which your body can not use.
Because the methylation system also is the system that processes and detoxifies every chemical your body comes in contact with, people with the MTHFR gene mutation will almost always have high levels of lead, mercury, copper, and other metals and chemicals that are harmful to the body. For some reason zinc levels will be low, impairing wound healing. You need to avoid chemicals as much as possible, because once they get inside your body it is hard for the body to get them out.
Organic food and totally grass-fed meats ( not finished with grain) are the best diet for everyone with the MTHFR gene mutations. Avoid processed foods in packages, buy foods in glass, as foods in plastic and cans absorb chemicals from the package.
Folate in plants are in three forms, folic acid, folate and methylfolate. The levels of all three vary from plant to plant, but the list will not tell you how much of each form is in each plant. They will only give the total folate level.
Organic whole food vitamins are best, the only stores that carry them are stores like Whole Foods and health food stores. These vitamins are low dose and rarely have more than the RDA levels of vitamins in them.
This is best for the following reason, once your body gets vitamins it can use, it will go to town making the hormones and enzymes it has been low on for so long. This sudden flow will cause over-methylation and you will feel extremely sick. Your body will be trying to get rid of all the bad chemicals stored in your tissues and blood, so you have to go low and slow with vitamins.
You are also fortunate in that you have only one copy of the A1298C gene, this means your methylation system is 60- 70 percent efficient and so your body is able to use alot of the folinic acid. I have two copies and can only convert 10-20 percent so I have to use methylfolate.
Today on the news they were reporting that 50 percent of adults over 18 years old were developing allergies. It a sudden crisis, any they are recommending people eat fresh whole foods and decrease use of processed food products.
Gee, 40-60 percent of people have the MTHFR gene mutation. Anyone else see the connection?
It is 7:16 PM on Wednesday September 27, 2017 here in the USA. This site must not be in the US. Hmmm, 14 hours difference, is the owner in Australia?
Hi Alexa
I’m thankful to read the research you’ve done. I also have 2 copies of MTHFR and continue to struggle with energy. I do however have additional conditions which effect my energy as well. Though I’m in the medical field, and have done some research myself, you’ve shared some important information I hadn’t thought of including the removal of lotions, shampoos and the frightening thought of no makeup…..maybe I’ll cut that last until I find an alternative. Thank you very much for your time in sharing.
I really understand about the makeup, just make sure you get the least toxic you can afford. I was amazed to find lipstick, especially makeup made in China, can still contain lead compounds! I use one that is made by Burt’s Bees, and I use his vanilla lipbalms. A woman just wants to look her best. Aelxa
I have been dealing with this problem forever, so I know what you mean about having other conditions. I started working as a Respiratory Therapist in 1975. We used a liquid sterilizing solution called Codex, which is a gluteraldehyde related to formaldehyde, and it was kept in a 30 gallon trash can in our office. By 1982 I was diagnosed with Asthma. Since then I have been diagnosed with Chemical Sensitivities, Chronic Fatigue Syndrome, Fibromyalgia, Hypothyroidism, Adult-onset Growth Hormone Deficiency, Osteo and Rheumatoid Arthritis, Chronic Pain Syndrome, High Blood Pressure, Hyperparathyroidism ( Parathyroidectomy 2016), and the latest Irregular Heartbeat(origin unknown) .
So I know about having no energy and not feeling well. It can make life an interesting challenge at times. But I just keep trucking along, my son keeps me young,
That should read Cidex, not Codex. Silly machine keeps “correcting” my spelling.
Energy! I have found that if I am very low on energy if I take 400mg of acetyl L-Carnitine and 400mg of Alpha Lipoic Acid about 30 minutes later I will feel fine and no longer. You can get the acetyl l-Carnitine 400mg with alpha Lipoic acid 200mg capsules, then I add an alpha lipoic acid 200mg capsule and take them together. It helps immensely with energy.
HI Alexa,
I’ve been tested for the MTHFR genetic mutation and the results show C677T/C677T, two copies of the same variant. I am fairly confused about this situation, as I wade through all the information listed on this site, as to what is the correct approach to this problem, dietary, as well as supplemetary. I do have high levels of lead contamination in the body. I had been undergoing edta chelation therapy for the lead removal, but was getting nowhere with the removal, thus showing that there was a source of contamination for lead in my system. I had been drinking coffee for 8 yrs. from some ceramic mugs made in China., when it finally occurred to me to test a mug for Pb and Cd (another high element that I tested for), I discovered finally the source of the contaminants. After eliminating these mugs and all ceramics from my life, I continued with intensive chelation therapy for a number of months, only to be disappointed with the results, as the Pb levels were not dropping like I thought they should. The physician who owns and manages the chelation clinic, then had me tested for the MTHFR gene mutation, which showed up. She then put me on a regime of supplements. So I am taking the Methyl-Guard product from THORNE, 1 cap 2X daily. I assume you are familiar with the ingredients in the Thorne product. I have also been taking a product from RHP, their Advanced Nerve Support Formula for about 7 yrs. in order to ease the effects of neuropathy which I experienced from Metoproloi (blood pressure) and a lower back surgery in 2010. This product contains per 2 caps: D3 (100IU); K2 MK7 (100mcg; , B1, Benfotiminine (166 mcg); B2 (4mg); B6, PyroHCL (4mg); Folic acid, methyltetrahydrofolic acid (200mcg); B12, Methylcobalamin (2000 mcg); Tumeric; Acetyl L-carnitine; and R-alpha Lipoic acid.
I am 69 yrs. of age, overweight by about 30 #, with metabolic syndrome (pre-diabeties). Lately I have felt fatigued and somewhat light-heated and slightly vertigoic(?). I do eat most of everything you have listed in terms of veggies and will switch to your take of grass-fed organic meats. I had discontinued the chelation out of frustration, but would sure love to eliminate Pb & Cd from my body (this would probably drop the BP), so I am beginning chelation again soon.
I am writing for an opinion as to whether it seems as if I am on the right track concerning the MTHFR issue in your opinion and also if you can add by suggestion any other nutritional or other practices to my life. Thanks in advance, Bill Keller
Hi Bill. I have the same two copies, so like me, your methylation system is only working at 10-20 percent efficiency.
The huge problem with lead and other heavy metals, the molecule takes alot of enzymes to detoxify it and excrete it out of the body, the molecular bonds for lead, cadmium, copper, etc are such that they bind to our tissues faster and harder than the magnesium, lithium ,etc that we do need for good functioning. When you do the chelation again make certain they keep a close eye on your calcium, magnesium, zinc, and lithium levels (which we tend to be low on anyway with the methylation system not working well) because chelation will strip your body of all minerals and metals indiscriminately. Make your physician aware that we tend to have low levels because of the MTHFR gene mutations, low magnesium especially can be a cause of high blood pressure. You will tend to lose the minerals you need before any lead or cadmium comes out, so my physician back in 1989 stopped using it in patients who had my symptoms. He switched to using Vitamin C IVs with added B Vitamins, they were much easier on the body, and worked just as well in getting the lead and mercury out of the body. The IVs also had the side effect of decreasing my pain and increasing my energy levels. That and taking powdered Vitamin C added in my drinking water and sipping water all day worked very well for me and my son. (He has one copy of C667T and had high lead levels).
Vitamin C helps the methylation system work better and is not as traumatic to the body .
I am learning more organic biochemistry in the last three weeks than I would like to have to, biochemistry was never my favorite subject. All those chemical reactions dependent on enzymes and hormones, levels of which were basically unknowns. Physics and inorganic chemistry are so much more simple.
I am familiar with Thorne. With what I have learned about the methylation system I am looking for supplements that have the least amounts of “inactive” ingredients in them. So I no longer stay with one particular brand. Most important is that the vitamins and minerals are in bioavailable forms and have few other ingredients in them. Every added chemical is another item putting strain on the methylation system, and working only at 10-20 percent I find I feel worse when I am exposed to alot of chemicals. Going into a department store can make my brain foggy for days, and I find days later when it is working better that I bought all sorts of stuff I did not really need or want.
I hope that folic acid which you listed is not in the Advanced formula, if it is you really should not take it. We really have to avoid all chemical vitamins and other chemicals as much as possible , getting by on a system only working at 10 percent is challenging. I use glass plates, glasses, even glass jars to drink from to avoid any possible chemicals or metals, even liquid foods like spaghetti sauce and mustard. I threw away all the liquid foods I had open that were not in glass, the rest I gave to the food bank. I have been feeling so much better in the last three weeks since I got serious about avoiding chemicals. I had not realized how impaired my body was, with the methylation system functioning so poorly at only 10 percent, 20 if I was lucky.
I used to be diabetic with an A1C of 12, my physicians kept saying I had to be eating foods I had not written down when I was carefully measuring and weighing everything before it went in my mouth. Then I found that even minute amounts of maltodextrin would raise my blood sugar 40 points! The tiny amount in a stevia packet I put in my tea raised my blood sugar 40 points, and the packet stated it had zero calories in it. Now I use SweetLeaf, and my A1C is 5. I found six of the supplements had maltodextrin in them, and when I eliminated them too, I was no longer diabetic. Corn also raises my blood sugar high, even one kernel will do what maltodextrin does to me. I looked into it and found corn is so contaminated with chemicals and pesticides, I do not understand how they can sell it as food. The government just keeps raising the “allowable” limits. Giving up corn is harder for me than giving up wheat. I adore corn fresh, corn muffins, grits, corn chips, whatever way you make corn I love it. I had a favorite corn muffin recipe I made with jalapeño peppers and fresh corn in them that I miss so bad. It’s been 5 months since I gave up corn and have lost forty pounds.
Regarding your neuropathy, I had carpal tunnel syndrome in both hands. The right hand was so bad, the neurologist wanted to do surgery immediately as I was in danger of losing the hand, the pain was like cold ice, freezing cold like I had never felt before in my life. My pain management physician has a device from Germany called Hakomed. They put pads on my hands, like the ones they use with TENS units, with one 45 minute the pain was down from a 10 to a 3. After three 45 minute treatments the pain and numbness all went away. Now whenever I start to feel any numbness, it happens about every 10 months, I get one or two treatments and the pain and numbness goes away again. If you can find someone in your area with a Hakomed machine who is knowledgeable in it’s use, they may be able to help relieve your neuropathy.
I have been using two products, one called Niagen that I take in the morning and another called Sirutan that I take before bed, both made by HPN which have helped my energy immensely, and I have also added reduced glutathione which helps the methylation system detoxify the body. I hope you find this information helpful
Aelxa
I have just learned that reduced glutathione does not survive stomach acid, only acetyl glutathione or liposomal glutathione are absorbed intact for the body to use. Going to switch from reduced glutathione to acetyl glutathione , since the liposomal form is fragile. This means it needs to be stored carefully and used fairly soon after it is manufactured, whereas the acetyl form is much less fragile.
Lead in products from China continues to be a problem, ceramics and paint on children’s toys are often contaminated with lead. The US does not require automatic testing of imported items, and China has no laws against using lead in paint and glazes. Another source of high lead (Pb) and high copper blood levels can be copper water pipes, from acidic water. They used a high lead metal composition to solder the piping together. Even after they made it illegal, they let plumbers continue using the lead-based solder they had on hand instead of making them turn the stuff in. And many cities have old lead water supply pipes and if the correct chemicals are not added the lead will leach into the water. Cadmium is used in galvanizing iron pipes, so if you have water pipes made of galvanized iron that could be the source of the cadmium in your body. Plastic piping will eliminate the cadmium, lead, and copper, but add chemicals to the water as they leach out. In my opinion, water supply pipes which supply water for drinking and cooking should be plain iron. If iron leaches from piping it is the least harmful element to our bodies. I use a Pur filter to reduce metals and chemicals in my drinking water, but there no great answer to the problem. Distilled water is not a great solution since we get most of our minerals from our drinking water, and chemicals from the plastic jug it comes in leaches into. You have to do just the best you can, with what you have available.
4 months ago, I was diagnosed with MTHFR mutation (2 snps). I have Hashimotos, my adrenal glands are working about 20%, and I also have struggled for about 3 years with chronic kidney infections. I quit even going to the doctor because I was getting no where and they were constantly telling me my blood results were “normal.” As for the kidney infections, I just got frustrated they wouldn’t go away with several rounds of antibiotics and started drinking a ton of cranberry juice and taking capsules. OH! Did I mention I am also Multi-drug resistant? That’s why I couldn’t get rid of the infection.
I reached a point that I couldn’t get out of bed. I was exhausted all the time. We already ate organic, grass-fed, and mostly vegetarian with lots of natural greens for the folate (I learned about that after a miscarriage before my last child was born). I couldn’t get going though. I was in a bad place physically and my brain just wouldn’t shut down. I wanted to do more. I wanted to be my typical active self, but couldn’t. I finally reached out to a naturopath. He has really helped change my life from the path it was going. After some blood work, urinalysis, saliva, and DNA testing, he was able to diagnose all the above and then some. What no one has yet mentioned, is that when your methylation isn’t happening, your neurotransmitters aren’t functioning properly either. This has now caused a chemical depression. Ask me if I’m depressed and I’ll tell you NO. True answer, yes. 8 of my 9 neurotransmitters are in the below normal range. My naturopath wondered how I wasn’t suicidal at that point. Well, I thank a strong-will and God for that. I knew something was physically and chemically wrong, but just didn’t know what. Now I do.
Anyway, I am now gluten-free, soy-free, dairy-free, caffeine-free, corn-free, tomato-free, & peanut-free. The hardest thing to give up was pasta and bread. I have found a few alternatives that stay within my new lifestyle, but I think the best thing for anyone dealing with all this is to realize that it’s about our all-around health. How did our ancestors eat? How did they ever make it in life? I’m sure it wasn’t on fries and cheeseburgers. It was eating off the land. Just look around and see all the glorious foods the grow and realize that is the way we were meant to eat. I want to feel good. I want to be more energetic. I want to be a healthy mother and wife. I don’t hardly eat out because it’s discouraging the crap that is served. I got eggs and potatoes at a major chain restaurant recently, thinking, “Can’t go wrong with eggs…” WRONG! They were fake eggs. It was made from some sort of powder or whatever. I was sick within minutes. So, the little sacrifice of not eating out but eating what is natural and good is worth all of that to me. And remember, what works for one of us doesn’t work for all of us. All of our bodies methylize and metabolize differently.
If you don’t like your doctor’s answers, find another one. Find one who knows what MTHFR is and how to treat it. I am taking a supplement called Methyl-B12 along with about 7 other remedies/supplements. It can be frustrating taking all these supplements and taking them around eating times and not eating those foods that can have affects on them; but then I think about where I was a few months ago and push on. I don’t want to be back in that place.
I hope others who are searching for answers and understanding find that healing is about the whole health. It isn’t just the folate/folic acid. You have to start treating your whole health because it’s all intertwined.
Hi Kristina, I’m glad you’ve found a way of life that helps you and is conducive to your health. Keep it up and good luck! 🙂
Hi Kristina,
I know how you feel, I have two copies also so my methylation system only works at 10-20 percent. I only have two antibiotics that I can take, so I drink lots of water and avoid anything that can cause an infection.
Did your doctor check your lithium level? Our bodies naturally use lithium and when lithium levels are low, as is common in people with the MTHFR mutations, depression is the usual result. I take 300mcg of lithium a day and no longer severely depressed. This dose is what we normally need and is a very tiny, tiny, tiny fraction of the dose they use in psychiatric illnesses. In fact, I get it over the counter because it is not a prescription item at this strength.
My recent MTHFR test indicates = Compound heterozygous A1298C + C677T.
Homosystene levels and B12 results are fine but blood test indicates toxic levels of B6. B6 levels slowly coming down due to detox diet and natural liver detox capsules plus I stopped taking my B Complex vitamins.
My concern is not knowing how the B6 got so high in the first place. I was taking a B complex (150% daily B6) for about 6 months but this was around a year –after– my pain started so I doubt it was the cause of the toxicity. I’ve had severe neuropathy type pain in my feet and legs for over 2 years undiagnosed and unable to work since. With the B6 results we are assuming it’s the reason for my pain. Neurologist says he’s not sure if the nerve damage in my feet is permanent or not being it went undiagnosed for so long. As the B6 levels drop my pain remains. Feels like electricity running through my feet all day and night. The only thing that seems to help is heat from a bath or heating pad.
Do you think my MTHFR mutation has anything to do with the B6 toxicity in my blood ? Also, you mentioned the the Compound Heterozygous A1298C + C677T is the most severe or “at risk” of enzyme function. Can you shed some more light on that subject or recommend a book / website where I can get more information ? I appreciate your time. Cheryl G.
You have two copies of the MTHFR gene mutations, with two copies your methylation system is only working at 10-20 percent efficiency. This means your body can not convert folic acid through the multiple conversions to make it into L-methylfolate that the body can use. What no one mentions is that the same process is used in converting almost all vitamins, including B12.
This means if your blood test levels of B12 are normal or high, and you have symptoms of. B12 deficiency, then the B12 in your blood is in unconverted B12 forms that your body’s cells can not use. At the same time it can not excrete the useless B12 forms either since the methylation system is also part of the body’s detox system. You will need to educate your doctor about this.
The neuropathy you are experiencing is indicative of the B12 in your blood being unconverted. If it were converted you would not have the neuropathy. Unless you are also diabetic, high blood sugar levels also cause the neuropathy you are complaining of.
Doctors do not understand this since most get only a few hours of nutrition in medical school, and almost nothing about gene mutations and vitamin conversion difficuties. Only in the last 10 years has the information about gene mutations and the problems they cause in regard to vitamins even been discovered.
The high B6 is due to the same problem, the best form of B6 to take is Pyridoxine, because it can enter the cells, where it is then turned into the active form, pyridoxal-5-phosphate or P5P. If you take B6 as P5P it will stay in the bloodstream since P5P can not enter cells, and you will wind up with toxic high B6 blood test results. (This is from a research article in BMC. Pediatrics 2011 “Effect of a Vitamin/Mineral Supplement On Children and Adults with Autism”. Note: It has been found that 98 percent of children and adults with Autism have the MTHFR mutations.)
Anytime you have normal or high levels of a vitamin, and you are showing symptoms of a vitamin deficiency, just assume the vitamin is in unconverted forms, and that you are actually suffering from a vitamin deficiency. In your case you probably need to be taking B12 in the hydroxocobalamin form as an injection. I have two copies of the MTHFR gene mutations, and this is the form I have to take.
If you get the correct B12 form soon enough, then there is a possibility of reversing the neuropathy, if you wait too long then the condition will be permanent .
I suggest you make an appointment with your doctor today, and make him aware of what the normal B12 blood level really means.
The website I get my information from is the US Government’s National Institutes of Health. http://www.nih.gov. PubMed site.
Meanwhile, clams have the highest levels of B12 with 80 mcg per 100 grams, followed by beef liver with 26-58 mcg per 100 grams , beef and lamb 1-3 mcg per 100 grams, eggs are 1-2.5 mcg per 100 grams,chicken trace- 1 mcg per 100 grams. But you have to chew them well, because the B12 absorption process starts with the TCN1 enzyme in your mouth’s saliva. If the B12 is not attached to the TCN1 enzyme, then it will not survive the acid in your stomach.
It is also best to eat your B12 containing animal foods in small amounts of 3-4 ounces every 4-6 hours apart. This is because a study found that you can only absorb a small amount of B12 no matter how how high the dose of B12 you take. They believe it is because your body can only make a minute amount of intrinsic factor every 4-6 hours. Intrinsic factor is made in the small intestine and is the next enzyme B12 hooks up to after the B12 gets through the stomach and then unhooks from the TCN1.
So chew your animal foods very well, and make them organic and grass-fed to avoid the nasty chemicals that we have trouble detoxing due to the MTHFR gene mutations.
I am homozygous for C677T and recent lab results showed low (below normal) levels of folic acid and B12. My doctor gave me a Cyancobalimin b12 shot. Will this type work for those with MTHFR mutations?
My doctor recommended I take a folic acid supplement, but I’m hesitant to do so given what I’ve read about problems being able to convert folic acid. Is there a specific type of supplement I should be taking? From what I’ve read, increasing folic acid in foods like spinach should help, but won’t be enough. Appreciate any advice.
Hi Cheryl, I’m not sure if it effects your B6 levels.
It’s mainly to do with homocysteines. Please see this part of the article; Other research confirms that both homozygous C677T (T677T) and compound heterozygous (C677T + A1298C) are linked with higher homocysteine concentrations and greater risk of heart disease (http://www.ncbi.nlm.nih.gov/pubmed/18204887, http://www.nejm.org/doi/full/10.1056/NEJM200104123441517).
Hi I have had mthfr for over 10 years now. I know very little about it. I was diagnosed after throwing saddle PE’s. My Dr said little about it and I have asked many different Drs and get no advice. I’m trying to read and learn on my own. I have a question about how it effects weight gain and if eating my folate rich food will help with this. I workout 4 to 5 Times a week watch my carb intake but no results. Does mthfr effect this?
Eating folate rich foods may help but it depends.
The MTHFR gene mutations affect the body’s methlyation system, one copy and the system works at 60-70% efficiency and with two copies it only functions at 10-20%.
The methlyation system function is to do detoxification of chemicals and heavy metals, conversion of almost all vitamins into methyl-forms which the body can use, also it deals with the hormones in our bodies.
Hypothyroidism is common in people with the MTHFR gene mutations because of the impaired methlyation system, it is supposed to convert the T4 the thyroid makes into T3, if the thyroid is not making enough T3. We need a specific balance of T4 and T3. over the entire 24 day period. The form of thyroid medicine most doctors prescribe is Synthroid which the methlyation system cannot convert into both T4 and T3 when impaired by the MTHFR gene mutations. We need bioidentical forms the body can use, without them you get weight gain. The thyroid makes T4 well, T3 not so well since it depends on the methylation system to change the T4 into T3 AS NEEDED by the body as you go through your day. This means that anything that impairs the methylation system will cause a decrease in T4 to T3 conversion, not enough T3 and the body’s metabolism slows down and you store calories eaten as fat. You cannot exercise enough to overcome the low T3 level, unless you burn more calories than you eat. But if you do not eat enough calories, then the body’s metabolism system senses you are starving and will slow down even further to conserve what calories you do have in storage. This is a no-win situation, the only fix is to get T3, since the lack of T3 is causing the problem.
In my case I have a doctor who listens, and I take Synthroid(T4) and Cytomel(T3) before I go to sleep, then Cytomel every 8 hours thereafter. The benefits have been that 1) my depression, that no medication has helped, is now almost completely gone. 2) my sleep is deep and solid, and my dreams are great with no more bad dreams at all. Before I was waking every 2-3 hours that I was aware of (sleep study showed me waking every 40 minutes minimum. 3) My stomach where I carry my weight is getting smaller, and I weigh the same because I am finally building muscle instead of storing fat. Low Thyroid is the biggest contributer to depression, thyroid is needed in the brain to keep your brain’s neurotransmitters functioning properly. If you want to know more there is a book that I have not read yet, but have a copy of, that is written by an endocrinologist Ridha Arem, MD called “The Thyroid Solution ” , make certain that you get the newest edition which is the Third Edition that was published in 2017. I made my changes from reading his professional paper published at an Endocrinology conference, but I will be reading his book that I just got on Friday.
Now, will eating your greens help, the answer is yes IF you eat greens that are organic. Why? Because every chemical we take in our body has to be detoxified by the methylation system, and if the body is busy working to detoxify the pesticides and other various chemicals in and on conventional veggies, it will take care of that first. After it makes certain we will not die from poisons, then it will work on converting vitamins and hormones, etc. This is why I tell people to eat organic and grass-fed meats and organic veggies, and get the chemicals out of your house. The methylation system will keep you alive the best it can, but if you throw too much cra_ at it then it can only can only do a cr_ppy job of it. The methylation system has too many functions to do and in our modern polluted society it has a hard enough job, add in MTHFR gene mutations and we are the first to get sick and we get sicker faster, and die early. Why? Because physicians are only being taught that the MTHFR gene mutations affects the conversion of Folic Acid and to give lots of folate instead , if they are taught what the methylation system does in converting Folic Acid, detoxifying chemicals, converting hormones, etc then the information must slip out of their brains while they are still in medical school.
The better you treat your body, then the better it will work to keep you healthy and happy. Remember, “Better Living Through Chemistry” was a DuPont Company marketing slogan, chemicals are NOT you friends—they will make you sick.
That should have read ” We need a specific balance of T4and T3 over the entire 24 hours of the day period.”
Also, the usual time a patient is told to take their thyroid medicine is in the morning before eating. The problem with this is that fiber will block the absorption of thyroid medicine. And since it takes four hours for your body to totally absorb the thyroid medicine, you would have to wait almost four hours in the morning to eat your breakfast, since breakfast is the most fiber heavy meal of the day.
I am taking the same amount of Synthroid and Cytomel as before, just no longer in the morning and the Cytomel every 8 hours, ( instead of taking 2 Cytomel with the Synthroid in the morning and one Cytomel in the afternoon as my endocrinologist had me doing before. ) Now my blood thyroid levels are all mid-range which is perfect, instead of being low thyroid as I was before. Same medicine just different timing made all the difference.
I also want to add that when you get any blood tests done you should get the printed results, DO NOT accept the doctor saying “Your results are normal “. Why do I say this? Because back in 1998 I got very sick and my primary physician told me all my results were normal. I knew something was seriously wrong and insisted on a copy of the results from the hospital lab. It turned out that my IGF- 1 was only 26 and normal levels range from 70 to 298. This freaked me out because I knew from my studies that the level of 70 was for a person who was 100 years old ( 298 is the level at puberty). When I pointed out the result was only 26, the doctor told me “That’s OK, it’s only a little low”. At that point I knew he was totally clueless when it came to Endocrinology, so I immediately went to my endocrinologist and when he saw the 26 result, the endocrinologist admitted me to the hospital right away. He ordered a special IV challenge test the same day that confirmed my pituitary gland was hardly functioning at all and I was put on daily growth hormone injections that I inject myself. Without enough growth hormone your heart will start to fail and then you die, and my heart was already showing signs of failing.
I wound up with thyroid problems six weeks ago because my endocrinologist was retiring and only working two days a week, so he transferred me to one of the new endocrinologist on staff. This brilliant new doctor discontinued my Cytomel (T3) medication because she said at my age “the levels should be lower “. And three days later I was in my primarycare physician’s office because I was unable to stop crying, my hair was falling out, and I felt like I was dying. My primary physician was horrified and immediately put me back on the Cytomel, and even increased it from the two tablets a day I had been taking before it was stopped, up to three tablets daily.
In a way I should thank the new endocrinologist because, due to her messing me up, I got online and looked into studies dealing with thyroid. Needless to say, I made adjustments to my medicine based on what I learned (with my primary physician’s OK), and my blood thyroid levels are all mid-range and I feel great. I also asked my old endocrinologist to take me back and thank heavens he is taking me back!
The last time I saw the new endocrinologist I told her I did not care if she was unhappy with me being back on the Cytomel, because I would be damned if I would be sick and falling apart just to make her happy. And that her job was to make me well, not to make me so sick that I was unable to function. It seems once you get over 50, it is not only hard to get a job, but physicians start treating you like you are a waste of space and you need to die to make room for all the younger people.
So be proactive people, the life you save may very well be your own. End of rant.
I have one copy of A1298C. I’ve been taking The Synergy Company’s organic whole food vitamins and their other supplements for a year now. They don’t contain any synthetic ingredients, and are fully organic. The multi has 800mg of folate.
We eat only grass finished meats, organic proteins, organic produce, almost no sugar, no grains, legumes, (Paleo Diet) We exercise regularly, have zero toxins in the home, a large air purifier, and drink R/O water.
I also extensively tested for thyroid issues – did the full panel on my own, not the TSH test offered by doctors. Results were normal thyroid numbers, EXCEPT for Reverse T3, which was slightly high. (Tested that one twice to be sure.) I have normal homocysteine numbers, my blood pressure and cholesterol are fine, etc.
However, I’m still tired all the time, and cannot lose weight.
My main concerns are:
1. Whether I should take a methylated B-complex supplement in addition to the other supplements I’m already taking.
2. Many of the folate-rich vegetables contain vitamin K as well. Is there such a thing as eating too much Vitamin K? (As an older woman, I have a concern about blood clots.)
I wonder if an additional Methylated B supplement would help with the fatigue and excess weight. I cannot see a ND or Functional MD now, or do more lab tests, due to budget constraints.
Any advice or comments are greatly appreciated
Hi Robin, MTHFR does not effect weight gain to my knowledge. I can’t see how that mutation would effect your weight.
May I please ask, I have both mutation for C677t and A1298C. I also suffer from Hashimotos and therefore the fatigue is unbearable and I am not certain what I can do. My TPO AB are over 600 with no success in lowering them at all in 2 yrs. I have tried injections of B12 or B Complex but they don’t seem to give me any extra energy. Perhaps because of the MTHFR mutations? I have read that I would need methylfolate. Now although there are oral supplements out there, could I take an injection of B12 and and injection of folic acid instead?? Thankyou for any information.
Hi Shaunte, I don’t recommend injecting B12 or folic acid. And you should speak to your doctor about that.
hello how are you, if you take anything supplemental make sure it is in its converted stage (folate opposed to folic acid) (b12 in methyl form) very few doctors are educated on this matter I am going to see a geneticist that understands mthfr, don’t listen to doctors that are not sure exactly it could be dangerous if untreated or mistreated
Just because you have an MTHFR mutation(s) doesn’t mean eating extra folate will help. Sometimes, depending upon whether your system is overmethylating or undermethylating, folate with have positive or deleterious effects. It is not wise to suggest ALL people with MTHFR to load up on folate. In undermethylators the excess folate can speed up the SERT function, that is the serotonin transporter. When SERT is speeded up, it takes the serotonin out of circulation and the result is depression. I have inadvertently done this without supplementation, only with whole fresh foods. I would advise caution in high consumption of folate rich foods or methylfolate supplementation for people with MTHFR C677T. In some people folate helps with depression, in others it can make it worse.