Around 1 in 100 people have celiac disease worldwide (1).
The only known treatment is a strict gluten-free diet, which is not easy to do.
This article takes a detailed look at managing celiac disease and how to do a gluten-free diet.
What is Celiac Disease?
Celiac disease (also called coeliac disease) is an autoimmune condition that can damage the small intestine.
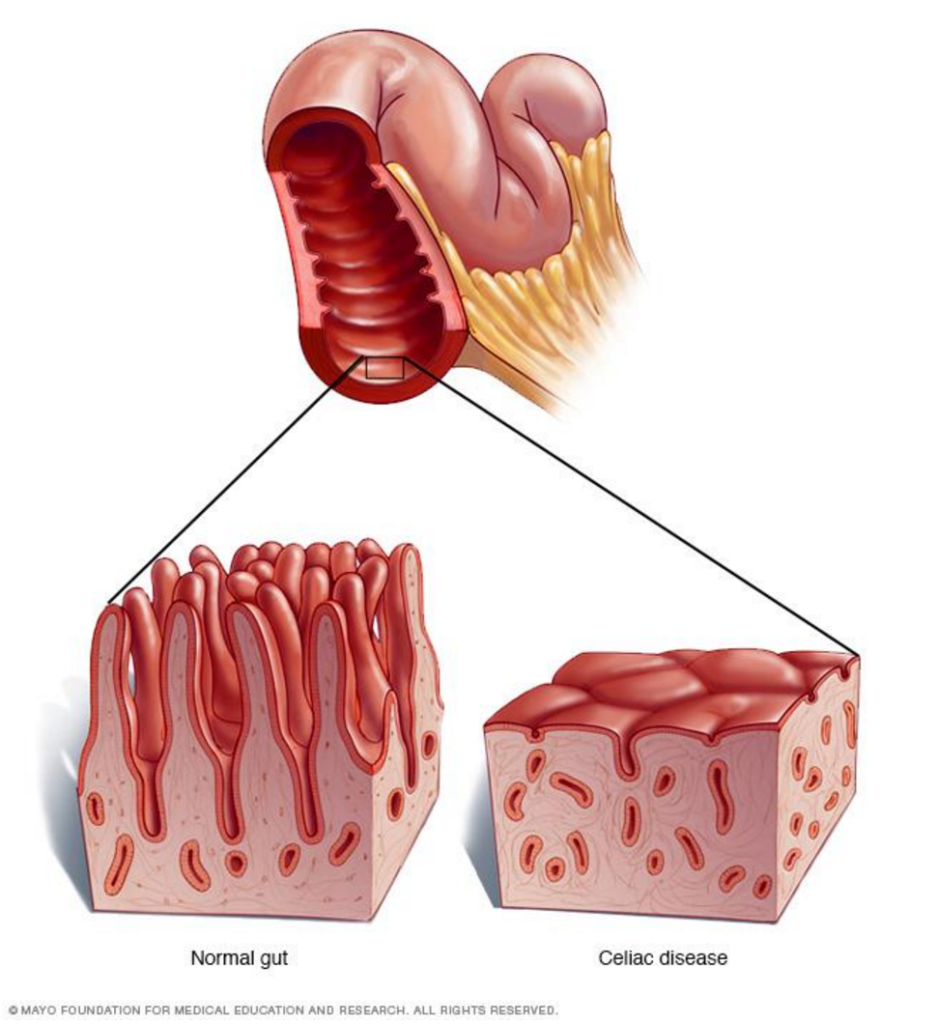
Specifically, the small intestine has many small projections (villi) along it, which help absorb nutrients from food. In celiac disease these are damaged and nutrients can’t be absorbed properly.
Normal villi vs. celiac disease villi in the small intestine. Image source. Click to enlarge.
Celiac disease causes the immune system to see gluten as a threat, attacking both the gluten and the villi of the small intestine. Therefore, people with celiac disease need to avoid foods containing gluten.
Gluten is a naturally occurring protein that gives bread its elasticity. It’s found in:
- Wheat
- Rye
- Barley
- Any products derived from these ingredients.
Celiac disease vs gluten intolerance
Celiac disease should not be confused with gluten intolerance.
Also known as non-celiac gluten sensitivity (NCGS), gluten intolerance is now formally recognised in the scientific community.
Gluten intolerant individuals can tolerate small amounts of gluten up to a certain threshold, whereas celiacs cannot tolerate any gluten at all.
Don’t self-diagnose though… see your doctor to rule out celiac disease first.
Summary: Celiac disease is a genetic condition that causes damage to the gut lining when gluten is eaten. Gluten is a protein found in wheat, rye and barley. Make sure to rule out celiac disease before considering gluten intolerance.
Celiac Disease Symptoms

Celiac disease affects many organs.
It can sometimes be confused with irritable bowel syndrome (IBS), as they share similar symptoms.
- Diarrhea
- Abdominal pain
- Bloating
- Fatigue
- Iron deficiency anemia (low red blood cell count)
- Depression
- Anxiety
- Weight loss
- Vitamin deficiencies
- Skin rash (dermatitis herpetiformis)
- White, yellow or brown spots on teeth
- Dementia
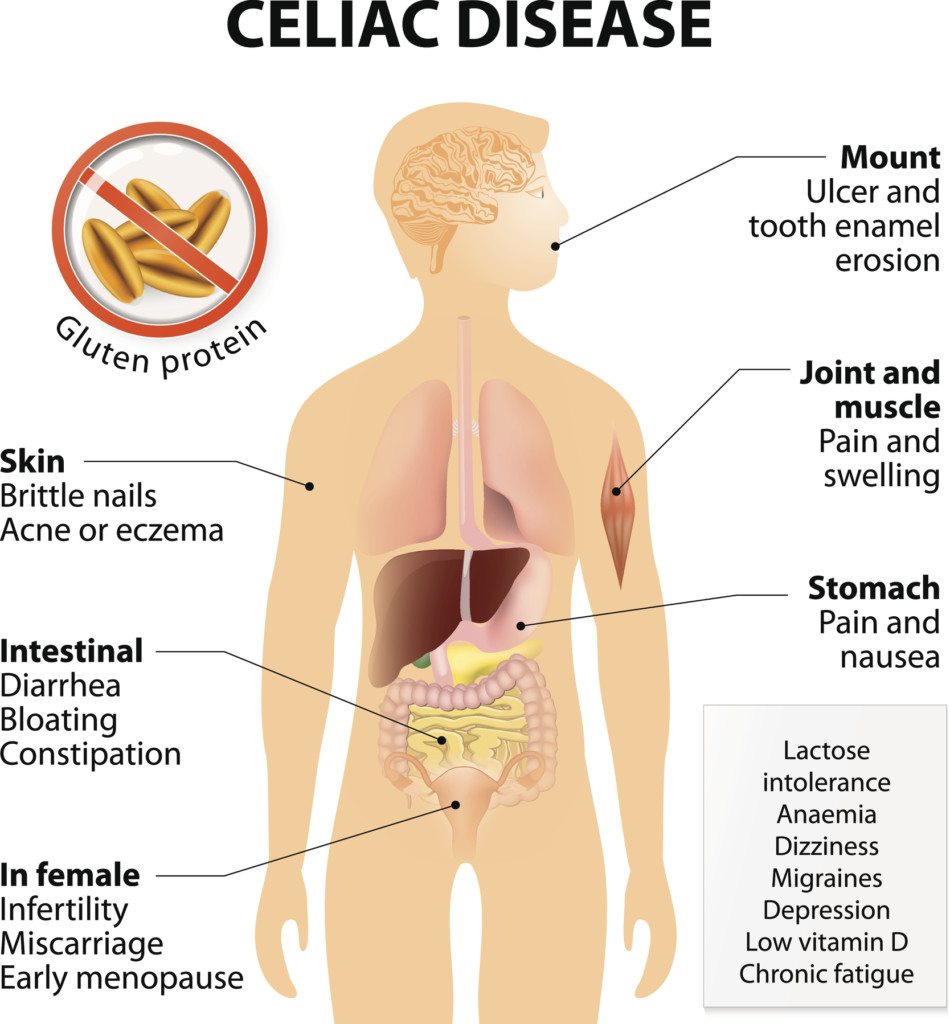
Celiac disease symptoms. Click to enlarge.
Summary: Celiac disease has a wide range of symptoms that can impact many organs. Many are similar to what you would experience with IBS.
Long-Term Complications
If poorly managed, celiac disease can cause a host of serious health problems.
Many of these stem from malabsorption of nutrients in the gut.
Complications include (2):
- Malnutrition – which can cause delayed growth in children
- Problems with bone density – from malabsorption of calcium and vitamin D
- Reproductive issues – infertility and miscarriage
- Lactose intolerance – can be caused by damage to the small bowel
- Cancer – non-Hodgkin’s lymphoma, small bowel adenocarcinoma
- Neurological issues – seizures and neuropathy
Fortunately, a strict gluten-free diet can help reduce the risk of these complications.
Summary: Celiac disease can cause many serious health problems if left unmanaged.
Celiac Disease Testing and Diagnosis
Should you get tested?
Celiac disease is difficult to diagnose, which is why it’s commonly under-diagnosed (3).
Symptoms can vary a lot between individuals, and some may have no obvious symptoms at all.
Conditions including Type 1 diabetes and hypothyroidism can also put you in the high risk category (3).
Additionally, family history plays a part:
- If your parent or sibling has celiac disease, you have a higher risk and it’s wise to get tested, particularly if you have symptoms.
- Likewise, if you have celiac disease, your child has a higher risk. Children that have parents with celiac disease are often tested from 2-3 years old.
Testing for celiac disease
For blood tests to work you must be eating gluten beforehand for several weeks.
This is often referred to as a gluten challenge.
With gluten back in the diet, testing for celiac disease may involve:
- A blood test to check for high antibodies produced when your body sees gluten. Antibodies are proteins that your immune system uses to protect your body from threats.
- A positive blood test needs to be confirmed by a small bowel biopsy. A few small pieces of your bowel are taken and examined under a microscope to check for damage. The test can take less than 30 minutes and you are usually put to sleep.
- People that have already removed gluten from their diet may be unwilling to undertake the gluten challenge. In this case, gene testing, for the HLADQ2 or HLADQ8 genes, may be considered (4).
If you don’t have these genes it’s unlikely you have celiac disease. In saying that, having the genes doesn’t mean you have the disease. The only way to be sure is from the small bowel biopsy.
Testing more than once
Unfortunately, celiac disease can develop at any time.
The trigger for the disease is a complex relationship between genetics, the environment and the immune system.
High risk individuals may need repeat testing. This is particularly important for children, as the tests can be unreliable until they have been eating gluten for some time.
Summary: High risk individuals should be tested for celiac disease, which usually involves a blood test and small bowel biopsy. As celiac disease can develop at any time, repeat testing is needed.
The Celiac Disease Diet: Gluten-Free

A gluten-free celiac disease diet is the only effective diet option.
Although we call it gluten-free, it’s near impossible to remove 100% of gluten. The exact safe amount is unknown, but less than 10 mg per day has been suggested (5).
In the US, Europe and Canada, a food must have less than 20 ppm (parts per million) of gluten to be labelled gluten-free (4).
Australia is stricter, requiring foods to have ‘no detectable gluten’.
List of celiac disease foods to avoid
Aside from actual grains of wheat, rye and barley, gluten can hide in many everyday foods.
Watch out for these gluten sources:
- Wheat described by different names– some are durum, kamut, semolina, faro, bulgar and spelt
- Triticale, which is a crossbreed of wheat and rye
- Malt
- Brewer’s yeast
- Packaged foods not labelled gluten free like pasta, cookies, cereals and breadcrumbs
- Marinades and sauces
- Starch or dextrin
- Beer
As you can see, learning to read food labels is important when on a celiac disease diet.
What are gluten-free foods?

Many foods are naturally gluten free and help to create a balanced and nutritious celiac disease diet.
These include:
- Meat
- Fruits and vegetables
- Eggs
- Nuts and legumes
- Dairy products including milk
- Fats and oils
- Naturally gluten free grains such as rice, corn, millet and sorghum
- Pseudo-cereals like amaranth, buckwheat and quinoa
- Foods labelled ‘gluten free’
What about oats?
Technically oats are naturally gluten-free.
However, they are often cross-contaminated from other grains during the harvesting or packaging process.
For this reason certified gluten-free oats exist, which are processed and packaged on separate equipment from other grains.
Additionally, some celiacs may react to a unique protein in oats called Avenin, which is structurally similar to gluten (4, 6).
It’s best to work with your doctor and dietitian if you’d like to include oats in your celiac disease diet.
Is a gluten-free diet healthy?
Following a healthy, balanced gluten-free diet is difficult but not impossible.
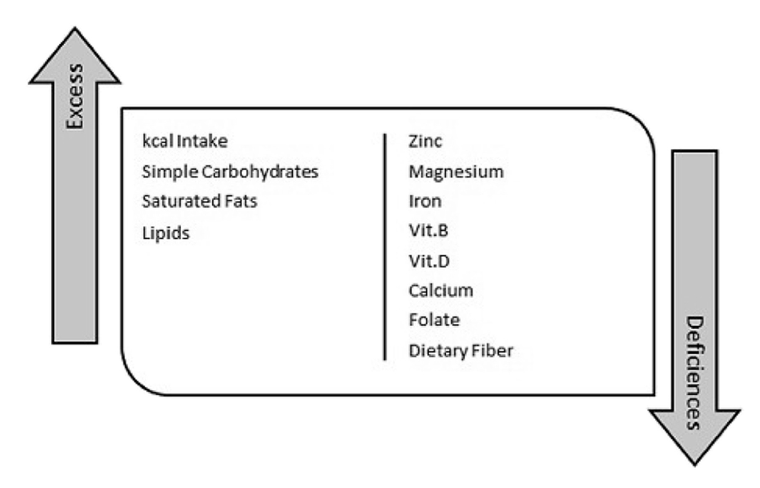
A recent study found several common problems (shown in the image below) for someone following a gluten-free diet.
Image source. Click to enlarge.
The main concern is nutrient deficiencies that can develop over time, including zinc, magnesium, iron and folate deficiency.
Symptom improvement
A gluten-free celiac diet relieves symptoms and allows the small intestine to heal.
The length of time this takes can vary between individuals, from several months to years (2).
One study of 215 patients showed that symptoms of diarrhea took four weeks on average to improve after starting a gluten-free diet (7).
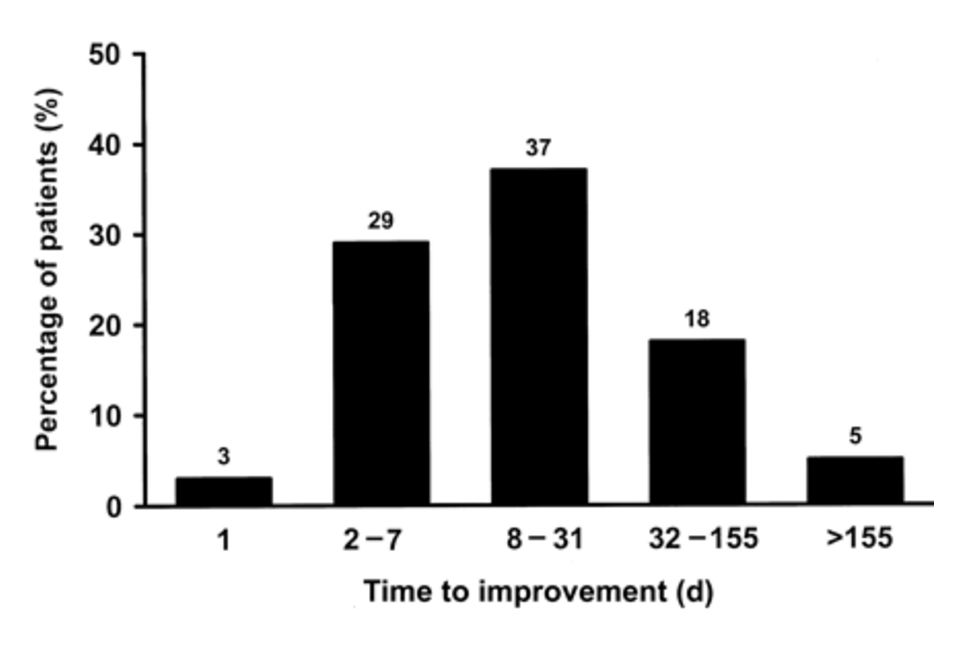
Your doctor will monitor symptoms and blood tests regularly to check for improvements.
Cross-contamination
A strict gluten-free diet includes avoiding cross-contamination from all foods containing gluten.
Something as simple as sharing butter with family members who eat regular bread containing gluten could be harming your intestine, even if you don’t feel symptoms.
Here are some great tips on how to avoid cross-contamination.
Summary: Celiac disease is managed with a gluten-free diet, which allows the small intestine to gradually heal and symptoms to resolve. Gluten can be hidden in many food sources and cross-contamination must be avoided.
Can a Gluten-Free Celiac Disease Diet Fail?

If symptoms remain on a gluten-free diet there are a few things to consider.
There may be some hidden sources of gluten in your diet, even though you think it’s gluten-free.
Other reasons could be confusing symptoms with another condition like lactose intolerance, fructose malabsorption, irritable bowel syndrome (IBS) or small intestinal bacterial overgrowth (SIBO).
This is why it’s important to work with a dietitian where possible.
If damage to the small intestine remains after a strict gluten-free diet for 6-12 months, it may be refractory celiac disease.
About 1-2% of those with celiac disease have this condition, which is typically treated with immunosuppressants or steroids (2).
Summary: If symptoms persist on a gluten-free diet, working with a dietitian can help rule out gluten contamination or other conditions with similar symptoms. Refractory celiac disease could also be an issue.
Non-Food Sources of Gluten to Avoid

Aside from celiac disease foods, gluten can also be found in non-food sources including:
- lipsticks
- herbal supplements
- vitamin and mineral supplements
- play-dough
- medications
It’s best to check the label or contact the manufacturer.
Some medications may contain gluten, often in the form of wheat starch. Talk to your doctor about appropriate medications if you are unsure.
Summary: Possible non-food sources of gluten include lipsticks, supplements and medication.
Where to Find More Information

Your doctor, dietitian or gastroenterologist will be the best source of reliable information about celiac disease and a proper celiac disease diet.
If you’d like to read more, these online resources are a great start:
To interact with others that have celiac disease or for some light-hearted humour check out the Reddit forum. Just know that not all information in online forums is accurate.
As celiac disease shares symptoms with other gastrointestinal conditions, you may also want to also read one of our guides about Irritable Bowel Syndrome (IBS) or Small Intestinal Bacterial Overgrowth (SIBO) to understand the differences.
What Can And Can’t I Eat On This Diet?
Often it’s easiest to start with this giant list I’ve made of what foods to eat, and what foods to avoid when following a low FODMAP diet.
It’s based on the latest published FODMAPs data (1, 2, 3, 4, 5).
Print or save to your phone to use as a quick-reference guide when shopping or cooking. I’ve attempted to list foods in both US and UK/Aus names, with US first.
I’ve included a screenshot of the first page below. But the full PDF is 4 pages and suitable for printing. To download it simply tap the box below and it will then be emailed straight to you – it’s free!



I have dh, a form of celiacs and even after being diagnosed in January, 6 months ago, my skin will still break out in rashes. It seems like I’m doing everything right but it is very difficult to find food every where I go. There is always a chance of gluten ingredients, even on gluten free menus and I’m not sure how sensitive I am to gluten or if my skin also has a reaction to other foods. It’s questionable weather some salads are even gluten free. This article was very helpful though!
Thank you for the article. I have become very discouraged because after three months on a gluten-free diet I still have many symptoms. Although they have decreased about 50% I felt like something more must be wrong. After reading the article I’ve learned that it can take a long time from something to disappear and my body to heal. The damage that was done to my organs I’m told was expensive and I had been malnourished for a long time. So again thank you for the article and look forward to doing follow-up.
Please pardon my typos I was doing voice to text. So read between the lines because I could not find an edit button. Thanks so much!
I have had a celiac diagnosis for 14 yrs now. I am not a medical professional but can lend you my experience.
STOP eating gluten free packaged food. All of your symptoms, acne, gas/bloating, etc will disappear. I didn’t know this and just replaced all of my old food habits of gf pasta, bread etc. it’s all garbage. I eat veggies, meat and fruit. Just found out this week dec2018 that most of the coffee produced in the k-cups have gluten in their coffee!!! WTH? No wonder my stomach hurts all of the time. I’m furious!!!
Celiac is an auto immune disease and once it starts, it begins to help develop other autoimmune issues begin. I am now allergic to ALL grains, including rice. I am also now developing an allergy to wine. It’s the yeast that forms in it. Yes …all wine. I have eczema on my face and forehead every time I drink wine. It takes three days to go away.
This is not a fad diet. It is my life.
Hi DCI thanks for your feedback and your experience. Hopefully it helps newly diagnosed coeliacs. 🙂
Is Celiac Disease associated with hairloss
I have Collagenous Colitis or CC. It’s a microscopic colitis. I experienced hair loss and was devastated. Plus I had diarrhea, fatigue, and weight loss. When I lived in Austin, I was told it was Pancreatic Malnourishment Syndrome. It’s a disease where you’re not putting out enzymes to break down your food. Sounded good to me because my father had it along with being a Type 1 Diabetic, just like me. Like Father, Like Daughter. I was put on Creon and my hair flourished and got thick. The thickest ever! Felt like Farrah Fawcett and I got looks. Then the diarrhea came back. I was going through my Mom’s stroke, Death and my brother’s abusive behavior against me. I was living in the bathroom, sick, and fatigued. I increased my Creon, but the diarrhea still continued. Went to a doctor in Savannah, and I did not like him. I was sick. I finally went to Mayo in Jacksonville, and they diagnosed me with Collagenous Colitis. I had been misdiagnosed for 5 years, even though I still think I have it at times. I still take a low dosage of CREON because it makes me feel better and my hair is getting thicker. A WOMAN AND HER HAIR! Hair is important and it’s our crowning glory.