Psoriasis is complex to treat.
In fact, Physician Paul Bechet once said it’s “the antidote to a dermatologist’s ego” (1).
It’s an autoimmune disease that causes chronic pain and itching that can severely impact on quality of life.
Many foods and supplements are rumored to help with psoriasis treatment. But does research support these claims?
This article examines the evidence surrounding the relationship between diet and psoriasis.
What is Psoriasis and Its Symptoms?
Psoriasis is a chronic autoimmune disease that causes patches of skin to become inflamed and scaly.
It affects up to 4% of the world’s population (2).
Symptoms occur in flares, and include itching, pain, and skin lesions. Psoriasis may also cause pitted fingernails and toenails, as well as mouth sores.
There are six types of psoriasis. Each type causes a distinctive rash:
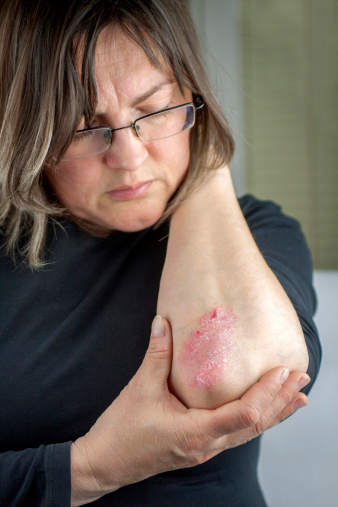
- Plaque psoriasis causes a rash that is red at the base with silver scales on top. It accounts for 90% of all psoriasis cases (3).
- Guttate psoriasis causes clusters of red, drop-shaped lesions.
- Inverse psoriasis affects the genitals and underarms and the area under the breasts. It causes a smooth, red rash that is often worsened by heat and friction.
- Pustular psoriasis is often triggered by environmental stressors. It causes pus-filled blisters on the skin.
- Erythrodermic psoriasis is a potentially serious medical condition characterized by a red, scaly rash all over the body.
- Psoriatic arthritis causes skin lesions, as well as joint pain and inflammation.
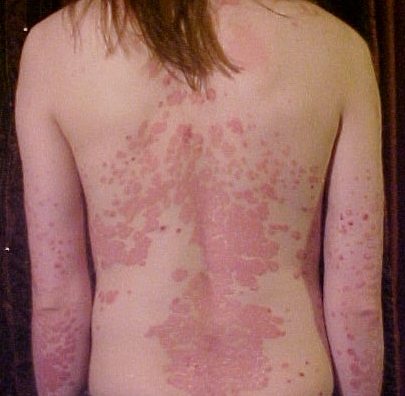
Plaque psoriasis. Image source.
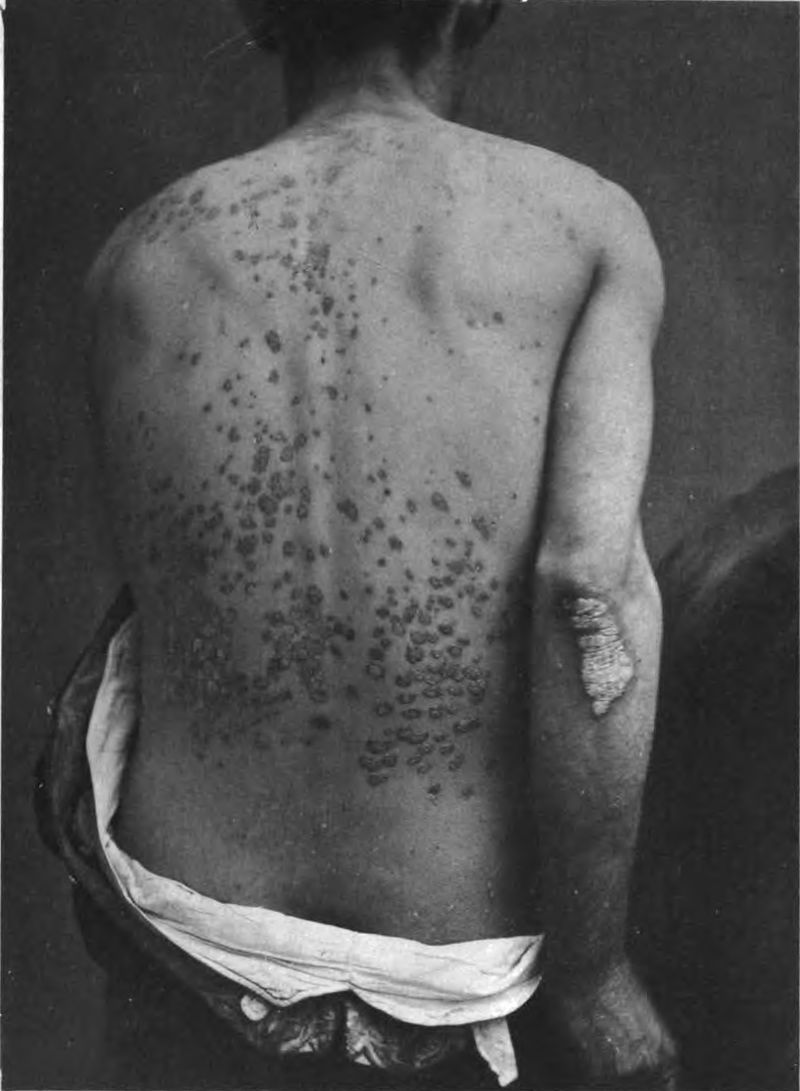
Guttate psoriasis. Image source.
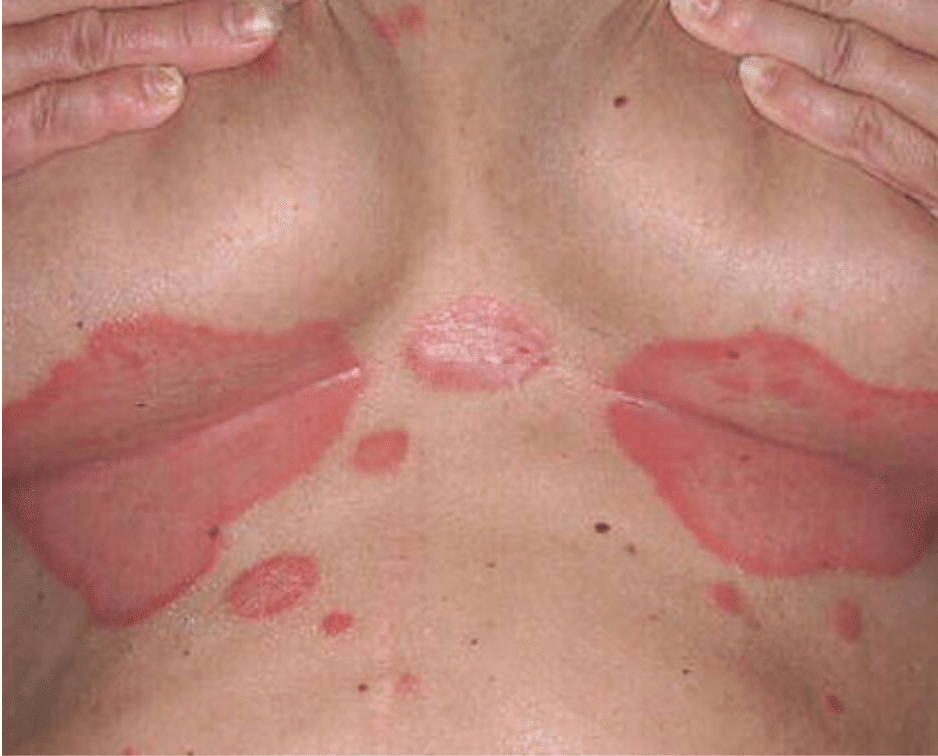
Inverse psoriasis. Image source.
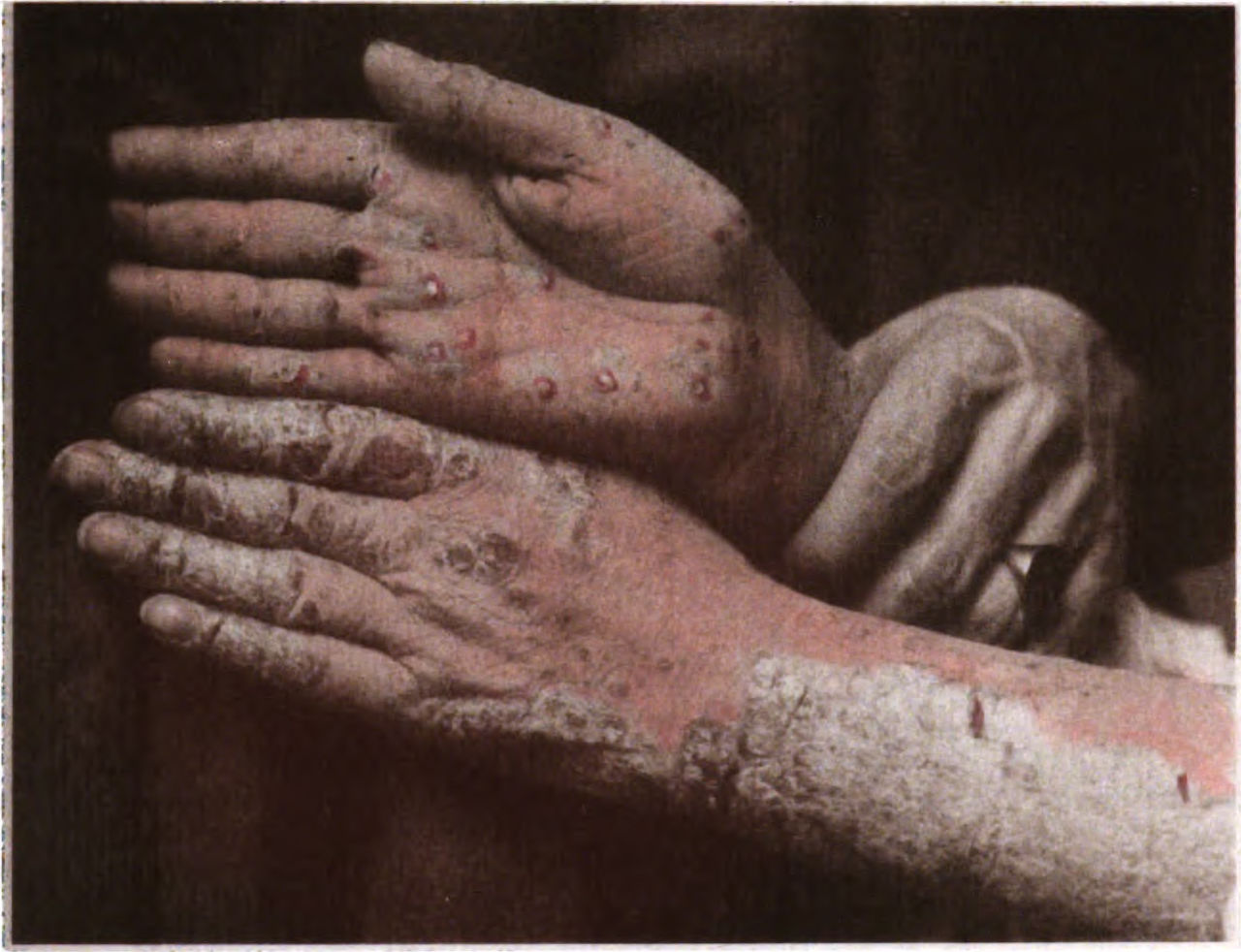
Pustular psoriasis. Image source.
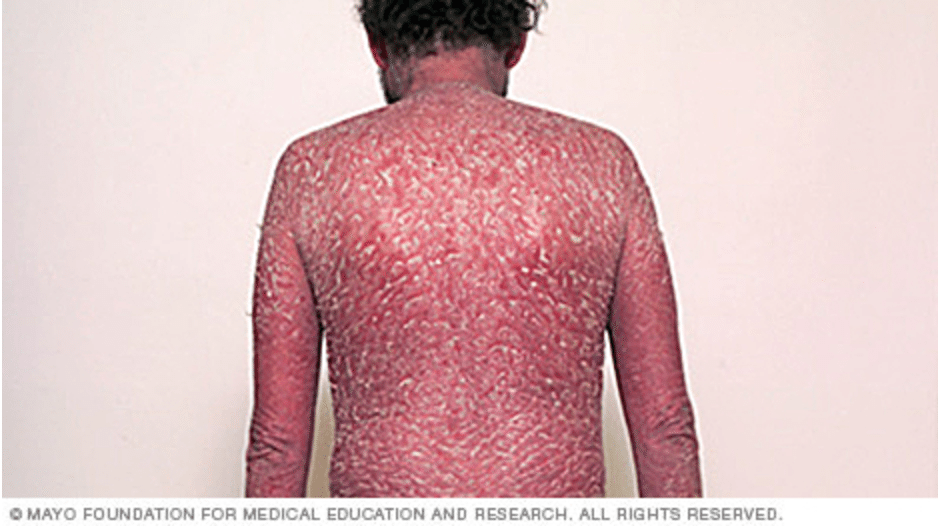
Erythrodermic psoriasis. Image source.
Summary: Psoriasis is a chronic condition that causes distinctive skin rashes, itching, inflammation, and pain. Symptoms occur in flares.
Psoriasis Causes

Psoriasis is caused by a combination of genetic, environmental, and immunological factors (3).
One large study found that a person’s risk increases up to 65% if their parents have psoriasis, and up to 83% if both their parents and siblings have it (4).
Not everyone who carries the gene will develop psoriasis. However, exposure to certain environmental stimuli may increase a person’s likelihood of developing the disease.
These stimuli include:
- Emotional stress (5).
- Certain infections, including strep throat (6).
- Some medications, including antihypertensives, beta-blockers, antipsychotics, antimalarial drugs, and nonsteroidal anti-inflammatory drugs (7, 8, 9).
- Lifestyle factors, including obesity, alcohol consumption, and smoking (10, 11, 12).
In the presence of both environmental and genetic factors, the immune system malfunctions.
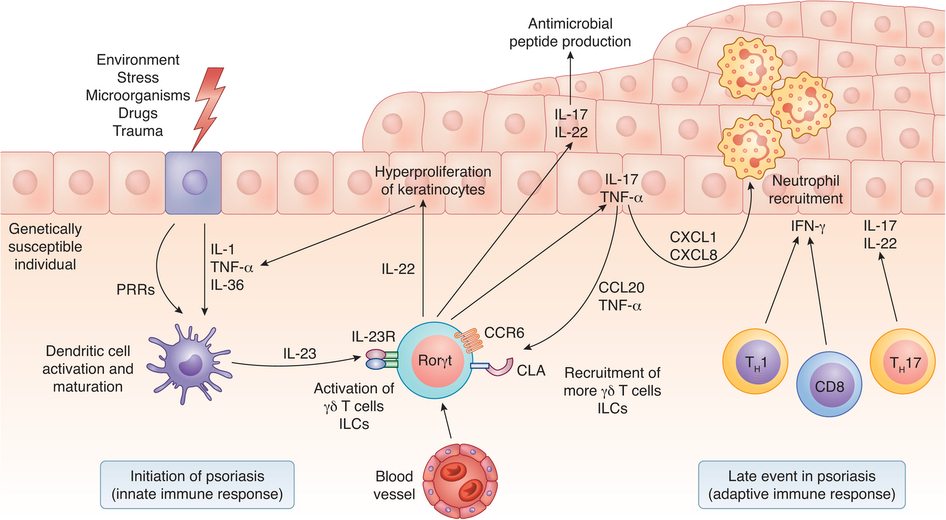
T cells, which normally respond to infection and injury, are mistakenly activated as a result. These cells recruit other immune cells and trigger the release of inflammatory cytokines (13).
This causes the skin cells to die off and regenerate more quickly than they should.
Onset of psoriasis. Image source. Click to enlarge.
The same environmental factors that cause psoriasis can also lead to flares, so it’s best to limit exposure to them when possible.
Summary: Psoriasis occurs when the immune system mistakenly attacks healthy skin cells. Many people carry a gene for the disease and develop it after exposure to certain environmental factors.
Diet and Psoriasis Treatment
The standard treatments for psoriasis involve topical and oral medications, as well as ultraviolet light therapy.
There is no scientific proof that diet is an effective treatment for psoriasis on its own.
However, patient testimonials and studies have shown certain diet strategies may help relieve psoriasis symptoms, especially when combined with traditional therapies.
The following sections will focus on foods and nutrients that affect psoriasis severity.
Achieve and Maintain a Healthy Body Weight

Overweight (in a clinical setting) is characterized by a body mass index (BMI) greater than 24.9.
A BMI greater than 29.9 is classified as obese.
Many studies have found a possible link between obesity and psoriasis.
In one long-term study of more than 67,000 females (14):
- Women with a BMI of 25.0-29.9 were up to 21% more likely to have psoriasis than women with a healthy BMI.
- Women with a BMI of 30.0-34.9 were up to 63% more likely to have psoriasis than women with a healthy BMI.
- Women with a BMI greater than 35 were up to 103% more likely to have psoriasis than women with a healthy BMI.
Even weight gain of just 10 pounds (4.5 kg) appears to increase risk by up to 8%, regardless of BMI classification (15).
In addition to risk, obesity is also linked to disease severity. This is likely because excessive fat tissue increases production of inflammatory cytokines, which contribute to inflammation and lesions in psoriasis (16, 17).
It makes sense then that studies have shown that calorie restriction paired with medication is more effective in reducing psoriasis symptoms than medication alone (18).
Notably, most studies on obesity and psoriasis are observational. This means that researchers aren’t exactly sure if obesity causes the disease or vice versa.
In any case, psoriasis is linked with several other heart disease risk factors, including high cholesterol, diabetes, and high blood pressure.
Weight loss can reduce heart disease risk for people who are overweight or obese, so it makes sense to maintain a healthy weight (17).
You can calculate your BMI here.
Summary: Those who are very overweight are more likely to have psoriasis, although researchers aren’t sure if obesity causes it directly. Maintaining a healthy bodyweight also lowers risk of heart disease which is more common in psoriasis patients.
The Autoimmune Protocol, Gluten, and Alcohol
The autoimmune protocol (AIP) is a diet that eliminates gluten, soy, dairy, legumes, grains, added sugars, nightshades, and alcohol for at least 30 days.
The goal is to identify foods that trigger undesirable autoimmune reactions.
There’s a strong link between psoriasis and other autoimmune diseases. In one large study, those with psoriasis had higher rates of 14 different autoimmune disease than the general population (19).
Patient testimonials suggest that the AIP is helpful for many conditions, including psoriasis.
There have been no clinical trials on the AIP, so there’s no scientific evidence to support it. But certain foods eliminated in the AIP—including gluten and alcohol—have been reported to worsen psoriasis symptoms.
Some small studies have shown a gluten-free diet to improve psoriasis symptoms, but only in those with antibodies against gliadin (a protein found in gluten). These antibodies would be seen in those with celiac disease or non-celiac gluten sensitivity (20).
Although other studies found no benefits at all, so it’s all quite unclear at this stage (19).
A stronger link has been suggested between alcohol intake and psoriasis severity.
One review of 28 studies found that alcohol is likely a risk factor for developing psoriasis, and that those with the disease drink more than healthy adults (11).
It’s best to avoid alcohol if you have psoriasis, or a strong family history of it.
Summary: Patient testimonials suggest that the autoimmune protocol may help with psoriasis, but this hasn’t been formally studied. You should definitely avoid alcohol and potentially gluten too if you are sensitive.
Anti-Inflammatory and Mediterranean Diets

A Western diet high in fat, sodium, and added sugars has been linked to inflammation and autoimmune disease (21).
For this reason a so-called anti-inflammatory diet may ease psoriasis symptoms.
There’s no universal definition for anti-inflammatory diet, but it generally refers to a style of eating that (22, 23, 24):
- is moderate in calories.
- has a favorable ratio of omega-3 to omega-6 fatty acids.
- identifies and eliminates foods that cause sensitivities.
- limits red and processed meats.
- reduces added sugar.
- emphasizes fruits, vegetables, and whole grains.
- eliminates trans fats.
An anti-inflammatory diet hasn’t been studied in psoriasis specifically, but systemic inflammation is a key feature of the disease.
This diet pattern has also been shown to help with certain autoimmune diseases, so in theory and based on patient testimonials it may be beneficial (18, 25, 26).
Patient testimonials also indicate that an anti-inflammatory eating pattern is helpful for arthritis. As such, it may be useful for relieving pain and stiffness in those with psoriatic arthritis (27, 28).
The diet is similar in many ways to the Mediterranean diet, which includes fish and lean meats, vegetables, fruits, healthy fats, whole grains, and legumes.
In one study, stronger adherence to the Mediterranean diet was associated with fewer psoriasis symptoms. Further, those with fewer symptoms ate more fruit, vegetables, legumes, nuts, and fish and less meat (29).
More human studies are needed to know if the Mediterranean diet is beneficial for psoriasis. But given its other health benefits, such as reducing heart disease risk, it makes sense to eat this way regardless of its effects on skin (30).
Summary: Anti-inflammatory and Mediterranean diets emphasize healthy fats, fruits, vegetables, and whole grains. One study linked the Mediterranean diet with improved psoriasis symptoms.
Supplements for Psoriasis
Several dietary supplements have been reported to help with psoriasis treatment.
Fish Oil

Fish oil capsules contain the omega-3 fatty acids eicosapentaenoic acid (EPA) and docosahexanoic acid (DHA).
It’s known for its anti-inflammatory properties.
In one literature review, 12 of 15 studies found fish oil to improve psoriasis severity (31).
The strongest evidence is in support of high-dose intravenous (IV) omega-3 infusions for plaque and guttate psoriasis. However, this isn’t a typical therapy, and wouldn’t be readily available to most patients (32, 33).
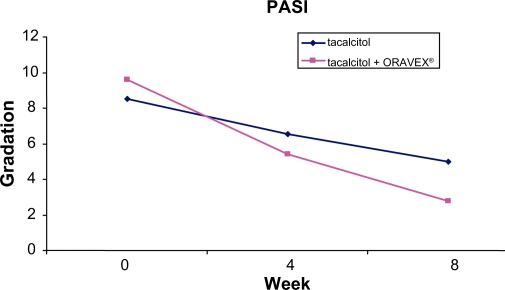
One small observational study found that oral fish oil supplements significantly reduced psoriasis severity and improved quality of life when paired with prescription ointment. Volunteers in this study received 640 mg of DHA plus EPA per day for eight weeks (34).
Change in Psoriasis Area and Severity Index (PASI) over duration of study for fish oil plus ointment group compared to ointment only group. Lower score is better. Click to enlarge.
Larger clinical trials are needed to confirm these effects but it looks promising.
Probiotics
Probiotics are beneficial bacteria that we eat.
They have been the focus of many studies recently because of the interaction between the gut microbiota and various health conditions, including psoriasis.
One study found adults with psoriasis—especially psoriatic arthritis—to have less diversity in gut bacteria than healthy adults. The researchers likened the bacterial profile in psoriasis to that of inflammatory bowel disease, which often responds well to probiotics (35, 36).
In another study, 23 patients with mild to moderate plaque psoriasis received the probiotic Bifidobacterium infantis 35264 at a dose of 1×1010 colony forming units (CFU) per day for eight weeks.
Researchers found that most blood markers of inflammation (CRP and TNF-α) were significantly lower at eight weeks (37).
Other probiotic strains haven’t been studied specifically in psoriasis yet.
Vitamin D

Vitamin D helps regulate the immune system by inhibiting T cell multiplication and limiting cytokine production (38).
Because T cells and cytokines play key roles in psoriasis, and because vitamin D deficiency is common among those with autoimmune disease, it’s been studied as a possible psoriasis treatment (38).
One literature review found vitamin D supplements and ointments to be as effective as corticosteroids in easing symptoms. The benefits were even greater when vitamin D was used with a high-dose steroid ointment (39).
In one study, 85 psoriasis patients began taking 0.5 micrograms (μg) of oral calcitriol (the active form of vitamin D3) per day. Researchers increased the daily dosage by 0.5 μg every two weeks, as long as lab tests were normal. Volunteers received treatment for between 6-36 months.
Patients saw significant reductions in Psoriasis Area and Severity Index (PASI) scores at six months and even greater improvements at 24 months. Nearly 27% had complete improvement in symptoms, while 88% had some improvement (31, 40).
The results are promising, and no negative side effects were reported.
But high quality clinical trials are needed to make firm conclusions.
Antioxidants
Antioxidants are molecules that protect cells against oxidative stress.
A handful of studies have linked oxidative stress and psoriasis, and certain antioxidants have been proposed as a supplemental therapy for the disease (41, 42).
Selenium
Selenium is an antioxidant mineral found in vegetables, meat, fish, poultry, grains, and eggs.
Evidence is conflicting as to whether selenium deficiency directly contributes to psoriasis risk (43, 44).
Small studies, however, have found that it may play an indirect role. Selenium helps inhibit activity of a protein called osteopontin, and high osteopontin levels are thought to increase psoriasis risk (45, 46).
It’s unclear whether selenium supplements are helpful in reducing symptoms though.
In one study of 58 psoriasis patients, supplementation with 48 μg of selenium per day decreased symptom severity quicker and more significantly than placebo. Unfortunately, it’s difficult to know how much of a role selenium played in the improvement, as the capsules also included coenzyme Q10 and vitamin E (47).
Other studies have shown selenium supplements to be equal or inferior to placebo, so it’s unclear if they are useful (48, 49).
Curcumin
Curcumin is the main chemical compound in the spice turmeric.
It’s said to have strong anti-inflammatory properties, and patient testimonials suggest that it’s helpful in psoriasis.
However, rodent studies and small human trials have found mixed results in terms of symptom improvement (50, 51).
Additionally, a recent review cautioned that the benefits of curcumin may be overstated. In fact, the researchers raised concerns that the compound may mask inflammation rather than treating it (52).
In short, there’s no currently strong evidence in support of curcumin for psoriasis.
Quercetin
Quercetin is a flavonoid antioxidant that’s found in many fruits and vegetables.
One study conducted on mice found that 25 to 50 grams of quercetin per kilogram of body weight significantly reduced skin thickness and inflammation and increased production of healthy skin cells (53).
It’s not known how quercetin affects psoriasis activity in humans though. In fact, recent human studies have questioned the antioxidant power of dietary flavonoids in general.
Quercetin and other flavonoids are poorly absorbed, which indicates that other factors may contribute to its antioxidant action (54).
At this stage it seems quercetin will not help with psoriasis.
Always speak with your doctor before beginning any supplement.
Summary: Of the many supplements that may help with psoriasis, fish oil, probiotics, and vitamin D show the most promise. They’re generally considered safe, but you should always speak with your doctor before beginning supplements.
Psoriasis Treatment: The Punch Line
No diet or pill can cure psoriasis.
However, certain eating patterns and supplements have been reported to help ease symptoms.
Research shows it’s important to achieve and maintain a healthy body weight, as being overweight or obese is linked with greater risk for psoriasis and greater severity in symptoms.
Patient testimonials indicate the autoimmune protocol (AIP) may help, but it has not been formally studied. Certain guidelines from the AIP are beneficial though, like avoiding gluten if you’re sensitive and eliminating alcoholic beverages.
Alternatively, an anti-inflammatory diet such as the Mediterranean diet has shown promise in reducing disease severity. This eating pattern has many other known benefits and is strongly recommended.
Some evidence suggests that supplemental fish oil, vitamin D, and a particular probiotic strain helps reduce symptoms too. Stronger studies are needed, but these supplements are generally well-tolerated.
Always ask your doctor before beginning any new supplements.







I had Psoriasis as a teenager and for over 20 years. It was horrible having to feel self-conscious and in pain every second of the day. But I took matters into my own hands. Got off all medications and followed natural healing with psoriasis diet and I am happy to say I am a Psoriasis Warrior, clear now for over 2 years.