More than half of all people over the age of 60 have diverticulosis. Most of them have absolutely no idea.
Not because they haven’t been paying attention. Not because they’ve been eating badly. But because nobody told them. And in many cases — including cases we see regularly in our clinic — their own doctor doesn’t explain what’s happening inside their gut, why, or what it means for their future.
In this article, I’m going to explain the five things that most people are never told about how diverticulosis actually develops. And one of them (I’ll save it for last) is something that even the medical research is only just starting to figure out. It might be the most important one of all.
Please keep in mind that this is educational information only and not direct medical advice for your specific situation.
Here is a video we made; there is also a written version underneath.
What is Diverticulosis?
Before we get into it, one important distinction worth making: diverticulosis and diverticulitis are not the same thing.
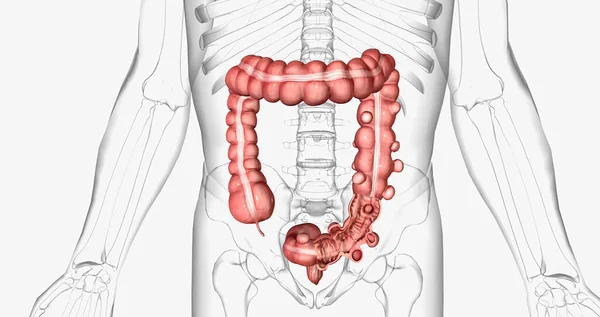
Diverticulosis is the condition of having small pouches — called diverticula — that have formed in the wall of your large intestine. It’s structural. Most people with diverticulosis have zero symptoms. They don’t know they have it.
Diverticulitis is what happens when one or more of those pouches becomes inflamed or infected. That’s when you get the pain, the fever, the hospital visit.
This article is about diverticulosis — how those pouches form in the first place. Because if you understand that, you understand why some people progress to diverticulitis, and others don’t — and what you can actually do about it.
Point #1: It’s Almost Always Completely Silent
The first thing most people are never told is this: diverticulosis develops with no symptoms whatsoever.
The pouches form over years — sometimes decades — with no pain, no warning, and no indication that anything is happening. The vast majority of people find out one of two ways: either during a colonoscopy done for a completely different reason, or the hard way — when a flare-up lands them in the emergency room.
A 2024 study followed 684 people who went in for a routine screening colonoscopy. 42% of them had diverticulosis. Most had no idea going in. And the prevalence climbs with age — by the time you’re in your 60s, you’re looking at more than one in two people. Over 70, it’s even higher (1).
This matters because the window to intervene — to slow the progression, to prevent flares — is often happening silently. People don’t start thinking about their gut health until they’re already in pain. And by then, the structural change has already happened.
Summary: Diverticulosis is almost always asymptomatic, forming silently over years or decades. Most people only discover it during an unrelated colonoscopy or after their first painful flare. The window to intervene is open long before symptoms appear — which is why awareness matters so much.
Point #2: It’s Not Random — There Are Specific Weak Points
Most people assume diverticula form randomly throughout the colon, like a wall developing cracks in unpredictable places. That’s not what happens.
Diverticula form at very specific structural weak points: the places where tiny blood vessels called the vasa recta penetrate through the muscular wall of the colon.
Think of it like a bicycle tyre. A tyre doesn’t blow out anywhere — it blows out at the thin spots, the places where the rubber is already a little weaker. Your colon works the same way. Those entry points for blood vessels are the thinnest parts of the wall. Under enough pressure, over enough time, that’s where the pouches push through.
This is why in Western countries, diverticulosis almost always occurs in the descending and sigmoid colon — the lower left section. That’s where those weak points are concentrated. Interestingly, in Asian populations, the distribution is different — more right-sided — which tells us genetics plays a role too. We’ll come back to that (2).
The key point: this isn’t random degradation. It’s a structural vulnerability that every human colon has, responding to pressure that builds over time.
Summary: Diverticula don’t form randomly. They push through at predictable structural weak points where blood vessels enter the colon wall. Understanding this helps explain why the condition is so common, and why pressure management — not just diet — is central to prevention.
If you’re just getting started, download our low FODMAP Food List Guide to get clarity on common food triggers
Tap the blue button below to download our “Eat This, Not That” list as well as additional resources for Diverticulitis (it’s free!)

Point #3: “Eat More Fiber” Is Correct But Dangerously Incomplete
If you’ve been diagnosed with diverticular disease, you’ve heard this advice. And it’s not wrong. But it explains about 20% of what’s actually happening and leaves out the other 80%, which is why people follow it and still get flares.
Here’s the actual mechanism. When you don’t eat enough fiber, your stool has less bulk. Less bulk means your colon has to work harder to move it. Harder work means more pressure with each peristaltic contraction — each squeeze of the colon wall. That increased pressure pushes against those weak points, and over time, the wall gives way (3).
So “eat more fiber” is right — but it describes the endpoint of a mechanical process, not the full picture. And here’s where it gets more complicated: many high-fiber foods are also high in FODMAPs, which in people with a sensitive or already-inflamed gut can trigger symptoms and make things significantly worse. The advice, applied without context, can actually cause problems for the very people it’s meant to help.
We see this constantly in our clinic. People come to us having dutifully added fiber — bran, legumes, onions, wheat — and they feel worse, not better. They’re not doing anything wrong. They just don’t have the context to understand which fiber, how much, and introduced in what order.
That’s exactly the situation our client Janice was in. She’d been told to eat more fiber for years. Every time she tried, she’d flare. She came to us, went through a structured Low FODMAP protocol, and for the first time understood what her gut could and couldn’t handle. She now manages her condition without fear of what she eats.
The fiber advice isn’t wrong. It’s just dangerously incomplete.
Summary: Low fiber intake increases colon pressure, which drives pouch formation — so the advice to eat more fiber is mechanically correct. But many high-fiber foods are also high-FODMAP, meaning they can worsen symptoms in people with a sensitive gut. Understanding which fiber, how much, and when to introduce it is what actually makes the difference.
Point #4: Your Genes Have More to Do With This Than You Think
Here’s something that rarely comes up in a GP’s office: diverticulosis isn’t just about what you eat. Your genetics play a significant role.

Research confirms that diverticula form from a complex interaction of genetic factors, changes in colonic motility — how well your colon moves — and lifestyle factors including diet, smoking, obesity, and alcohol intake (4).
This is why you’ll see people who have eaten well their entire lives develop diverticulosis. And why you’ll see people who eat poorly and never develop it. Genetics loads the gun. Your lifestyle and diet influence whether the trigger gets pulled, and how fast.
What does this mean practically? It means if a parent had diverticular disease, you should be paying attention earlier. It means blaming yourself for developing diverticulosis misses the point entirely. And it means the solution isn’t as simple as adding a fiber supplement — it’s understanding your individual risk profile, which looks different for every person.
We’re not all working with the same colon. Context matters enormously.
Summary: Genetics plays a significant and underacknowledged role in diverticulosis. The condition develops through an interaction of inherited factors, gut motility, and lifestyle — which is why diet alone doesn’t explain every case. A family history of diverticular disease is a meaningful risk factor worth discussing with a specialist.
Point #5: A 2024 Microbiome Discovery That Changes Everything
Now for the one worth saving until last. This is genuinely new science — and most GPs are not yet aware of it.
In 2024, researchers published what they described as the first large-scale evidence of measurable changes in gut microbiome composition in people with asymptomatic diverticulosis (5).
Meaning: even before any symptoms appear, even when you feel perfectly fine, the community of bacteria living in your gut is already measurably different if you have diverticulosis compared to someone who doesn’t.
Specifically, people without diverticulosis had higher levels of beneficial bacteria. People with diverticulosis showed different bacterial profiles — shifts that appear to influence inflammation and gut wall integrity.
What this tells us is that diverticulosis isn’t just a mechanical problem of pouches under pressure. It’s also a microbial environment problem. Your gut bacteria are part of what determines how the colon wall behaves, how inflamed it is, and how resilient it is under that pressure.
This is why simply eating more fiber or taking a generic probiotic off the shelf doesn’t fix the underlying picture. You can change what you eat without changing what’s living in your gut. And if the microbial environment is already shifted — which this research suggests it is, even before symptoms appear — you’re treating the surface while ignoring the ecosystem.
Summary: A landmark 2024 study found measurable differences in gut microbiome composition in people with diverticulosis — even before any symptoms appeared. This positions diverticulosis not just as a structural or dietary issue, but as a microbial environment problem. Addressing the bacterial ecosystem, not just fiber intake, is increasingly central to effective management.
Bonus: What the Research Actually Admits
One more thing, and it may be the most important thing in this entire article.
A 2024 paper published in Nature Communications — one of the most prestigious scientific journals in the world — opened with this statement: the cause and mechanism of diverticulitis remains largely unknown (6).

This is 2024. Diverticulitis sends over 300,000 people to hospital in the US every single year. And the exact reason why some people’s pouches become inflamed while others don’t — science doesn’t fully know yet.
So when your doctor says “just watch it and call me if you have a flare” — they’re not being dismissive. They’re working with the same uncertainty the research reflects. The conventional medical system doesn’t have a complete answer. Which is precisely why a reactive approach — waiting for a flare, treating it with antibiotics, waiting for the next one — isn’t the right strategy.
The same paper found something else worth noting: your microbial composition actually influences how protective your diet is. Two people can eat the same fiber-rich diet, and one gets significantly more protection from diverticulitis than the other — because of what’s living in their gut.
You can’t separate the diet from the ecosystem it’s operating in. And that’s exactly why personalised, root-cause care changes everything for people with diverticular disease.
Summary: Even in 2024, the exact mechanism behind why diverticulosis progresses to diverticulitis remains incompletely understood. A reactive, symptom-management approach is limited by this uncertainty. Emerging research suggests that gut microbiome composition directly influences how protective diet is — making personalized, root-cause assessment the most effective long-term strategy.
What Should Your Next Steps Be?
If you’re feeling overwhelmed navigating treatment, diet, recovery, and prevention on your own, professional guidance can make all the difference. At Diet vs. Disease, we specialize in diverticular disease and have helped thousands of patients build a more resilient gut through an individualized, holistic approach.
To learn more about our integrated approach, I invite you to apply for a nutrition assessment call with us. We’ll help you make sense of what’s really happening and map out the next steps to get you feeling confident again — not just temporarily avoiding symptoms, but addressing the root cause and fixing your gut issues for good.

Leave a Reply